| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Drug induced Lupus Erythematosus
Related Subjects: |Systemic Lupus Erythematosus (SLE) |Drug induced Lupus Erythematosus |Discoid lupus erythematosus (DLE) |Neonatal Lupus Erythematosus |Raynaud's Phenomenon |Polymyositis |Dermatomyositis |Polyarteritis nodosa |Rheumatoid Arthritis |Systemic Sclerosis (Scleroderma) |Rheumatology Autoantibodies |Overlap Syndrome |Inclusion Body Myositis |Inflammatory Myopathies |Psoriatic Arthritis |Adult Onset Still's Disease |Alkaptonuria |Behcet's Syndrome
💊 Drug-induced lupus erythematosus (DILE) is an autoimmune condition caused by a reaction to certain medications. ⚠️ It tends to be more benign than idiopathic SLE, with rare renal, skin, or neurological involvement.
🧬 About
- Resembles systemic lupus erythematosus but usually milder.
- Key distinction: renal, neurological, and cutaneous involvement is uncommon.
- Improves after withdrawal of the offending drug.
⚖️ Risk Factors
- Older age group compared with classic lupus.
- Pharmacogenetics: slow acetylator status.
- Genetic predisposition: HLA DR4, DR2, DR3, DR0301, DQB1, B8, C4 null allele.
💊 Common Culprit Drugs
- High yield: Isoniazid, Procainamide, Hydralazine, Penicillamine, Phenytoin.
- Biologics: TNF-α inhibitors (etanercept, infliximab, adalimumab).
- Other causes: Minocycline, Quinidine, Methyldopa, Chlorpromazine, Sulfasalazine, Capoten (captopril).
- Levamisole-adulterated cocaine – increasingly recognised cause.
🩺 Clinical Features
- Onset: usually after 3–6 months of therapy (sometimes up to 10 years).
- Systemic: fever, malaise, weight loss.
- MSK: polyarthritis or migratory arthralgia (often symmetrical).
- Serositis: pleuritis or pericarditis.
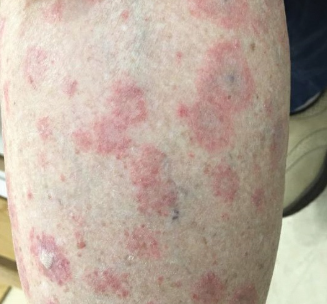
- Skin: annular or papulosquamous lesions on sun-exposed areas (less severe than idiopathic SLE).
🔬 Investigations
- FBC & U&E: usually normal.
- Complement (C3/C4): usually normal (contrast with SLE where low).
- ANA: positive in ~90% (homogeneous pattern).
- Anti-dsDNA: typically negative.
- Anti-histone antibodies: positive in >95% of DILE cases – hallmark test.
- ESR: may be raised.
🛠️ Management
- 🚫 Stop the causative drug – symptoms usually resolve within weeks to months.
- NSAIDs or low-dose steroids for symptomatic relief in persistent arthritis/serositis.
📊 Exam Tip – DILE vs SLE
| Feature | Drug-Induced Lupus | Systemic Lupus (SLE) |
|---|---|---|
| Age | Older | Younger (esp. women of childbearing age) |
| Time course | Months–years after exposure | Chronic/relapsing |
| Renal/CNS involvement | Rare | Common |
| ANA | Positive, homogeneous | Positive, mixed patterns |
| Anti-dsDNA | Negative | Positive (specific) |
| Anti-histone | Positive in >95% | Positive in 50–70% |
| Management | Stop drug → resolution | Immunosuppression needed |
📚 References
Cases - Drug-Induced Lupus Erythematosus (DILE)
- Case 1 - Hydralazine-related 💊: A 54-year-old man on long-term hydralazine for resistant hypertension develops fatigue, arthralgia, low-grade fever, and a photosensitive rash. Bloods: ANA positive, anti-histone antibody positive, normal complement levels. Diagnosis: drug-induced lupus from hydralazine. Symptoms improve on drug withdrawal.
- Case 2 - Procainamide-associated ❤️: A 61-year-old woman treated with procainamide for atrial fibrillation presents with pleuritic chest pain and arthralgia. Exam: small pleural effusion. Autoantibodies: anti-histone strongly positive, dsDNA negative. Diagnosis: drug-induced lupus from procainamide. Managed with discontinuation and NSAIDs.
- Case 3 - Anti-TNF induced 🌐: A 45-year-old man with rheumatoid arthritis on infliximab reports photosensitive rash, oral ulcers, and joint pains. ANA and anti-dsDNA are positive, but disease resolves after stopping the drug. Diagnosis: anti-TNF–induced lupus-like syndrome. Managed with drug cessation and short steroid course.
Teaching Point 🩺: DILE resembles SLE but usually spares the kidneys and CNS. Hallmarks are exposure to culprit drugs (hydralazine, procainamide, isoniazid, minocycline, anti-TNF agents), positive ANA/anti-histone antibodies, and resolution after withdrawal.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
