| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Miliary (Disseminated) Tuberculosis
Related Subjects: |Assessing Breathlessness |Fever - Pyrexia of unknown origin |Tuberculosis |TB Meningitis |Miliary Tuberculosis |Lady Windermere syndrome
Key point: Miliary TB is haematogenous (blood-borne) dissemination of Mycobacterium tuberculosis, producing countless tiny granulomas across multiple organs (classically “millet seed” nodules in the lungs). It can be rapidly fatal if missed, and may present without a dramatic cough - think unexplained systemic illness, abnormal LFTs, cytopenias, or sepsis-like physiology.
📌 Why it matters (UK context)
- TB remains an important UK diagnosis; UKHSA provisional data for England reported 5,424 TB notifications in 2025 (broadly stable vs 2024).
- Miliary TB is less common than isolated pulmonary TB but is high-risk: higher rates of delayed diagnosis, multi-organ failure, and CNS involvement.
- In the UK, TB (including disseminated forms) requires specialist TB team involvement, notification, and contact tracing.
🧬 Pathophysiology (the “why”)
- Primary infection or reactivation can seed bacilli into the bloodstream → widespread micro-embolic spread to lungs, liver, spleen, bone marrow, adrenals, kidneys, meninges, and eye.
- Host response forms granulomas (macrophages, T-cells, caseation). The burden becomes “miliary” when dissemination is extensive.
- Risk rises with impaired cell-mediated immunity: HIV, steroids/biologics (anti-TNF), transplant, CKD, diabetes, malnutrition, pregnancy/post-partum, extremes of age.
⚠️ When to suspect miliary TB (clinical clues)
- Constitutional: fever, night sweats 🌙, weight loss, anorexia, profound fatigue.
- Respiratory: dry cough, dyspnoea, tachypnoea; may be mild or absent early.
- Sepsis-like picture: hypotension, high lactate, multi-organ dysfunction.
- Organ hints:
- Liver: cholestatic/raised ALP, hepatosplenomegaly, jaundice.
- Bone marrow: pancytopenia, unexplained anaemia.
- CNS: headache, confusion, meningism, cranial nerve palsies (think TB meningitis / tuberculomas).
- Adrenal: hyponatraemia, hyperkalaemia, hypotension → possible adrenal TB/Addisonian crisis.
- Eye: choroidal tubercles (important clue; urgent ophthalmology if visual symptoms).
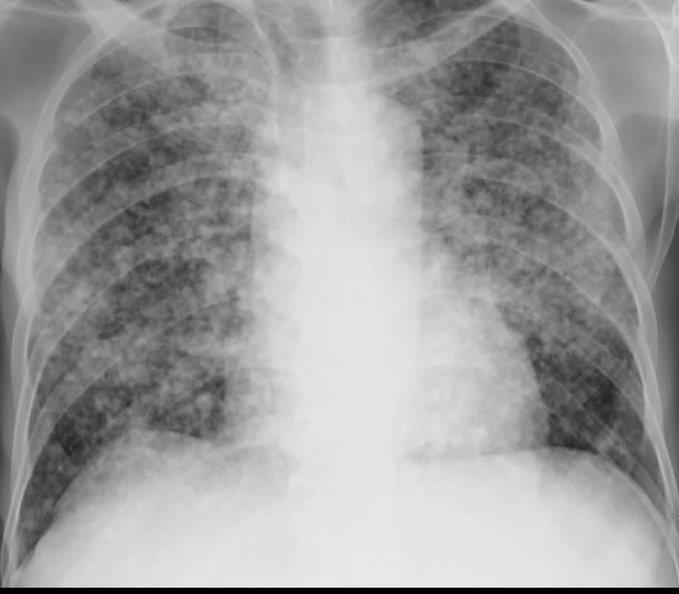
🩻 Imaging
- CXR: classic diffuse, fine nodular (“miliary”) mottling - but can be normal early.
- HRCT chest: more sensitive; shows innumerable 1–3 mm nodules with random distribution.
- CT/MRI brain if neuro symptoms/signs: meningitis features, hydrocephalus, tuberculomas.
- Abdominal imaging (USS/CT) if hepatosplenomegaly, abnormal LFTs, lymphadenopathy, ascites.
🧪 Investigations (practical, high-yield)
1) Baseline bloods
- FBC (anaemia, leukopenia, thrombocytopenia), CRP/ESR.
- U&E (hyponatraemia; renal impairment impacts dosing), LFTs (common derangement), glucose.
- HIV test (offer routinely in suspected/confirmed TB), hepatitis B/C baseline before treatment where relevant. :contentReference[oaicite:2]{index=2}
2) Microbiology (send early, send widely)
- Respiratory samples (even if cough minimal): sputum (induced if needed), BAL if intubated/bronchoscopy.
- NAAT/PCR (e.g., Xpert MTB/RIF-style assays) where available for rapid detection ± rifampicin resistance signal.
- Culture from multiple sites (slow but essential) + full drug susceptibility testing.
- Blood cultures for mycobacteria (especially in HIV/advanced disease) and urine AFB/culture if GU involvement suspected.
- Bone marrow aspirate/trephine if pancytopenia/PUO - can yield TB on culture/histology.
3) Histology
- Biopsy accessible sites: lymph node, liver, pleura, bone marrow. Look for granulomas; send tissue for AFB stain + TB PCR + culture.
4) Lumbar puncture (LP) - do not miss CNS TB
- LP if any CNS symptoms/signs or unexplained delirium.
- Typical TB meningitis CSF: lymphocytic predominance, high protein, low glucose (but can be mixed early).
🔎 Differential diagnosis (things that mimic “miliary”)
| Condition | Clues | How to distinguish |
|---|---|---|
| 🦠 Disseminated fungal infection (e.g., histoplasmosis) | Immunosuppression, travel/exposure | Fungal cultures/antigen tests, biopsy |
| 🎗️ Miliary metastases | Known malignancy, weight loss, bone pain | CT pattern + tumour markers/biopsy |
| 🫁 Sarcoidosis / hypersensitivity pneumonitis | Non-infective systemic features | ACE (non-specific), BAL profile, biopsy (non-caseating) |
| 🦠 Pneumocystis jirovecii (HIV) | Severe hypoxia, diffuse ground-glass | CT pattern + PCR/BAL; LDH raised |
| 🧫 Sepsis with DIC / HLH | Shock, cytopenias, ferritin very high | Bone marrow + HLH workup; TB can trigger HLH |
🚑 Immediate management (what you do first)
- Escalate early: involve the TB specialist team urgently; miliary TB is “severe TB” until proven otherwise. :contentReference[oaicite:3]{index=3}
- Assess severity: oxygenation, ABG/VBG, lactate, organ dysfunction; consider ITU if respiratory failure/ARDS.
- Infection control: treat as potentially infectious pulmonary TB until assessed - use airborne precautions if pulmonary involvement suspected (local IPC policy + TB team advice).
- Start treatment promptly if high clinical suspicion, especially if critically unwell, after obtaining urgent samples (do not delay lifesaving therapy waiting for culture).
💊 Treatment (drug-susceptible TB, typical UK approach)
In the UK, standard initial therapy for active TB is 4-drug therapy while awaiting drug susceptibilities:
| Phase | Regimen | Typical duration | Notes |
|---|---|---|---|
| Intensive 🔥 | Rifampicin + Isoniazid + Pyrazinamide + Ethambutol (RIPE) | 2 months | Use ethambutol until sensitivities known |
| Continuation ✅ | Rifampicin + Isoniazid | 4 months | Total 6 months for many non-CNS cases |
Important: Duration often needs extension in disseminated disease depending on site (e.g., CNS TB, bone/joint TB). Always follow the TB specialist plan and local protocol. NICE NG33 is the core UK reference for TB services and management principles.
🧠 If CNS involvement (TB meningitis / tuberculoma)
- Requires urgent specialist management, neuroimaging, LP (where safe), and typically longer treatment than 6 months.
- Corticosteroids are standard adjunctive therapy for TB meningitis and reduce inflammatory damage (oedema, vasculitis, infarction risk).
❤️ If TB pericarditis
- Also typically treated with adjunctive steroids (specialist-led) due to risk of constriction and intense inflammation.
🌡️ Steroids in “severe” miliary TB
- Not routine for all miliary TB, but may be considered in selected severe inflammatory complications (e.g., ARDS, adrenal involvement) - this should be TB specialist/ICU-led because immunosuppression can worsen uncontrolled infection if misapplied.
🧯 Monitoring & safety (don’t get caught out)
- Baseline: LFTs, U&E, FBC; consider visual acuity/colour vision if ethambutol is used (especially prolonged therapy).
- Drug interactions (very common): rifampicin is a strong enzyme inducer → affects warfarin, DOACs, many antiepileptics, methadone, contraceptives, steroids, and antiretrovirals. Liaise with pharmacy/HIV team early.
- Hepatotoxicity: isoniazid/rifampicin/pyrazinamide can all contribute - interpret LFT rises with symptoms, bilirubin, and clinical trajectory.
- Paradoxical reactions / IRIS: clinical worsening after starting therapy (esp. HIV) due to immune rebound; distinguish from resistance, non-adherence, or alternative diagnosis.
- Adherence support: TB teams may use DOT/VOT (direct/video observed therapy) for complex cases or adherence risk.
🧑🧑🧒 Public health duties (UK)
- TB is notifiable and managed through specialist TB services with contact tracing.
- Assess close household contacts for symptoms and TB testing; consider latent TB screening/treatment according to risk.
- Consider social factors: housing insecurity, substance use, barriers to follow-up - addressing these reduces transmission and relapse risk.
🚨 Complications (what kills patients)
- Acute respiratory failure / ARDS
- TB meningitis → infarction, hydrocephalus, long-term disability
- Bone marrow failure and severe anaemia/cytopenias
- Adrenal insufficiency
- HLH (rare but critical; TB can be a trigger)
🌍 Advice for patients and clinicians in low- and middle-income settings: In resource-limited settings, early recognition of miliary TB is critical because delayed diagnosis is a major driver of mortality. Any patient with prolonged fever, weight loss, night sweats, unexplained anaemia, or multi-organ symptoms should prompt strong clinical suspicion, even if chest X-ray findings are subtle or absent. Where advanced imaging and cultures are unavailable, treatment should be started on strong clinical grounds after basic microbiological sampling, as untreated dissemination rapidly leads to respiratory failure, CNS disease, and adrenal insufficiency. Ensuring reliable access to full-course combination therapy, supporting adherence through community health workers, and addressing malnutrition and HIV co-infection are as important as prescribing drugs. From a systems perspective, strengthening contact tracing, reducing stigma, and integrating TB care into primary health services remain the most effective long-term strategies for reducing transmission and late presentations.
✅ “Makindo exam pearls”
- Think miliary TB in PUO + weight loss + abnormal LFTs/cytopenias, especially with immunosuppression or epidemiological risk.
- A normal early CXR does not exclude it - HRCT is more sensitive.
- Always ask: “Could there be CNS TB?” - because it changes urgency, imaging, LP decisions, steroid use, and duration.
🖼️ Suggested Makindo images/figures to add
- Figure: “Miliary pattern on CXR vs HRCT (random micronodules)”
- Diagram: “Haematogenous dissemination pathway (lungs → bloodstream → organs)”
- Flowchart: “Suspected miliary TB: samples first → start RIPE → assess CNS → TB team + IPC”
📚 References (UK & international)
- NICE Guideline NG33: Tuberculosis (last reviewed Feb 2024; NICE PDF copyright 2025).
- UKHSA (England): National quarterly report of TB - Quarter 4, 2025 (provisional).
- WHO consolidated guidelines on TB, Module 4: Treatment and care (updated evidence-based recommendations).
- Ray S et al. Review: Diagnosis and management of miliary tuberculosis. :
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
