| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Leishmaniasis (Cutanenous and Visceral)
The risk of infection is highest from dusk to dawn, when sand flies are most active. Amphotericin B is now the treatment of choice due to rising resistance to pentavalent antimonials.
📖 About
- Three major forms: Cutaneous (CL), Mucocutaneous (MCL), and Visceral (VL).
- Spread by infected sand flies:
- Lutzomyia species in the New World.
- Phlebotomus species in the Old World.
- Protozoan parasites of the Leishmania family.
- Endemic in Central/South America, Africa, India, Middle East, Asia, Southern Europe, and the Mediterranean.
🧬 Mechanism of Infection
- Inoculated promastigotes are phagocytosed by macrophages.
- They transform into amastigotes, multiply by binary fission, and evade nitric oxide killing.
- Rupture of infected macrophages → spread to other cells in the reticuloendothelial system.
🦟 Transmission
- Vector: infected sand flies living in mud huts and rural dwellings.
- Peak biting activity: evening, twilight, and night.
- Sand fly bites are silent and painless; lesions may go unnoticed until ulcers appear weeks to months later.
- Lesions may cause scarring; mucosal disease can lead to nasal destruction.
- Regional lymphadenopathy or lymphangitis may accompany skin lesions.
🩺 Clinical Manifestations
- Cutaneous Leishmaniasis (CL)
- Geography: Mexico, Central/South America, Middle East, Asia, N. Africa, Southern Europe.
- Parasites multiply in dermal macrophages near inoculation site → nodules/ulcers on arms, legs, face, ears.
- Classic ulcer: painless, chronic, may be called the “Baghdad boil”.
- May be mistaken for leprosy.
- Diagnosis: slit skin smear from raised ulcer edge or nodule centre (shows amastigotes).
- Mucocutaneous Leishmaniasis (MCL)
- Mainly in South America.
- Causes destructive lesions of nose, nasopharynx, palate, uvula, larynx, and upper airways.
- Visceral Leishmaniasis (VL, “Kala-azar”)
- Most severe form; frequently fatal if untreated.
- Caused by L. donovani, L. infantum, L. chagasi.
- Incubation up to 2 years (usually 8 months).
- Dissemination via macrophages → reticuloendothelial system.
- Symptoms: prolonged fever, weight loss, massive splenomegaly > hepatomegaly, pancytopenia.
🔍 Investigations
- FBC: anaemia, leucopenia, thrombocytopenia; low albumin, raised globulins.
- Diagnosis:
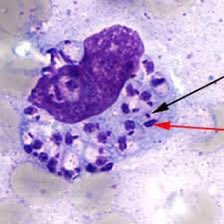
- Amastigotes (Leishman-Donovan bodies) on bone marrow aspirate.
- Tissue scraping: amastigotes within macrophages.
- Splenic aspirate (if safe: INR normal, platelets >40) – very sensitive.
- Consider co-infections: TB, dysentery, pneumonia; advanced disease predisposes to cancrum oris.
- Note: treated patients may later develop Post-kala-azar dermal leishmaniasis (PKDL), remaining reservoirs of infection.
💊 Management
- Amphotericin B is the treatment of choice (liposomal form preferred where available).
- Miltefosine or paromomycin may be used as alternatives in some regions.
- Cutaneous lesions: may heal spontaneously but can require antimonials, amphotericin, or cryotherapy depending on severity.
- Supportive care: treat malnutrition, secondary infections, and anaemia.
🛡️ CDC Advice (Prevention)
- Stay in screened/air-conditioned rooms; avoid outdoor activities from dusk to dawn.
- Wear protective clothing (long sleeves, trousers, socks, tucked-in shirt).
- Apply insect repellents with DEET (30–35% for adults; ≤10% for children aged 2–6; avoid in <2 years).
- Spray clothes with permethrin-containing insecticides; reapply after washing.
- Spray rooms with insecticides; sand flies are highly susceptible.
- Use fine-mesh bed nets (≥18 holes per inch), ideally treated with permethrin.

🧾 Clinical Case Reports – Leishmaniasis
Case 1 – Cutaneous Leishmaniasis 🩹 A 28-year-old soldier returns from the Middle East with a slowly enlarging ulcer on his forearm. The lesion has a raised border and central crust but is painless. Skin biopsy shows amastigotes of Leishmania major. 👉 Diagnosis: Cutaneous leishmaniasis. 👉 Management: Local wound care and intralesional antimonials; spontaneous healing possible but scarring likely.
Case 2 – Visceral Leishmaniasis (Kala-azar) 🌙 A 6-year-old boy from rural India presents with fever, weight loss, massive splenomegaly, and pancytopenia. Bone marrow aspirate confirms Leishmania donovani. 👉 Diagnosis: Visceral leishmaniasis. 👉 Management: Liposomal amphotericin B, nutritional support, and monitoring for relapse.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
