| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
ECG - NSTEMI
Related Subjects: |ECG Basics |ECG Axis |ECG Analysis |ECG LAD |ECG RAD |ECG Low voltage |ECG Pathological Q waves |ECG ST/T wave changes |ECG LBBB |ECG RBBB |ECG short PR |ECG Heart Block |ECG Asystole and P wave asystole |ECG QRS complex |ECG ST segment |ECG: QT interval |ECG: LVH |ECG RVH |ECG: Bundle branch blocks |ECG Dominant R wave in V1 |ECG Acute Coronary Syndrome |ECG Narrow complex tachycardia |ECG Ventricular fibrillation |ECG Regular Broad complex tachycardia |ECG Crib sheets
Typical ECG Findings in NSTEMI
Core Definition NSTEMI = myocardial infarction without persistent ST elevation on ECG but with troponin rise and ischaemic symptoms or ECG changes.
Key Message ECG is abnormal in ~80–90% of NSTEMI cases, but ~10–20% can have a completely normal or non-specific ECG → troponin is diagnostic. Changes are often dynamic → repeat ECG every 15–30 min if pain ongoing or high clinical suspicion.
Most Common & Typical ECG Changes
- ST-segment depression – most frequent and characteristic finding
- Horizontal or downsloping ≥0.5 mm (0.05 mV) in ≥2 contiguous leads
- Most common in lateral leads (I, aVL, V5–V6) or inferior leads (II, III, aVF)
- Can be widespread (anterior + lateral + inferior) in multivessel disease
- T-wave inversion – deep symmetric inversion (>2 mm) in ≥2 contiguous leads
- Common in anterior (V2–V4), lateral (I, aVL, V5–V6) or inferior leads
- Wellens' pattern (deeply inverted or biphasic T waves in V2–V3) indicates critical proximal LAD stenosis → urgent angiography
- Transient / brief ST elevation that resolves quickly before ECG capture
- Indicates unstable plaque with transient occlusion → still classified as NSTEMI if no persistent elevation
- Other supportive findings
- Hyperacute (tall, broad, peaked) T waves early in ischaemia
- Poor R-wave progression or loss of R waves (anterior infarction)
- New left bundle branch block (LBBB) with ischaemic symptoms → treat as STEMI equivalent
- Reciprocal ST depression opposite to subtle elevation
- Arrhythmias (sinus tachycardia, new atrial fibrillation, ventricular ectopics)
High-Risk ECG Patterns in NSTEMI
- Widespread ST depression in ≥3 leads + ST elevation in aVR → left main or triple-vessel disease
- Wellens' syndrome (deeply inverted or biphasic T waves V2–V3) → high-risk proximal LAD lesion
- Dynamic changes on serial ECGs (worsening depression, new T inversion)
- ST depression in multiple territories → multivessel ischaemia
Important Clinical Notes & Pitfalls
- Normal ECG does NOT exclude NSTEMI → always interpret with symptoms + troponin
- NSTEMI vs unstable angina → troponin elevation distinguishes (NSTEMI = troponin positive)
- Differentials for ST depression / T inversion: LVH with strain, digoxin effect, hypokalaemia, pulmonary embolism, takotsubo cardiomyopathy, myocarditis
- Always compare to previous ECGs if available
- Repeat ECG frequently during ongoing pain or if initial ECG non-diagnostic
Management Implications of ECG
- High-risk ECG (Wellens', widespread depression + aVR elevation, dynamic changes) → immediate invasive strategy (<2 hours to cath lab)
- Intermediate-risk → early invasive (<24 hours)
- Low-risk or non-specific changes → selective invasive or conservative approach
Clinical Pearl for Exams / OSCE / MCQ
- Most common ECG in NSTEMI → ST depression ± T-wave inversion in lateral or inferior leads
- Wellens' pattern or ST elevation in aVR + widespread depression → high-risk → urgent angiography
- Normal ECG does NOT rule out NSTEMI → rely on clinical picture + high-sensitivity troponin
- Always repeat ECG and compare serial changes in suspected ACS
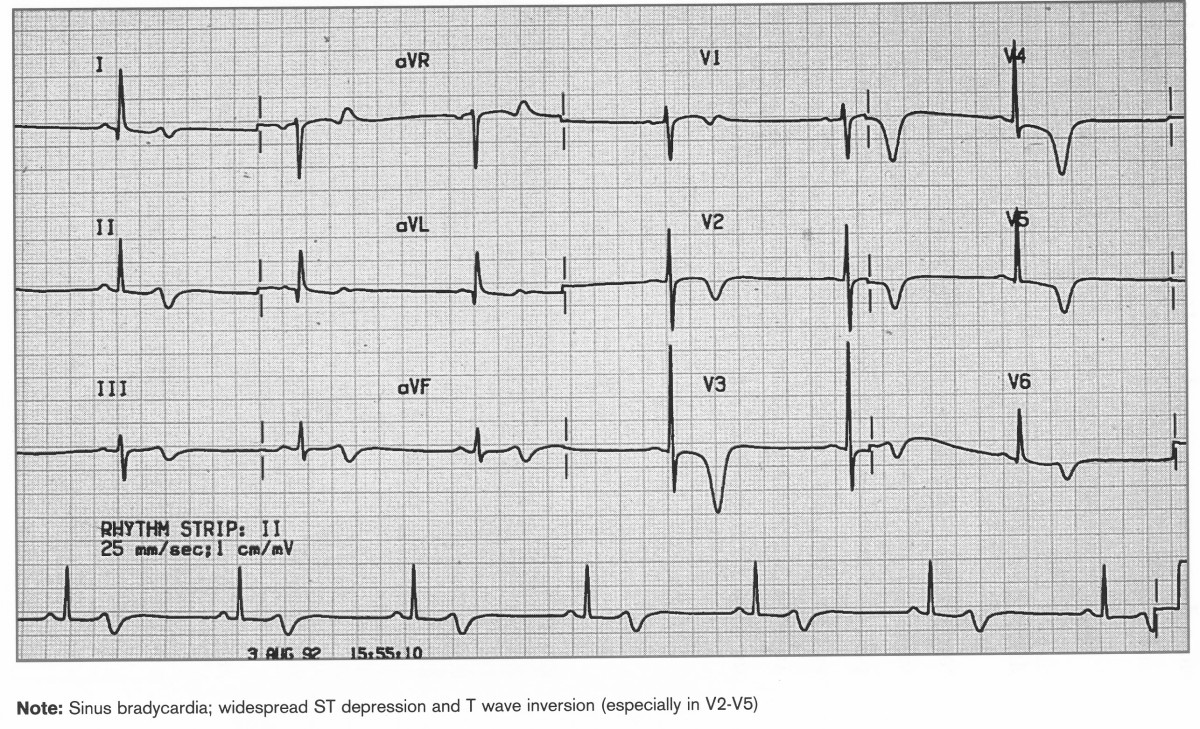
Chest pain at rest and ECG shows Sinus bradycardia, ST depression widespread, T wave inversion V2-5. Wellens Syndrome
Sources (2026)
- ESC Guidelines: Acute Coronary Syndromes (2023, minor 2025 updates)
- AHA/ACC NSTE-ACS Guideline (2022, reaffirmed 2025)
- NICE CG95 / NG185: Chest pain of recent onset (updated 2025)
- Life in the Fast Lane ECG Library (2026 updates)
- UpToDate: ECG in NSTEMI (2026)
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
