| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acne Vulgaris ✅
Related Subjects: | Nikolsky's sign | Koebner phenomenon | Erythema Multiforme | Pyoderma gangrenosum | Erythema Nodosum | Dermatitis Herpetiformis | Lichen Planus | Acanthosis Nigricans | Acne Rosacea | Acne Vulgaris | Alopecia | Vitiligo | Urticaria | Basal Cell Carcinoma | Malignant Melanoma | Squamous Cell Carcinoma | Mycosis Fungoides (Sezary Syndrome) | Xeroderma pigmentosum | Bullous Pemphigoid | Pemphigus Vulgaris | Seborrheic Dermatitis | Pityriasis/Tinea versicolor infections | Pityriasis rosea | Scabies | Dermatomyositis | Toxic Epidermal Necrolysis | Stevens-Johnson Syndrome | Atopic Eczema/Atopic Dermatitis | Psoriasis
🧑⚕️ Acne Vulgaris is a chronic inflammatory disorder of the pilosebaceous unit, affecting adolescents and adults. It presents with comedones, inflammatory papules/pustules, nodules, and sometimes cysts. 💡 Acne is multifactorial: genetics, hormones, immune response, microbiome, environment, and lifestyle all contribute. Early recognition and structured treatment prevents scarring and psychological morbidity.
🧬 Aetiology & Risk Factors
- 🧬 Genetic predisposition: First-degree relatives with acne → ↑ risk. Polymorphisms in androgen receptor, TNF-α, IL-1α, filaggrin.
- 💡 Androgen excess: Testosterone → DHT via 5α-reductase in sebaceous glands → sebaceous hyperplasia and ↑ sebum production 🧴.
- 🧪 Sebum composition: Rich in triglycerides, squalene, free fatty acids → follicular occlusion, lipid peroxidation, bacterial growth.
- 🧫 Follicular hyperkeratinisation: Abnormal keratinocyte differentiation → comedones. Retinoid pathways dysregulated.
- 🦠 Cutibacterium acnes colonisation: Triggers TLR2 → ↑ IL-1β, IL-8, TNF-α → neutrophil recruitment → pustules. Biofilm formation prolongs inflammation.
- 🔥 Inflammatory response: Early lesions show CD4⁺ T cells, macrophages, neutrophils → papules, pustules, nodules.
- 💊 Drugs: Corticosteroids, lithium, anticonvulsants, androgenic steroids.
- 🥗 Diet & lifestyle: High GI foods → ↑ insulin/IGF-1 → sebum synthesis; dairy may ↑ androgenic activity.
- ⚖️ Endocrine disorders: PCOS, Cushing’s, congenital adrenal hyperplasia → severe acne.
- 🌞 Environmental: UV light, occlusion, heat, humidity, pollution.
🔬 Pathophysiology (Stepwise)
Acne lesions arise from interaction of four main pathogenic processes:
- Sebaceous gland hyperactivity – DHT and IGF-1 ↑ sebum. Lipid peroxidation → comedone inflammation.
- Follicular hyperkeratinisation – Abnormal keratin shedding → microcomedone → clinical comedones.
- Microbial colonisation – C. acnes proliferates → activates innate immunity (TLR2, inflammasome) → inflammatory cytokines.
- Inflammatory cascade – Neutrophils, lymphocytes, macrophages → papules, pustules, nodules, scarring. Chronic lesions → fibrosis, hyperpigmentation, keloids.
🖼️ Illustrations
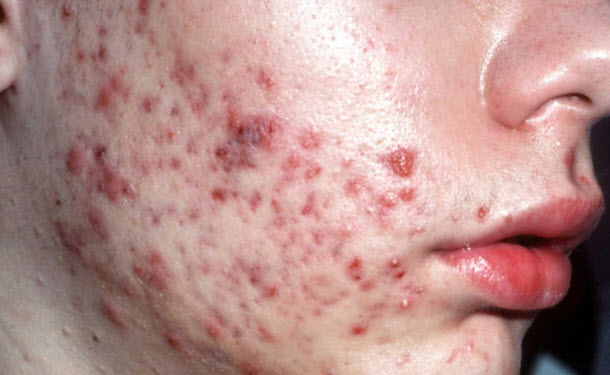
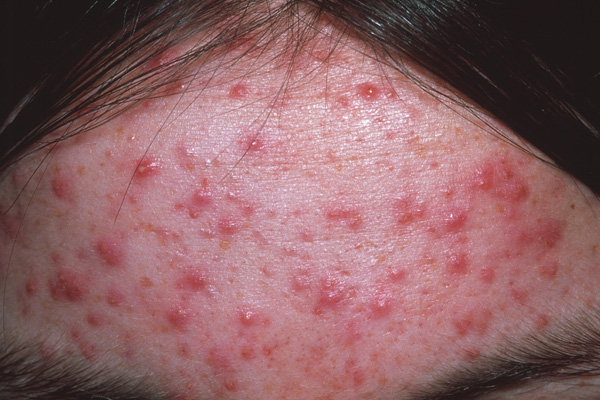
💡 Key Teaching Points
- Acne is a multifactorial inflammatory disease, not just “hormones” or “hygiene.”
- DHT drives sebaceous hyperplasia → androgen-blocking therapy may help.
- Innate immunity (TLR2, cytokines) → target for topical retinoids and anti-inflammatory agents.
- Systemic triggers (stress, diet, drugs, endocrine disorders) modulate severity and chronicity.
- Pathophysiology guides stepwise treatment: retinoids normalize keratinisation, benzoyl peroxide reduces bacteria, antibiotics/isotretinoin reduce inflammation & sebaceous activity.
💊 Management – NICE-Compliant & Stepwise
Guided by severity,
🔎 Principles
- Treat all 4 pathogenic processes: sebum, hyperkeratinisation, bacterial load, inflammation.
- Use combination therapy where possible to improve efficacy & reduce resistance.
- Review every 8–12 weeks; adjust therapy accordingly.
- Monitor for side effects (photosensitivity, irritation, antibiotic resistance, systemic toxicity).
📊 Stepwise Treatment
| Severity | Recommended Therapy | Monitoring / Notes |
|---|---|---|
| Mild (comedonal) |
|
|
| Moderate (papules/pustules) |
|
|
| Severe / Nodulocystic |
|
|
| Hormonal Acne (Women) |
|
|
📌 Practical UK Notes
- Benzoyl peroxide reduces resistance, use with antibiotics
- Topical retinoids: start 2–3 nights/week, gradually increase
- Oral antibiotics: stop at 3–6 months or if no response by 12 weeks
- Isotretinoin: pregnancy prevention, monthly labs, monitor side effects
- Gentle, non-comedogenic skincare; SPF ≥30 daily
- Adherence: 6–12 weeks to see improvement
⚠️ Urgent / Specialist Considerations
- Acne fulminans or sudden severe flare → urgent dermatology referral
- Resistant acne after multiple courses → dermatology opinion
- Endocrine disorders suspected (PCOS, virilisation) → endocrine/dermatology assessment
📈 Long-Term Maintenance
- Topical retinoid + benzoyl peroxide to prevent relapse
- Assess ongoing hormonal therapy needs
- Address psychosocial impact, counselling or support groups
📚 UK Guidelines

Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
