| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Idiopathic Fascicular Left Ventricular Tachycardia
Related Subjects: |Classical Ventricular Tachycardia |Idiopathic Ventricular Tachycardia |Right Ventricular Outflow Tract Tachycardia |Idiopathic Fascicular Left Ventricular Tachycardia |Left Ventricular Outflow Tract Tachycardia |Ventricular Fibrillation |Resuscitation - Adult Tachycardia Algorithm |Resuscitation - Advanced Life Support |Automatic Implantable Cardioverter Defibrillator (AICD)
⚡ Idiopathic ventricular tachycardia (IVT) in patients with an anatomically normal heart is a distinct entity whose management and prognosis differs from ventricular tachycardia associated with structural heart disease. This is a specialist diagnosis and should not be confused with VT in the setting of cardiomyopathy. ✅
📖 About
- A form of Idiopathic Ventricular Tachycardia (IVT).
- 💓 The most common idiopathic VT of the left ventricle, often arising from the Purkinje system.
🧬 Aetiology
- Absence of structural heart disease 🫀.
- Due to a re-entrant arrhythmia mechanism involving the fascicles of the left bundle branch.
- Mainly affects males (60–80%), young to middle-aged (15–40 years). 👨
🔎 Forms (Subtypes)
- Posterior fascicular VT (most common, ⬇️ axis).
- Anterior fascicular VT (less common, ⬆️ axis).
- Upper septal fascicular VT (rare, narrowest QRS).
✅ Diagnostic Criteria
- No structural heart disease (confirmed by Echo/CMR).
- No metabolic or electrolyte abnormalities (exclude hypoK/Mg, etc.).
- No inherited arrhythmia syndromes (e.g., Long QT, Brugada, CPVT).
📊 Fascicular VT ECG Example
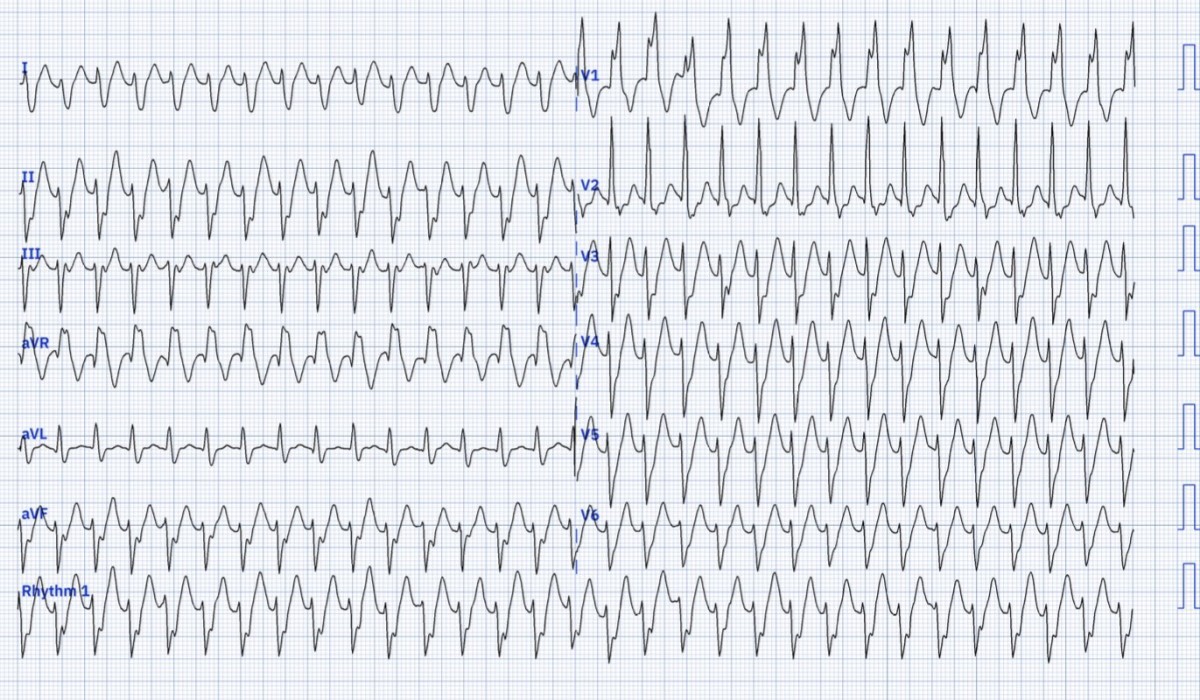
🩺 Classical VT is still the most common cause of wide-complex regular tachycardia. ❗ There is no perfectly reliable ECG method to distinguish classical VT from idiopathic VT or SVT with aberrancy. 👉 Always treat as VT until proven otherwise – follow the Adult Tachycardia (ALS) algorithm.
👩⚕️ Clinical Features
- Typically young male adults (15–40 years).
- Symptoms: palpitations 💓, dizziness, presyncope/syncope 😵, often triggered by exertion, febrile illness, or stress.
- Usually well tolerated, unlike scar-related VT, but still causes functional limitation.
🧪 Investigations
- 🧾 Bloods: Normal (exclude electrolytes, thyroid).
- 🫀 Echocardiogram: Normal LV size and function.
- 📷 CXR: Normal.
- 🩺 12-lead ECG (baseline): QT normal, no structural abnormality.
- 📉 Acute ECG during VT: RBBB morphology, axis depending on subtype; QRS narrower (100–140 ms) compared to other VT.
- 💡 Cardiac MRI may be used to exclude subtle myocarditis, sarcoid or ARVC.
💊 Management
- 🔑 First principle: If in doubt, treat as classical VT and involve cardiology early.
- 🛑 ABC approach. If unstable ➝ DC cardioversion (per ALS). ⚡
- 👨⚕️ In stable, proven fascicular VT with normal LV function ➝ IV Verapamil 10 mg over 3–5 min under senior cardiology supervision (be ready to DC convert). ❗ NEVER use verapamil if diagnosis uncertain as it may be fatal in scar-related VT.
- For recurrent but moderate symptoms ➝ Oral Verapamil (120–480 mg/day).
- Radiofrequency catheter ablation 🔥 offers curative therapy in >90% of patients with symptomatic or drug-refractory VT.
- 💡 Unlike scar VT, idiopathic fascicular VT has an excellent long-term prognosis with low risk of sudden death once properly diagnosed and managed.
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
