| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Abdominal Pain in Adults
Related Subjects:Acute Cholecystitis |Acute Appendicitis |Chronic Peritonitis |Abdominal Aortic Aneurysm |Ectopic Pregnancy |Acute Cholangitis |Acute Abdominal Pain |Penetrating Abdominal Trauma |Abdominal Masses: Clinical Approach and Considerations |Abdominal Distension |Vomiting |Substance Misuse |Cannabinoid Hyperemesis Syndrome (CHS) |Cyclical Vomiting Syndrome
Acute abdominal pain accounts for ~5–10% of emergency department visits. Approximately 15–25% of cases require surgical intervention. The goal is rapid identification of surgical emergencies while avoiding unnecessary operations.
✅ Key Clinical Advice
- Always assess and stabilise with ABCDE before focusing on diagnosis.
- In unstable patients → urgent surgical review, do not delay for imaging.
- Consider broad differentials; elderly and immunosuppressed may have atypical presentations.
💊 Management
- 🔄 Resuscitation: ABCs, O₂, IV fluids, Fast patient NBM, catheter for urine output.
- 💉 Antibiotics: Broad-spectrum IV (e.g., Tazocin ± metronidazole).
- 💊 Analgesia: IV morphine (2.5–5 mg), antiemetics.
- 🧑⚕️ Urgent surgical referral: Early laparotomy/laparoscopy.
- 🧑⚕️Diagnostic triggers
- Abdominal pain + low BP → think sepsis
- Abdominal pain + low BP + >50 yrs → leaking AAA
- Abdominal pain + fertile female → ectopic pregnancy
- Abdominal pain + AF/MI → ischaemic bowel
- Abdominal pain + gallstones/alcohol → pancreatitis
🔪 Surgical Management
- Indicated for perforated viscus, bowel ischaemia, or generalised peritonitis.
- Procedures:
- Exploratory laparotomy/laparoscopy
- Resection of necrotic bowel, repair perforations
- Peritoneal lavage, drain abscesses
- Continue IV antibiotics post-op.
1. Initial Assessment & Red Flags
- ABCDE + vital signs + NEWS score
- Two large-bore IV access, bloods (FBC, U&E, CRP, lactate, amylase/lipase, LFTs, group & save ± crossmatch), urinalysis, pregnancy test (all women of childbearing age)
- Red flags requiring urgent senior/surgical input:
- Hypotension / tachycardia / shock
- Board-like rigid abdomen / generalised peritonism
- Pain out of proportion to examination findings
- Rising lactate (>2–4 mmol/L) or metabolic acidosis
- Free subdiaphragmatic air on erect CXR
- Elderly, diabetics, steroid/immunosuppressed patients (atypical / muted signs)
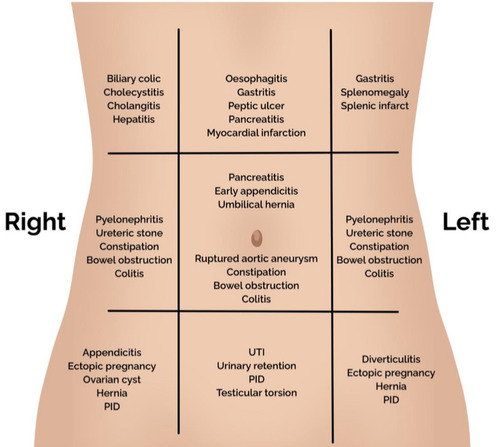
2. Differential Diagnosis by Anatomical Location
| Region | Common & Important Causes | Classic Clinical Features | First-line Investigations | Initial Management |
|---|---|---|---|---|
| Right Upper Quadrant (RUQ) | Acute cholecystitis
Cholangitis Biliary colic Perforated duodenal ulcer (referred) Hepatitis / liver abscess |
RUQ pain ± right shoulder tip
Murphy’s sign positive Charcot’s triad (fever + jaundice + RUQ pain) → cholangitis |
Abdominal ultrasound (first-line)
LFTs, FBC, CRP Blood cultures if febrile |
IV fluids, analgesia, IV antibiotics (if infection)
Early cholecystectomy (laparoscopic) for cholecystitis ERCP + antibiotics for cholangitis |
| Epigastric / Central | Perforated peptic ulcer
Acute pancreatitis Acute mesenteric ischaemia Aortic dissection / ruptured AAA Early appendicitis |
Sudden severe “knife-like” epigastric pain → perforation
Epigastric pain radiating to back → pancreatitis Severe pain out of proportion → ischaemia Tearing back/abdominal pain + shock → AAA |
Erect CXR (free air)
Amylase/lipase Lactate, CTA abdomen if ischaemia/AAA suspected Bedside US for AAA |
Resuscitation, NBM, IV PPI, broad-spectrum antibiotics, NG tube
Urgent laparotomy (perforation) Emergency vascular surgery (ruptured AAA) Heparin + revascularisation / resection (mesenteric ischaemia) |
| Right Lower Quadrant (RLQ) | Acute appendicitis
Mesenteric adenitis Ovarian torsion / ruptured cyst / ectopic Terminal ileitis (Crohn’s) |
Periumbilical → RLQ migration
Anorexia, nausea, low-grade fever Rebound / Rovsing’s sign |
FBC, CRP
Urine pregnancy test Ultrasound (young women / children) CT abdomen if diagnostic uncertainty |
IV fluids, analgesia, IV antibiotics
Laparoscopic appendicectomy |
| Left Lower Quadrant (LLQ) | Acute diverticulitis
Sigmoid volvulus Colonic perforation Ovarian / gynaecological pathology |
LLQ pain ± fever, change in bowel habit
Distension + tympany → volvulus |
CT abdomen/pelvis with IV contrast (gold standard)
AXR (coffee-bean sign in volvulus) |
IV fluids, IV antibiotics (e.g. co-amoxiclav or piperacillin-tazobactam)
Flexible sigmoidoscopy + decompression (volvulus without ischaemia) Surgery if perforation / peritonitis |
| Diffuse / Generalised | Generalised peritonitis (perforated viscus)
Bowel obstruction Mesenteric ischaemia Ruptured ectopic pregnancy Ruptured AAA |
Rigid “board-like” abdomen
Absent bowel sounds Shoulder tip pain (diaphragmatic irritation) |
Erect CXR (free air)
CT abdomen (most informative) β-hCG, FAST scan (ectopic) Bedside US or CTA (AAA / ischaemia) |
ABC resuscitation, broad-spectrum IV antibiotics, NBM, NG tube
Urgent laparotomy / laparoscopy |
3. Key Investigations – Tiered Approach
- Bedside / immediate: Pregnancy test, urinalysis, erect CXR (free air), ECG (exclude cardiac), FAST / POCUS (free fluid, AAA)
- Blood tests: FBC, U&E, CRP, lactate, amylase/lipase, LFTs, group & save / crossmatch, blood gas
- Imaging:
- Ultrasound: First-line for biliary, gynaecological, appendix (slim patients), AAA screening
- CT abdomen/pelvis with IV contrast: Gold standard for most acute surgical pathologies (perforation, ischaemia, diverticulitis, appendicitis in adults)
- CTA: Mesenteric ischaemia, aortic pathology
4. Antibiotic Choices (Empiric – Community-acquired)
- Mild–moderate: Co-amoxiclav IV or cefuroxime + metronidazole
- Severe / generalised peritonitis / healthcare-associated: Piperacillin-tazobactam (Tazocin) ± gentamicin (local policy)
- Cholangitis / biliary: Piperacillin-tazobactam or ceftriaxone + metronidazole
- Post-source control: Usually 4–5 days total; de-escalate / stop when clinically improved
5. Surgical vs Conservative Management Triggers
| Condition | Usually Surgical | Usually Conservative / Interventional |
|---|---|---|
| Appendicitis | Yes (laparoscopic appendicectomy) | Rarely antibiotics alone (selected uncomplicated cases) |
| Cholecystitis | Early laparoscopic cholecystectomy (within 7 days) | Antibiotics + percutaneous drainage (if unfit) |
| Perforated peptic ulcer | Yes (laparoscopic / open repair) | Very rare |
| Diverticulitis (uncomplicated) | No | IV antibiotics, fluids |
| Diverticulitis with abscess / perforation | Yes (often laparoscopic lavage or Hartmann’s) | Percutaneous drainage + antibiotics (selected cases) |
| Mesenteric ischaemia | Yes (revascularisation ± resection) | No |
| Ruptured AAA | Yes (open or EVAR) | No |
| Ruptured ectopic | Yes (salpingectomy / salpingostomy) | Methotrexate (stable, unruptured, selected cases) |
6. Final Key Take-home Messages
- Unstable or peritonism → theatre, not CT scanner
- Pregnancy test mandatory in women of reproductive age
- CT is the most useful single investigation in diagnostically uncertain cases in adults
- Pain out of proportion + atrial fibrillation / vascular risk → think acute mesenteric ischaemia
- Elderly / frail → assume surgical pathology until proven otherwise
- Early antibiotics + source control save lives in perforation / peritonitis
Always follow local protocols, consult senior clinicians, and refer to current trust / national guidelines (e.g., WSES 2024, NICE NG156, UpToDate 2026).
Case 1 – Perforated duodenal ulcer
A 48-year-old man with NSAID use develops sudden, severe epigastric pain radiating to the shoulder, rigid abdomen, and absent bowel sounds; vitals show tachycardia, low-grade fever, and mild hypotension. Erect CXR shows free subdiaphragmatic air. Manage with ABCDE, IV fluids, broad-spectrum antibiotics, PPI, NG tube, and urgent CT abdomen; refer for emergency surgery (laparoscopic Graham patch vs definitive ulcer surgery) and test/treat H. pylori after recovery.
Case 2 – Ruptured abdominal aortic aneurysm (AAA)
A 72-year-old man with smoking and hypertension presents with sudden tearing back/abdominal pain, hypotension, and a pulsatile abdominal mass. Avoid excessive fluids (permissive hypotension), give O₂, activate massive haemorrhage protocol, crossmatch, and call vascular surgery for immediate EVAR/open repair. POCUS/bedside ultrasound confirms large infrarenal AAA; do not delay for CT if unstable.
Case 3 – Ruptured ectopic pregnancy
A 30-year-old with 7 weeks’ amenorrhoea and vaginal spotting presents with worsening lower abdominal pain, dizziness, and shoulder tip pain; she is tachycardic and hypotensive with abdominal guarding. β-hCG positive; FAST scan shows free fluid. Resuscitate (O₂, IV access, bloods/crossmatch), consult gynae for urgent salpingectomy (or salpingostomy if appropriate), give anti-D if rhesus negative, and manage pain; differentials include ovarian torsion and ruptured corpus luteum.
Case 4 – Acute appendicitis
A 24-year-old develops periumbilical pain migrating to the RIF with anorexia, mild fever, and rebound tenderness; WBC/CRP raised. Ultrasound (slim female) or CT abdomen confirms inflamed, non-compressible appendix. Give IV fluids, analgesia, and broad-spectrum antibiotics; proceed to laparoscopic appendicectomy. Consider differentials (gynae, mesenteric adenitis); beware atypical retrocaecal pain.
Case 5 – Acute mesenteric ischaemia
A 78-year-old with AF has sudden, severe, diffuse abdominal pain out of proportion to scant early signs; lactate rising, metabolic acidosis. Urgent CTA shows SMA embolus. Resuscitate, start IV heparin and broad-spectrum antibiotics, involve vascular/HPB surgery for embolectomy/revascularisation ± bowel resection if non-viable; mortality is high-act fast.
Case 6 – Sigmoid volvulus
An 82-year-old in a care home presents with abdominal distension, pain, constipation, and tympany; X-ray shows the classic coffee-bean sign pointing to the RUQ. If no peritonitis/ischemia, perform flexible sigmoidoscopy with decompression and rectal tube; arrange definitive surgery (e.g., sigmoid colectomy) due to recurrence risk. If peritonitis or perforation, urgent laparotomy.
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
