| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Active Proctitis ✅
Related Subjects: |Rectal Prolapse |Anal Cancer |Anal Fissure |Perianal symptoms |Perianal abscesses and fistulae |Pilonidal Abscess (sinus) |Haemorrhoids (Piles) |Faecal Incontinence |Rectal Pain (Proctalgia) |Rectal Foreign Body |Acute Proctitis
🧠 Acute Proctitis refers to inflammation of the rectal mucosa, typically presenting with rectal pain, tenesmus, urgency, and bleeding. It results from mucosal barrier disruption with activation of innate and adaptive immune responses, leading to oedema, ulceration, and increased vascular permeability. ⚠️ In UK practice, infection must always be excluded first, particularly sexually transmitted causes, before diagnosing inflammatory disease. Management should be aetiology-directed, not purely symptomatic.
📌 Causes of Acute Proctitis
-
🦠 Infective (commonest in young adults)
- Sexually transmitted: gonorrhoea, chlamydia (incl. LGV), HSV, syphilis
- Enteric: Campylobacter, Shigella, Salmonella
- Clostridioides difficile (post-antibiotics)
-
🔥 Inflammatory
- Ulcerative colitis (classically starts in rectum)
- Crohn’s disease (less commonly isolated)
-
☢️ Radiation-induced
- Post pelvic radiotherapy (prostate, cervical, rectal cancer)
-
💊 Drug / Chemical
- NSAIDs, rectal preparations, enemas, irritants
-
⚠️ Other
- Ischaemia (elderly/vascular disease)
- Trauma, foreign bodies
- Solitary rectal ulcer syndrome
🧠 Pathophysiology
Acute proctitis involves epithelial injury → immune activation → mucosal inflammation. In infection, pathogen invasion drives neutrophilic infiltration and ulceration. In inflammatory bowel disease, dysregulated T-cell and cytokine responses (e.g. TNF-α) perpetuate damage. Radiation causes endothelial injury, fibrosis, and ischaemia, impairing healing.
🔍 Clinical Features
- Rectal pain, burning, discomfort
- Tenesmus (incomplete evacuation sensation)
- Rectal bleeding or mucus discharge
- Urgency ± diarrhoea
- Systemic symptoms (fever, malaise) if infective/severe
🧪 Investigation
- 🧫 Stool culture ± C. difficile toxin if diarrhoea
- 🧬 Rectal swabs for STI testing (essential in at-risk patients)
- 🩸 FBC, CRP, ESR
- 🧪 Consider HIV testing where appropriate
- 📸 Flexible sigmoidoscopy + biopsy if persistent, severe, or unclear diagnosis
💡 Clinical rule: Always exclude infection (especially STIs) before diagnosing IBD
💊 Management and Treatment
-
🦠 Infective
- Targeted antimicrobial therapy based on results
- Empirical STI treatment if high suspicion
- 👉 Refer to GUM clinic for testing, treatment, and contact tracing
-
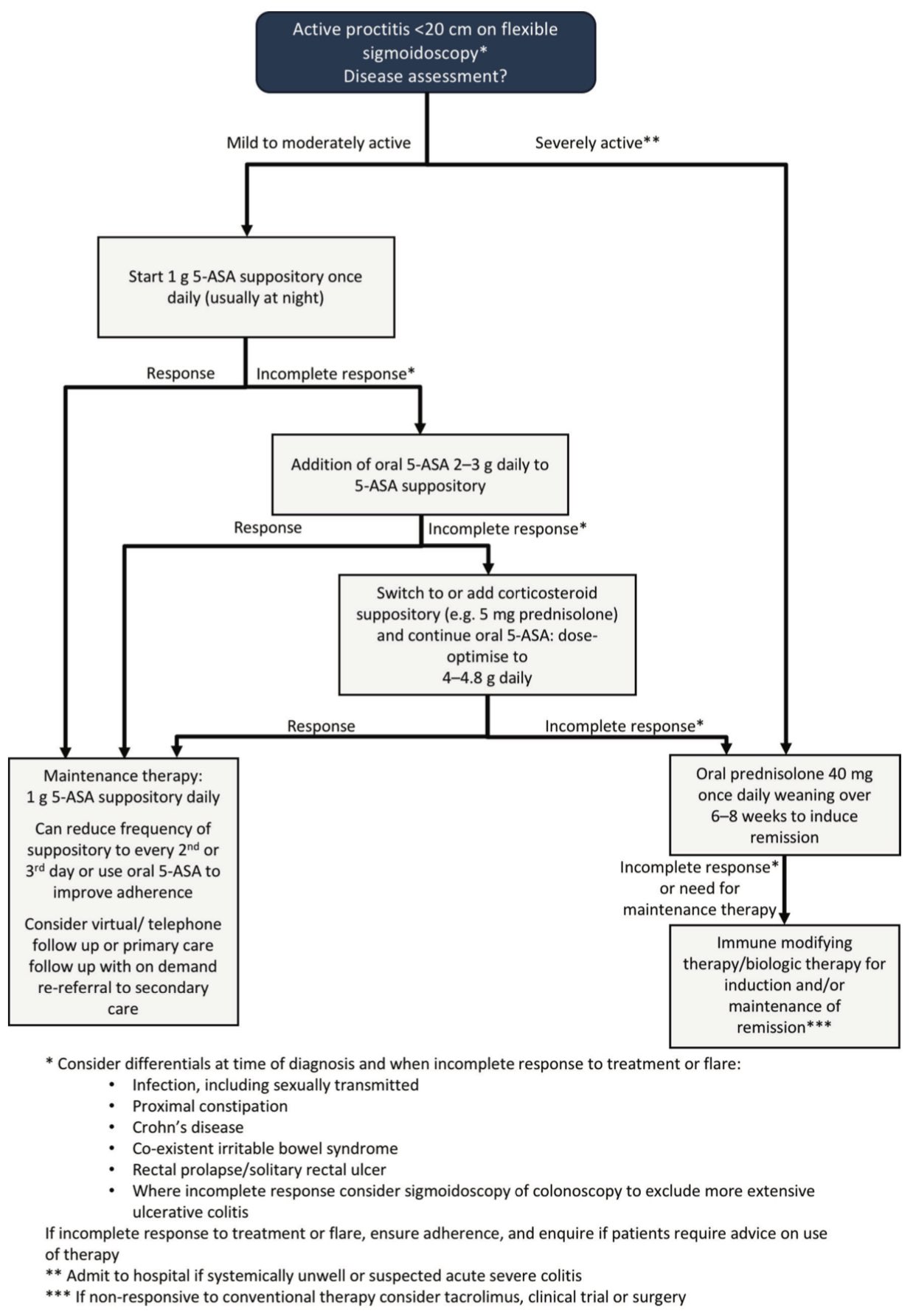
🔥 Inflammatory (IBD)
- Topical mesalazine suppositories first-line (high efficacy)
- Topical steroids if inadequate response
- Escalate to oral/systemic therapy if extensive or refractory
-
☢️ Radiation
- Sucralfate enemas, topical steroids
- Endoscopic therapy for persistent bleeding
-
🧴 Supportive
- Analgesia, stool softeners, hydration
- Avoid rectal irritants
🚨 Red Flags (Urgent Referral)
- Severe bleeding or haemodynamic instability
- Systemic sepsis
- ⚠️ Suspicion of colorectal malignancy (weight loss, anaemia, change in bowel habit)
- Failure to respond to initial therapy
🩸 Differential Diagnosis of Rectal Bleeding
| Cause | Key Features | Typical Clues |
|---|---|---|
| Haemorrhoids 🟣 | Painless bright red bleeding | Blood on paper, pruritus, no systemic symptoms |
| Anal fissure 🔪 | Severe pain on defecation | Fresh blood, tearing pain, constipation history |
| Proctitis 🦠 | Bleeding + tenesmus + urgency | Mucus, rectal pain, STI risk or IBD |
| Colorectal cancer 🎗️ | Change in bowel habit + bleeding | Weight loss, iron deficiency anaemia ⚠️ |
| Ulcerative colitis 🔥 | Bloody diarrhoea | Chronic symptoms, urgency, systemic features |
| Crohn’s disease 🌿 | Less overt bleeding | Abdominal pain, weight loss, perianal disease |
| Diverticular disease 💥 | Painless large-volume bleeding | Elderly, sudden onset |
| Angiodysplasia 🧬 | Intermittent bleeding | Elderly, associated with aortic stenosis |
| Infective colitis 🦠 | Bloody diarrhoea + fever | Recent travel, food exposure |
| Ischaemic colitis ⚠️ | Pain + bleeding | Older patient, vascular risk factors |
📚 Key Learning Points
Acute proctitis is a symptom-based diagnosis requiring systematic evaluation. In UK practice, STI causes are common and must be excluded early. Topical therapy is highly effective in IBD due to direct mucosal delivery. Thinking mechanistically - epithelial injury, immune activation, and vascular compromise - helps guide targeted treatment and avoid misdiagnosis.
📚 References (UK Guidance)
- NICE CKS – Diarrhoea: assessment of infective causes and stool testing
- NICE NG12: Suspected cancer – recognition and referral (colorectal cancer red flags)
- BASHH Guidelines: Management of sexually transmitted infections (gonorrhoea, chlamydia, HSV, syphilis)
- NICE NG197: Ulcerative colitis – management (including topical mesalazine)
- NICE QS161: Inflammatory bowel disease quality standard
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
