| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Anatomy and Physiology of the Oesophagus
Related Subjects: |AP of the Oesophagus |AP of the Diaphragm |AP of the Large Bowel (Colon, Rectum, Anal Canal) |AP of Small Bowel |AP of the Biliary system |AP of the Bone Marrow |AP of the Eye |AP of the Pharynx |AP of the Larynx |AP of the Ear |AP of the Nose |AP of Male Genitalia |AP of the Breast |AP of the Stomach |AP of the Rectum |AP of the Spleen
🦴 Anatomy of the Oesophagus
The oesophagus is a muscular tube (~25 cm long) that transports swallowed material from the pharynx to the stomach. It begins at the pharyngoesophageal junction (lower border of the cricoid cartilage, C6) and ends at the gastro-oesophageal junction (GOJ) where squamous mucosa transitions to columnar gastric mucosa (the Z-line). Beyond being a “pipe”, it is a finely coordinated motor organ: it initiates peristalsis, generates a barrier against reflux, and coordinates sphincter relaxation to allow safe bolus transit. 🌊
📍 Position, Course, and Key Levels
- General course: Descends in the neck and posterior mediastinum, lying posterior to the trachea and anterior to the vertebral column, then passes through the diaphragm to join the stomach.
- Diaphragmatic passage: traverses the oesophageal hiatus at T10.
Mnemonic: “I 8 10 Eggs At 12” → IVC T8, Oesophagus T10, Aorta T12 - Left atrial relation: In the thorax, the oesophagus lies close behind the left atrium (important for TOE/TEE and for symptoms from LA enlargement).
- Clinical landmarks for endoscopy: distances are often measured from the incisors to locate lesions/strictures.
🏷️ Anatomical Divisions
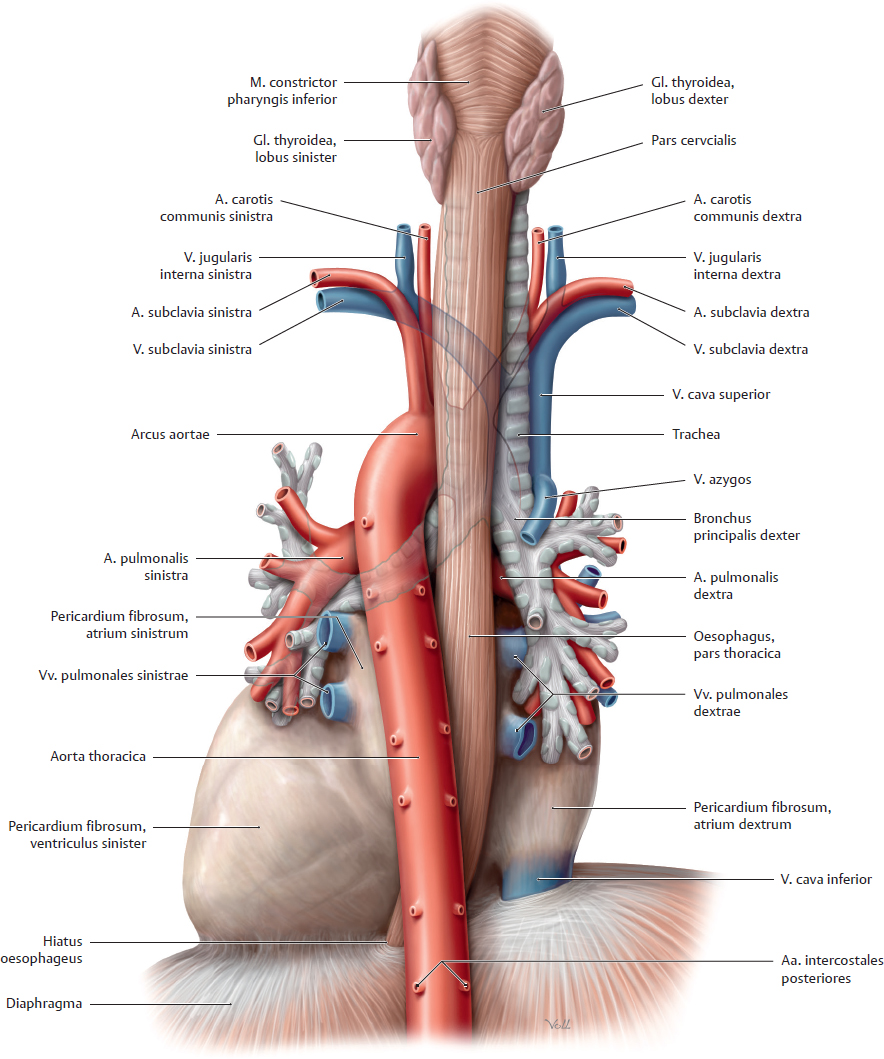
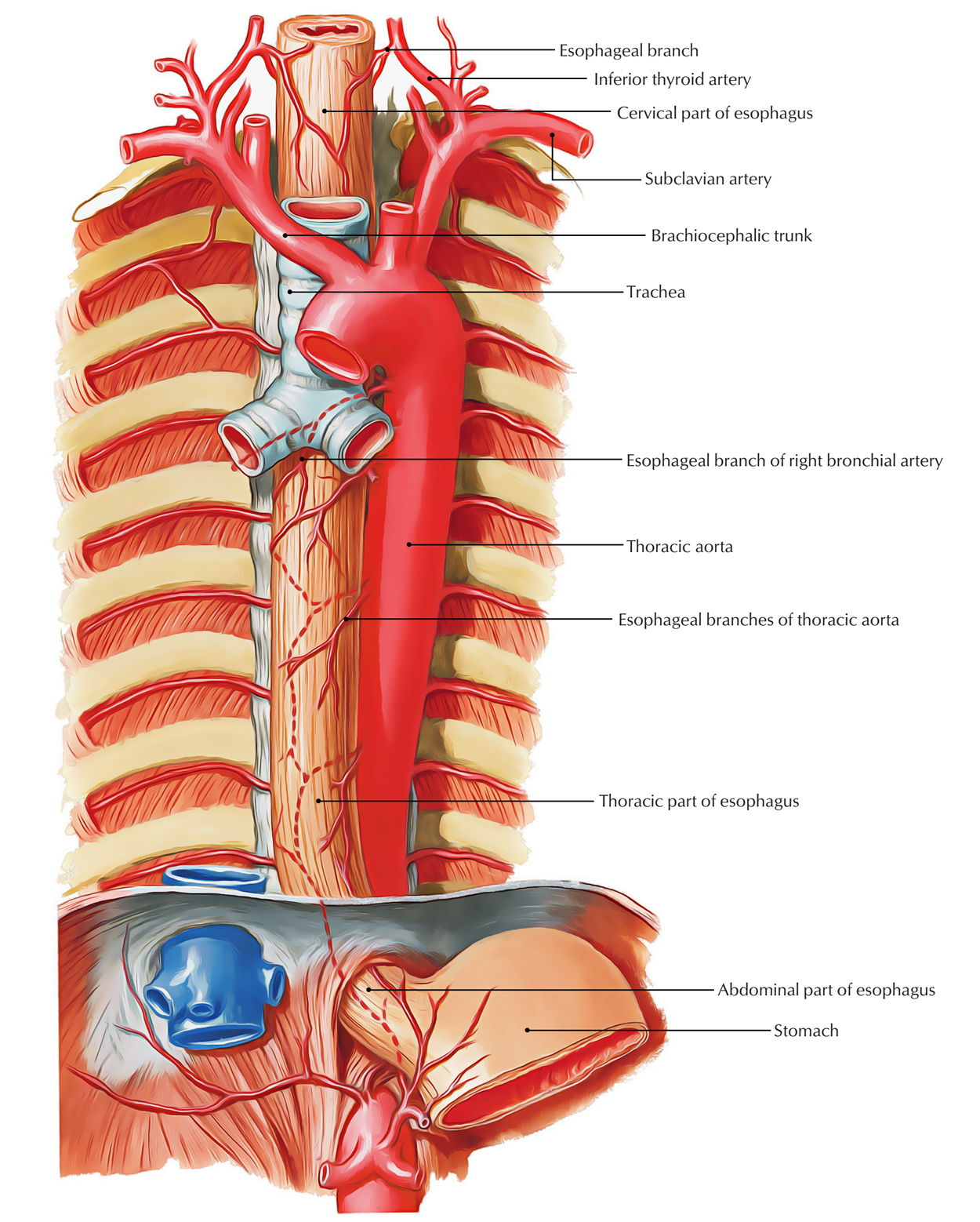
- Cervical oesophagus: Begins at C6 → thoracic inlet. Closely related to the trachea anteriorly and vertebral bodies posteriorly.
- Thoracic oesophagus: Thoracic inlet → diaphragm. Traverses the posterior mediastinum; intimately related to the aortic arch and left main bronchus (sites of narrowing).
- Abdominal oesophagus: Short (~1–2 cm) segment below the diaphragm → GOJ and gastric cardia.
🧭 Relations (High-yield Anatomy)
- Anterior: trachea (upper), then left main bronchus, then pericardium/left atrium (mid-lower thorax).
- Posterior: vertebral column; thoracic duct; azygos system (regional).
- Right side: azygos vein, mediastinal pleura (regional).
- Left side: aortic arch/descending thoracic aorta and mediastinal pleura (regional).
- At the hiatus: diaphragmatic crura form an external “pinch-cock” effect that contributes to the anti-reflux barrier.
🧩 Layers of the Oesophageal Wall (Structure ↔ Function)
- Mucosa: Non-keratinised stratified squamous epithelium - abrasion-resistant for bolus transit.
Clinical: chronic reflux can drive metaplasia to columnar epithelium (Barrett’s). - Submucosa: elastic tissue with mucous glands → lubrication and protection; contains the submucosal (Meissner) plexus.
- Muscularis externa: two coordinated layers generate peristalsis:
- Inner circular layer: constricts behind the bolus.
- Outer longitudinal layer: shortens the segment ahead of the bolus, reducing resistance.
- Muscle type gradient: upper 1/3 skeletal, middle 1/3 mixed, lower 1/3 smooth - the anatomical basis for the transition from voluntary to involuntary propulsion.
- Adventitia: outer connective tissue anchoring the oesophagus to surrounding structures (note: unlike the stomach, much of the oesophagus is not fully peritonealised).
🚪 Sphincters & the Anti-reflux Barrier
The oesophagus has two functional sphincters: the upper oesophageal sphincter (UES) prevents air entry and aspiration, while the lower oesophageal sphincter (LES) and diaphragmatic hiatus create a high-pressure zone that prevents reflux. Importantly, the LES is not a discrete “ring” like a valve; it is a physiological high-pressure segment shaped by smooth muscle tone, the diaphragm, and the angle of the GOJ.
- UES: largely the cricopharyngeus muscle.
- At rest: tonically contracted → prevents aerophagia and reflux into pharynx.
- During swallow: relaxes and opens in synchrony with pharyngeal contraction.
- LES / GOJ complex:
- Basal tone prevents gastric content reflux.
- Relaxation is triggered by swallow-induced inhibitory neurons (NO/VIP mediated).
- Additional components: diaphragmatic crura, the angle of His, and the intra-abdominal oesophageal segment (positive pressure zone).
- Failure contributes to GORD/GERD, oesophagitis, stricture, and Barrett’s.
🩸 Blood Supply, Venous Drainage, Lymphatics & Innervation
- Arterial supply (segmental):
- Cervical: inferior thyroid artery branches.
- Thoracic: oesophageal branches from thoracic aorta ± bronchial arteries.
- Abdominal: left gastric artery ± inferior phrenic branches.
- Venous drainage:
- Cervical: inferior thyroid veins.
- Thoracic: azygos/hemiazygos system.
- Abdominal: left gastric vein → portal vein.
- Key clinical concept: the distal oesophagus is a site of porto-systemic anastomosis → oesophageal varices in portal hypertension.
- Lymphatics: follow segmental pattern (cervical → deep cervical nodes; thoracic → posterior mediastinal; distal → left gastric/celiac).
Clinical: this contributes to early lymphatic spread of oesophageal cancer and “skip” metastases. - Innervation:
- Vagus nerve: major parasympathetic control of peristalsis and sphincter function.
- Enteric nervous system: myenteric (Auerbach) plexus coordinates smooth muscle contraction/relaxation.
- Sympathetic: modulates blood flow and can influence motility (stress-related symptom exacerbation).
- Pain referral: visceral afferents can refer discomfort retrosternally (reflux/oesophagitis can mimic cardiac pain).
⚙️ Physiology of Swallowing (Deglutition)
Swallowing is a coordinated sequence that protects the airway while propelling a bolus efficiently into the stomach. It has oral (voluntary), pharyngeal (reflex), and oesophageal (reflex) phases. The “swallowing centre” in the medulla coordinates cranial nerves and triggers a wave of peristalsis while transiently inhibiting respiration to prevent aspiration.
- Oral phase (voluntary): tongue propels bolus posteriorly → triggers swallow reflex.
- Pharyngeal phase (reflex):
- Soft palate elevates to close nasopharynx.
- Larynx elevates and vocal cords adduct; epiglottis helps protect the airway.
- UES relaxes and opens; pharyngeal constrictors push bolus into oesophagus.
- Oesophageal phase (reflex): coordinated peristaltic wave + LES relaxation to allow entry into stomach.
🌊 Peristalsis & Motility (How the bolus moves)
- Primary peristalsis: initiated by swallowing; propagates from UES to LES.
- Secondary peristalsis: triggered by oesophageal distension/residual bolus; important for “clearing” refluxed acid.
- Mechanics: circular muscle contraction behind bolus + longitudinal shortening ahead reduces lumen resistance.
- Neurotransmitters:
- Excitatory: acetylcholine/substance P → contraction.
- Inhibitory: nitric oxide (NO) and VIP → relaxation (critical for LES relaxation).
🛡️ Mucosal Protection & Reflux Defence
The oesophagus is not built to tolerate acid long-term, so its defence relies on barrier mechanisms (LES + diaphragm + anatomy) and clearance mechanisms (peristalsis + saliva). When these fail or acid exposure is prolonged, inflammation and metaplastic change can occur.
- Barrier: LES tone, diaphragmatic crura, intra-abdominal oesophagus, angle of His.
- Clearance: secondary peristalsis + saliva (bicarbonate) neutralisation.
- Exposure factors: delayed gastric emptying, obesity, pregnancy, hiatus hernia, medications reducing LES tone.
📊 Physiological Narrowings (Constrictions) - High yield
These are common sites for food bolus impaction, pill injury, corrosive burns, and endoscopic “hold-ups”. They are also important radiological landmarks.
- 📌 Pharyngoesophageal junction (C6, cricoid/UES)
- 📌 Aortic arch impression (around T4)
- 📌 Left main bronchus impression (around T5/6)
- 📌 Diaphragmatic hiatus (T10)
🧪 Function at the Gastro-oesophageal Junction (Z-line & metaplasia)
- Z-line: transition from squamous oesophageal epithelium to columnar gastric epithelium.
- Barrett’s oesophagus: intestinal metaplasia from chronic reflux; increases oesophageal adenocarcinoma risk (clinical surveillance context).
- Strictures: chronic inflammation and scarring can narrow lumen → progressive dysphagia (solids then liquids).
🩺 Clinical Correlations (Anatomy + Physiology → Symptoms)
- Dysphagia:
- Oropharyngeal (transfer problem) suggests neurological disease, structural pharyngeal pathology, aspiration risk.
- Oesophageal (transport problem) suggests obstruction (stricture/cancer) or motility disorder (achalasia, spasm).
- Reflux (GORD/GERD): heartburn/regurgitation; complications include oesophagitis, strictures, Barrett’s.
- Achalasia physiology (core concept): failure of inhibitory neurons → impaired LES relaxation + absent peristalsis → dysphagia to solids and liquids, regurgitation (manometry diagnosis).
- Varices: portal hypertension → dilated submucosal veins in distal oesophagus → massive upper GI bleeding risk.
- TOE/TEE: oesophagus is a key “acoustic window” to the left atrium/mitral valve because of close posterior relation.
- Oesophageal cancer: often presents with progressive dysphagia and weight loss; common at physiological narrowings and at GOJ.
📝 Summary
The oesophagus is a 25 cm muscular conduit from C6 to the stomach that combines abrasion-resistant squamous mucosa with a sophisticated motility system. Swallowing triggers primary peristalsis and coordinated sphincter relaxation, while secondary peristalsis and saliva help clear refluxed acid. The anti-reflux barrier depends on LES tone plus diaphragmatic and anatomical supports at the GOJ; failure leads to GORD and complications such as strictures and Barrett’s. Clinically, dysphagia localises disease (transfer vs transport), and the distal oesophagus is a key porto-systemic site explaining variceal bleeding in portal hypertension.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
