| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Sickle Cell Disease
Related Subjects:
|Sickle Cell Disease
|Acute Chest Syndrome (Sickle Cell)
|Exchange Transfusion
🩸 Sickle Cell Disease (SCD) → Inform haematology immediately if a known HbSS/SC patient is admitted.
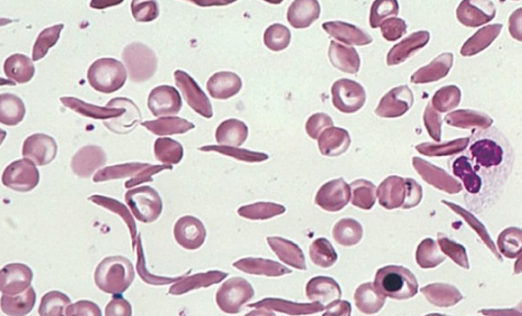
🔄 In SCD, red cells become “sickle-shaped” under hypoxic stress → vaso-occlusion, haemolysis, and multiorgan complications.
📚 Exam / OSCE Pearls
– 🚨 Sickle crises are medical emergencies → treat pain + fluids promptly.
– 🤒 Always rule out infection.
– 🌬️ Chest crisis: O₂ + antibiotics + consider exchange transfusion.
– 🍆 Ask about priapism, 🧠 neuro symptoms, 🪫 splenic sequestration in any acute admission.
Teaching Point 🩺: Sickle cell disease is an inherited haemoglobinopathy (HbSS) leading to haemolysis and vaso-occlusion. Key complications include: painful crises, acute chest syndrome, stroke, splenic sequestration, infections, chronic organ damage. Hydroxycarbamide, vaccination, prophylactic antibiotics, and transfusion programmes improve survival.
📖 About
🧬 Aetiology
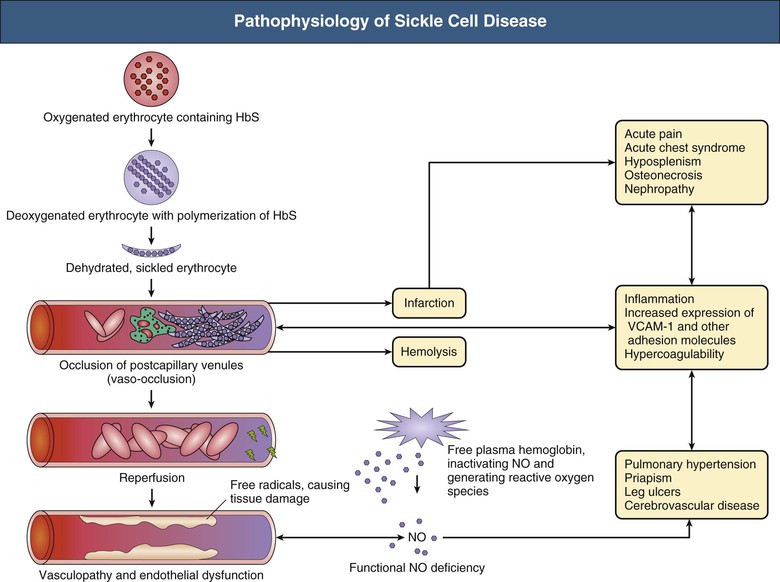
⚡ Precipitants of Sickling
🩺 Types of Haemoglobinopathy
👩⚕️ Clinical Presentation
🚑 Complications
🔎 Investigations
💊 Management of Acute Crisis
📅 Long-Term Management
📖 References
Cases - Sickle Cell Disease
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
