| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Spontaneous Pneumothorax
Related Subjects: Asthma
|Acute Severe Asthma
|Exacerbation of COPD
|Pulmonary Embolism
|Cardiogenic Pulmonary Oedema
|Pneumothorax
|Tension Pneumothorax
|Respiratory (Chest) infections Pneumonia
|Fat embolism
|Hyperventilation Syndrome
|ARDS
|Respiratory Failure
|Pleural effusion
|Pleural tap (thoracentesis)
⚠️ Treatment depends critically on whether it is a primary or secondary pneumothorax. Underlying lung disease = secondary, which is treated far more cautiously. 💨 Always suspect a pneumothorax in any mechanically ventilated patient with sudden deterioration (may present only as ↑ resistance to ventilation).
📖 About
- 🫁 Spontaneous presence of air in the pleural space.
- 👵 Patients >50 or with lung disease = secondary pneumothorax → require admission.
⚙️ Mechanism
- Hole in visceral pleura → air leaks into pleural space.
- Penetrating wounds (oesophagus, mediastinum, diaphragm).
- Gas-forming bacteria within empyema.
📂 Types
- 🟢 Primary: Age <50, no lung disease, minimal smoking history.
- 🔴 Secondary: Due to underlying lung disease.
- ⚔️ Traumatic: Injury-related (penetrating/blunt).
📊 Classification
- Primary Pneumothorax:
- 👨 Tall, thin young men (20–40 yrs), often right-sided.
- 🚬 Smoking ↑ risk (even subclinical lung disease).
- 🌬️ Subpleural blebs rupture due to apex stress.
- 🔁 Recurrence: ~40% within 2 years (especially smokers).
- Secondary Pneumothorax:
- Due to 👇
- ⚔️ Trauma (penetrating injuries).
- 💉 Iatrogenic (biopsy, pleural procedures).
- 💨 Ventilation (barotrauma with high PEEP).
- 🫁 Lung disease (COPD, asthma, CF, PCP pneumonia).
- 📉 Rare: Marfan’s, catamenial (endometriosis).
- Due to 👇
🩺 Clinical
- May be silent if small.
- Typical: sudden chest pain ⚡ + breathlessness 🫁.
- Severe: hypotension, tachycardia, cyanosis.
- Exam: hyper-resonance, ↓ breath sounds. ➡️ Tension PTX: tracheal deviation + distended neck veins.
🔍 Investigations
- 📸 CXR: Lung edge visible, no markings peripheral to it.
- 📏 Size: Small = <2 cm rim; Large = >2 cm.
- 🖥️ HRCT: For complex cases / to differentiate bullae.
💊 Management of Spontaneous Pneumothorax
- Initial assessment: ABCDE assessment, observations, oxygen saturation, analgesia and chest X-ray. Give oxygen if hypoxic; use controlled oxygen in patients at risk of CO₂ retention, such as severe COPD. If tension pneumothorax is suspected clinically, treat immediately — do not wait for imaging. Assess: symptoms, haemodynamic stability, oxygen requirement, underlying lung disease, pneumothorax size and recurrence risk.
- Size terminology: Older BTS guidance used a 2 cm rim on CXR at the level of the hilum to define a large pneumothorax. Current practice is more symptom-led: breathlessness, physiological compromise and underlying lung disease often matter more than size alone. A small pneumothorax is often described as <2 cm; a large pneumothorax as ≥2 cm, but management should not rely on size alone.
- Primary Spontaneous Pneumothorax
- No underlying lung disease: Minimally symptomatic and physiologically stable: consider conservative management, even if large, with safety-netting and early follow-up.
- Symptomatic or patient prefers active treatment: consider needle aspiration, ambulatory device or small-bore chest drain depending on local expertise and patient preference.
- Failed aspiration, persistent symptoms, ongoing air leak or clinical deterioration: insert a small-bore chest drain and admit.
- Secondary Spontaneous Pneumothorax — underlying lung disease, e.g. COPD, asthma, cystic fibrosis, ILD:
- Lower threshold for admission because respiratory reserve is reduced.
- Small and minimally symptomatic: admit for observation, oxygen if needed, analgesia and repeat imaging.
- Symptomatic, hypoxic, large or physiological compromise: insert a small-bore chest drain and admit.
- Needle aspiration may be considered in selected cases, but chest drain is often required.
- Aspiration: Needle aspiration is a controlled procedure for a spontaneous pneumothorax when the patient is usually stable but symptomatic or has a larger pneumothorax. The aim is to aspirate air with a syringe/3-way tap and potentially avoid a chest drain. Site is 2nd ICS MCL, or 4th/5th ICS AAL or MAL, aspirate up to 2.5 L → repeat CXR.
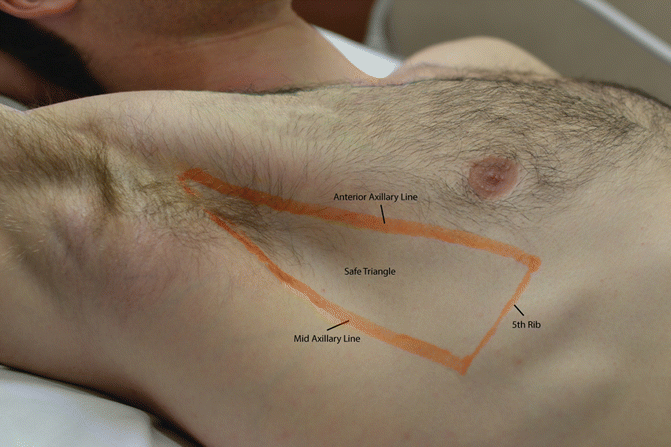
- Chest drain: Use a small-bore drain in most spontaneous pneumothoraces. Large-bore drains are usually reserved for trauma, haemothorax, very large air leak or specialist indications. Avoid routine suction initially; consider specialist advice if the lung fails to re-expand or there is persistent air leak. Indications: >2 cm and symptoms, failed aspiration, secondary PTX. Insert in safe triangle → monitor bubbling & swinging.
- When to involve thoracic surgery / consider VATS:
- Persistent air leak, often after 5–7 days depending on local policy and clinical context.
- Failure of lung re-expansion despite chest drainage.
- Recurrent ipsilateral pneumothorax.
- First contralateral pneumothorax.
- Bilateral spontaneous pneumothoraces.
- Spontaneous haemopneumothorax.
- High-risk occupation or activity, e.g. pilot, diver, remote worker.
- Patient preference after discussion of recurrence risk and treatment options.
- VATS procedure: VATS = video-assisted thoracoscopic surgery. Usually involves stapling/resection of visible blebs or bullae plus pleurodesis or pleural abrasion/pleurectomy to reduce recurrence. It is used mainly for recurrence prevention or persistent air leak, not as routine first-line treatment for every first pneumothorax.
- Discharge advice:
- Provide clear return precautions: worsening breathlessness, chest pain, syncope or collapse.
- Arrange follow-up chest imaging according to local pleural pathway.
- Avoid air travel until radiological resolution and specialist advice.
- Advise smoking cessation, as smoking significantly increases recurrence risk.
- Do not scuba dive after spontaneous pneumothorax unless definitively treated and cleared by a specialist diving medicine service.
🚨 Tension Pneumothorax:
- Emergency! Needle decompression → chest tube. Signs: severe distress, deviated trachea, distended neck veins, hypotension.
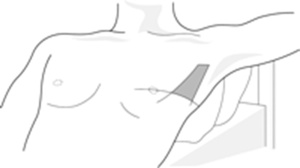
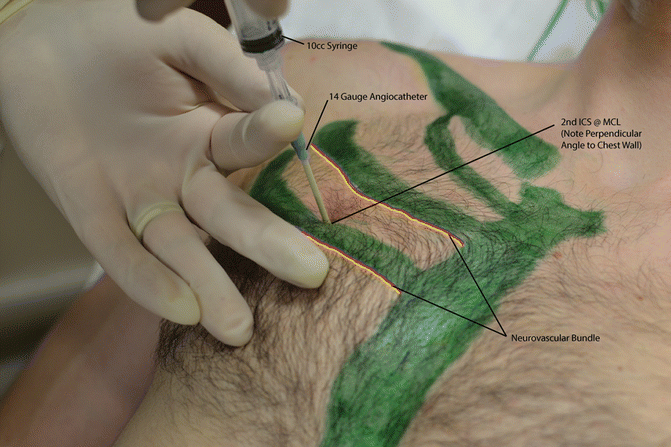
- Needle Decompression of Tension PTX Do not wait for imaging if the patient is unstable. Modern trauma teaching often uses 4th or 5th ICS, just anterior to the mid-axillary line. This is around the level of the nipple in males / inframammary fold area, but always count ribs if possible. Alternative is 2nd ICS mid-clavicular line, but failure rates can be higher because the chest wall is thicker and landmarking is often poor. Current sources describe both sites, with 4th/5th ICS anterior-to-mid-axillary or mid-axillary region increasingly preferred in trauma algorithms. Use a long large-bore cannula, often 14G/10–14G depending on local kit. Insert perpendicular to chest wall, just above the rib. Advance until air escapes / “hiss” is heard. Advance catheter over needle into pleural space. Remove needle, leave cannula in place.
Landmarks
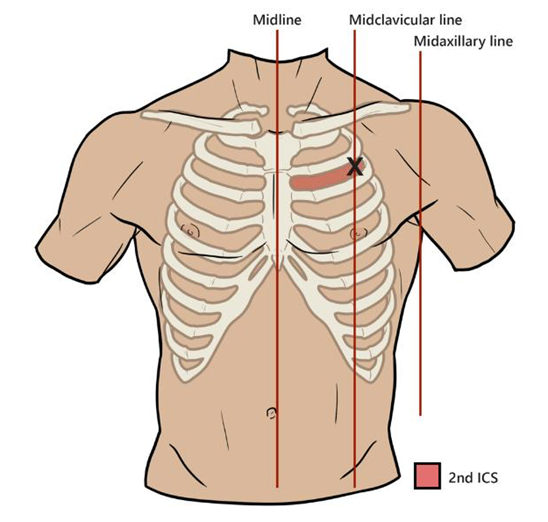
⚠️ Complications
- 💨 Persistent air leak → may need thoracic surgery.
- 🦠 Infection (chest drain in situ).
- 🔁 Recurrence (esp. smokers, tall males).
📚 References
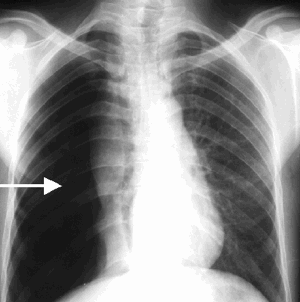
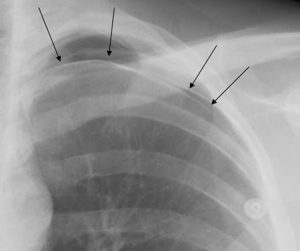
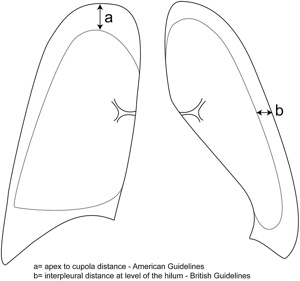
Cases - Pneumothorax (with size & management detail)
- Case 1 - Primary spontaneous 🌬️: A 22-year-old tall, slim man presents with sudden-onset left pleuritic chest pain and dyspnoea while at rest. No past medical history. Exam: hyper-resonance and absent breath sounds over the left chest. CXR: visible pleural line, 2 cm from the chest wall at the level of the hilum. Diagnosis: moderate primary spontaneous pneumothorax. Managed initially with needle aspiration; if unsuccessful, a chest drain would be placed.
- Case 2 - Secondary spontaneous 🫁: A 65-year-old man with GOLD stage 3 COPD presents with acute breathlessness and pleuritic pain. O₂ sats 85% on air. Exam: reduced breath sounds, hyper-resonance over right chest. CXR: right pneumothorax, 3 cm rim at the hilum. Diagnosis: large secondary pneumothorax. Managed with urgent chest drain insertion plus supplemental high-flow oxygen (if not hypercapnic).
- Case 3 - Traumatic / iatrogenic ⚡: A 34-year-old woman develops acute chest pain and breathlessness after insertion of a subclavian central line. Exam: tachypnoea, trachea central, reduced right-sided air entry. CXR: small right pneumothorax (<1 cm rim at hilum). Diagnosis: small iatrogenic pneumothorax. As she is stable and asymptomatic, managed with observation and repeat CXR in 24 hours.
Teaching Point 🩺: Size matters:
- Primary spontaneous PTX: <2 cm & stable → observe; ≥2 cm or breathless → aspirate (then chest drain if failed).
- Secondary spontaneous PTX: ≥2 cm or symptomatic → chest drain. 1–2 cm → attempt aspiration. <1 cm → admit, observe, and give O₂.
- Iatrogenic/traumatic PTX: often small and asymptomatic → observe; but if symptomatic or large, treat as above.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
