Related Subjects:Migraine
|Basilar Migraine
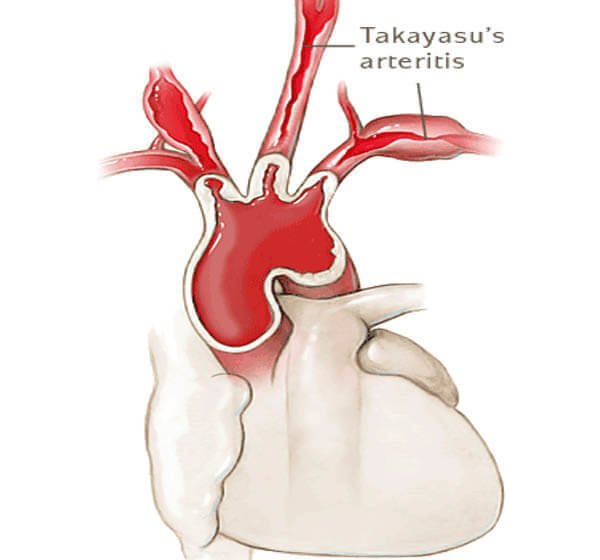
|Takayasu arteritis (pulseless disease)
⚠️ Takayasu’s arteritis = "Pulseless disease" → think of a young woman (<40), weight loss, malaise, absent pulses, and raised ESR.
The hallmark is granulomatous inflammation of the aorta and its major branches, leading to stenosis, occlusion, or aneurysm formation.
📖 About
- Chronic inflammatory large-vessel vasculitis of unknown origin.
- Median age of onset = 29 years; women are affected 8× more than men.
- Highest prevalence in Asia & Africa, less common in Europe/North America.
🧬 Pathophysiology
- Active inflammatory phase: Granulomatous aortitis ± branch vessel involvement.
- Sclerotic phase: Intimal hyperplasia + medial degeneration → stenosis/occlusion.
- Lesions are usually stenotic, though aneurysms may occur.
🩸 Affected Vessels
- Mainly the aorta and primary branches.
- Common sites = aortic arch, subclavian, renal, and carotid arteries.
- Pulmonary artery may also be affected.
🧑⚕️ Clinical Features
- Constitutional: fatigue, fever, night sweats, weight loss, arthralgia, headache.
- Vascular insufficiency signs:
- Upper/lower limb claudication
- Absent pulses → “pulseless disease”
- BP difference >10 mmHg between arms
- Bruits over subclavian / abdominal aorta
- Complications:
- Renal artery stenosis → hypertension
- Aortic regurgitation → heart failure
- Coronary involvement → angina/MI
- Carotid disease → TIA/stroke
- Mesenteric ischaemia → abdominal angina
🧪 Laboratory Findings
- ↑ ESR & CRP (active inflammation)
- Anaemia of chronic disease
- Mild leukocytosis
- Hypergammaglobulinaemia
📋 Diagnostic Criteria (Arend et al., 1990)
|
≥3 of the 6 → Sensitivity 90.5%, Specificity 97.8%
|
|---|
| 1 | Age at onset <50 years |
| 2 | Claudication of extremities |
| 3 | Decreased brachial artery pulse |
| 4 | Systolic BP difference >10 mmHg between arms |
| 5 | Bruit over subclavian arteries/abdominal aorta |
| 6 | Arteriographic narrowing/occlusion of aorta or primary branches |
🔍 Diagnosis
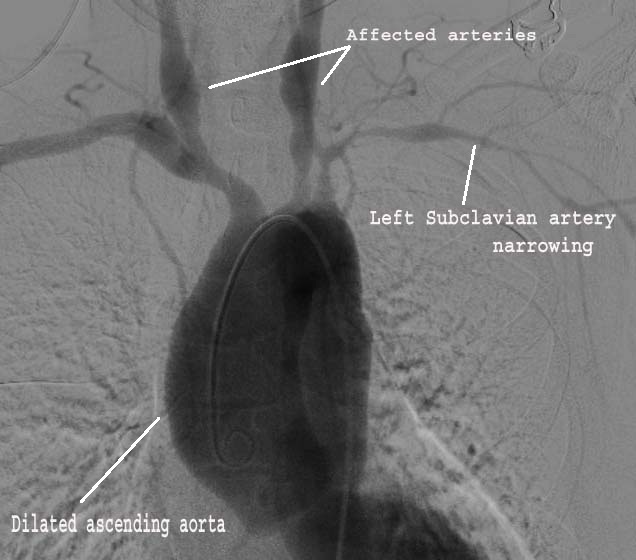
Imaging is essential → demonstrates stenosis, occlusion, or aneurysm.
- Aortography
- CT Angiography
- MR Angiography (non-invasive, preferred for follow-up)
💊 Treatment
- Corticosteroids: Prednisone 60–100 mg/day in active phase.
- If steroid-refractory → immunosuppressants (e.g. Methotrexate, Azathioprine, Mycophenolate).
- Biologics: Tocilizumab (IL-6 inhibitor) effective in resistant disease.
- Intervention:
- Balloon angioplasty → for short stenoses (high restenosis risk).
- Surgical bypass/reconstruction → avoid during active inflammation.
📊 Prognosis
- ~50% relapse within 10 years.
- 15-year survival: ~85% overall, but ↓ to 65% if major vascular complications.
- Leading causes of death = stroke, MI, heart failure.