| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Tuberculous Meningitis
Related Subjects: |Lumbar Puncture |Tuberculosis |TB Meningitis |Miliary Tuberculosis |Lady Windermere syndrome
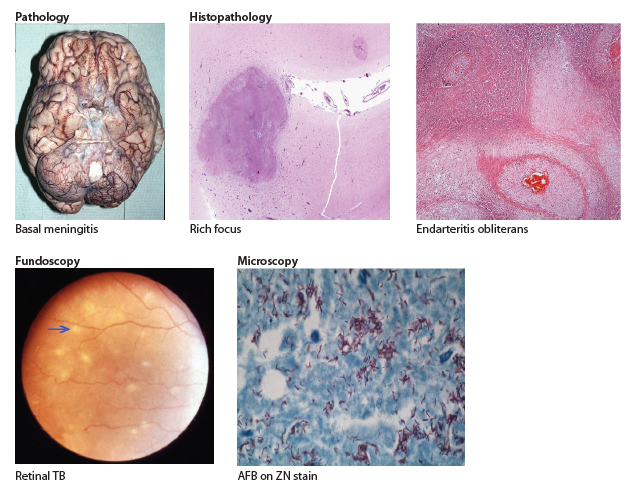
🧠 Tuberculosis can spread to the central nervous system, forming a Rich focus that may rupture into brain tissue. This can cause meningitis, tuberculomas, vasculitis, and hydrocephalus. Early recognition is critical for survival and prevention of long-term disability.
📖 About
- Presentation is often insidious, with subtle early features.
- Diagnosis is challenging but essential to prevent severe complications such as stroke or coma.
🧬 Tuberculous Involvement of the CNS
- TB Meningitis: Basal meningeal inflammation with high risk of hydrocephalus and cranial nerve palsies.
- Tuberculomas: Space-occupying granulomas causing focal neurology or seizures.
- Spinal Arachnoiditis: Pain, progressive weakness, and sometimes paralysis.
- TB Arteritis: Vasculitis leading to ischaemic strokes.
- Hydrocephalus: From impaired CSF resorption or blocked aqueduct.
- Cranial Nerve Involvement: Especially VI (abducens palsy) due to basal exudates.
⚠️ Aetiology & Risk Factors
- Recent TB exposure.
- HIV/AIDS or other immunosuppression.
- Alcoholism and malnutrition.
📊 Stages
- Stage I: Alert, rational, no focal neurology or hydrocephalus.
- Stage II: Confusion, with focal neurological signs.
- Stage III: Coma, hemiparesis/paraplegia, seizures, delirium.
🩺 Clinical Features
- Symptoms: Subacute fever, headache, malaise for 2–3 weeks.
- Signs: Meningism, vomiting, altered mental status, seizures.
- Cranial Nerve Palsies: Most often III & VI.
- Pathophysiology: Basal meningitis, optic chiasm involvement, vasculitis → thrombosis & infarcts.
- Hydrocephalus: From protein-rich CSF blocking resorption.
- Systemic: Lymphadenopathy, splenomegaly in some cases.
🔬 Investigations
- Bloods: FBC, U&E, LFTs, CRP/ESR (often raised).
- Mantoux Test: Positive in ~50%, not definitive.
- CSF: High protein (1–5 g/L), low glucose, lymphocytic pleocytosis. AFB smear often negative. Culture slow (up to 6 weeks). PCR can expedite diagnosis.
- Imaging:
- CT: May be normal early. Later: basal enhancement, hydrocephalus, or tuberculomas.
- MRI: Best for showing tuberculomas and basal exudates.
- HIV Test: Mandatory, given the strong association.
💊 Management
- Anti-TB Therapy:
- 2 months: Isoniazid, Rifampicin, Pyrazinamide, Ethambutol.
- Continuation: Isoniazid + Rifampicin for 7–10 months.
- Steroids: Dexamethasone or Prednisolone for raised ICP, hydrocephalus, or focal deficits. Taper over 4–8 weeks.
- Hydrocephalus: Ventriculoperitoneal shunt if severe.
- HIV Co-infection: Start HAART carefully (watch for IRIS).
- Supportive Care: Anticonvulsants if seizures, nutritional support, and monitoring for complications.
📌 Key Clinical Pearls
- Think of TB in subacute meningitis with cranial nerve palsies or basal exudates.
- Always test for HIV in suspected CNS TB.
- Start treatment early - waiting for culture confirmation can be fatal.
- Steroids improve survival and reduce neurological sequelae.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
