| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Myelofibrosis 🩸
Related Subjects: |Iron deficiency Anaemia |Haemolytic anaemia |Macrocytic anaemia |Megaloblastic anaemia |Microcytic anaemia |Myelodysplasia |Myelofibrosis |Hereditary Spherocytosis |Hereditary Elliptocytosis |Haemophilia A |Haemophilia B |Haemolytic anaemia |Heme |Globins |Red blood cells |White blood cells |Lymphocytes |Platelets |Cryoprecipitate |Fresh Frozen Plasma |Blood Cell Maturation |Blood film interpretation |Reticulocytes
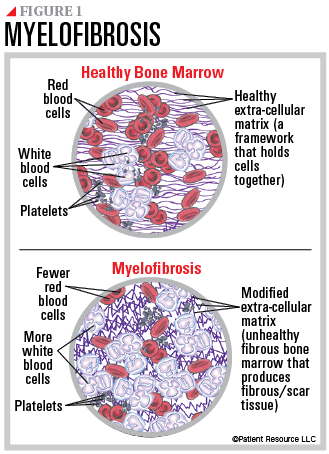
🩸 Primary myelofibrosis is a myeloproliferative neoplasm where bone marrow is progressively replaced by fibrous tissue (reticulin and collagen). This leads to ineffective haematopoiesis, extramedullary haematopoiesis, and massive splenomegaly. ⚠️ A minority of cases transform to acute myeloid leukaemia (AML).
📖 About
- One of the BCR-ABL negative myeloproliferative neoplasms (alongside polycythaemia vera and essential thrombocythaemia).
- Characterised by marrow fibrosis, abnormal megakaryocyte proliferation, and extramedullary haematopoiesis.
- Median age of onset: 60–70 years.
- Can be primary or evolve secondarily from polycythaemia vera / essential thrombocythaemia.
🧬 Aetiology / Pathogenesis
- Clonal proliferation of megakaryocytes → release of platelet-derived growth factor (PDGF) and TGF-β → marrow fibrosis.
- Haematopoiesis shifts to spleen and liver → massive hepatosplenomegaly.
- Mutations: JAK2 V617F (~50%), CALR (~30%), MPL (~10%).
- Complications: anaemia, splenic infarction, portal hypertension, AML transformation (~10–20%).
🩺 Clinical Features
- Constitutional symptoms: fever, night sweats, weight loss (“B symptoms”).
- Massive splenomegaly (often palpable well below costal margin).
- Hepatomegaly (extramedullary haematopoiesis).
- Anaemia-related symptoms: fatigue, dyspnoea.
- Bone pain (marrow expansion / fibrosis).
- Complications: infections, gout (hyperuricaemia), thrombosis, bleeding.
🔍 Investigations
Classic finding = leukoerythroblastic blood film with “teardrop” poikilocytes. 🧐
- FBC: anaemia; early stages → raised WCC and platelets; later → pancytopenia.
- Blood film: teardrop cells, nucleated RBCs, immature granulocytes, giant platelets.
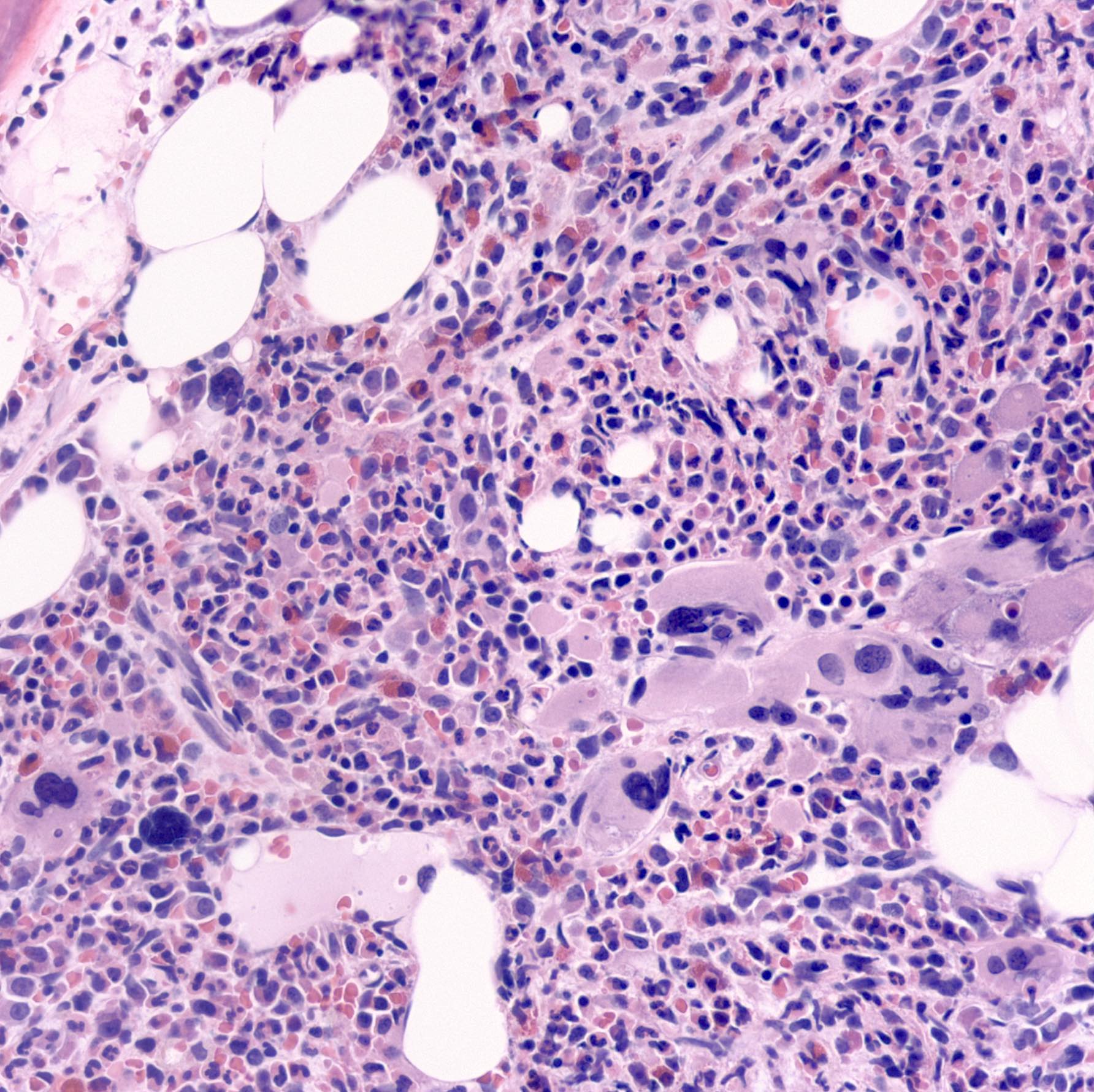
- Bone marrow: “dry tap” (aspiration failure); trephine biopsy shows fibrosis.
- Cytogenetics: no Philadelphia chromosome (distinguishes from CML).
- Raised LDH and uric acid (cell turnover).
- LAP score: normal or ↑ (low in CML).
🔎 Differential: Myelofibrosis vs CML
- Myelofibrosis: marrow fibrosis, teardrop cells, splenomegaly, ↑/↓ LAP, no BCR-ABL.
- CML: marked leucocytosis, basophilia, BCR-ABL fusion gene, ↓ LAP score.
💊 Management
- Supportive: transfusions, folate, allopurinol (prevent gout).
- Hydroxycarbamide: reduces splenomegaly and blood counts.
- JAK2 inhibitors (e.g., ruxolitinib): reduce symptoms and splenomegaly.
- Splenectomy / irradiation: palliative for massive splenomegaly.
- Allogeneic stem cell transplant: only curative option; reserved for younger patients with high-risk disease.
- Median survival: ~3–5 years (longer in indolent disease, shorter in aggressive forms).
- Common causes of death: infection, haemorrhage, AML transformation.
📚 References
Cases - Myelofibrosis
- Case 1 - Splenomegaly and Cytopenia: A 68-year-old man presents with weight loss, night sweats, and early satiety. Exam: massive splenomegaly. FBC: Hb 9.0 g/dL, WCC 4.0 ×10⁹/L, platelets 80 ×10⁹/L. Blood film shows tear-drop poikilocytes (dacrocytes). Bone marrow aspirate is “dry tap”; trephine biopsy shows fibrosis. Diagnosis: Primary myelofibrosis.
- Case 2 - Post-Polycythaemia Vera Myelofibrosis: A 72-year-old woman with a 12-year history of polycythaemia vera now develops progressive anaemia, night sweats, and bone pain. Spleen is palpable 12 cm below costal margin. Bloods: pancytopenia with leukoerythroblastic film. Diagnosis: Secondary myelofibrosis following PV.
- Case 3 - Young Adult with Constitutional Symptoms: A 40-year-old man presents with severe fatigue, weight loss, and bone pain. FBC: Hb 10.5 g/dL, WCC 18 ×10⁹/L, platelets 600 ×10⁹/L. JAK2 mutation positive. Film shows tear-drop red cells, nucleated RBCs, and immature myeloid cells. Diagnosis: Myelofibrosis (proliferative phase, JAK2-positive).
Teaching Commentary 🌿
Myelofibrosis is a myeloproliferative neoplasm where clonal proliferation of haematopoietic stem cells leads to cytokine-driven bone marrow fibrosis. Blood film shows a leukoerythroblastic picture with tear-drop RBCs. Patients often have constitutional symptoms (fever, sweats, weight loss), massive splenomegaly (extramedullary haematopoiesis), and cytopenias. Mutations: JAK2, CALR, MPL. Prognosis is variable, with risk of transformation to AML. Management: - Supportive (transfusions, hydroxycarbamide for cytoreduction), - JAK inhibitors (ruxolitinib) for splenomegaly/symptoms, - Allogeneic stem cell transplantation in fit younger patients (curative option).
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
