| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
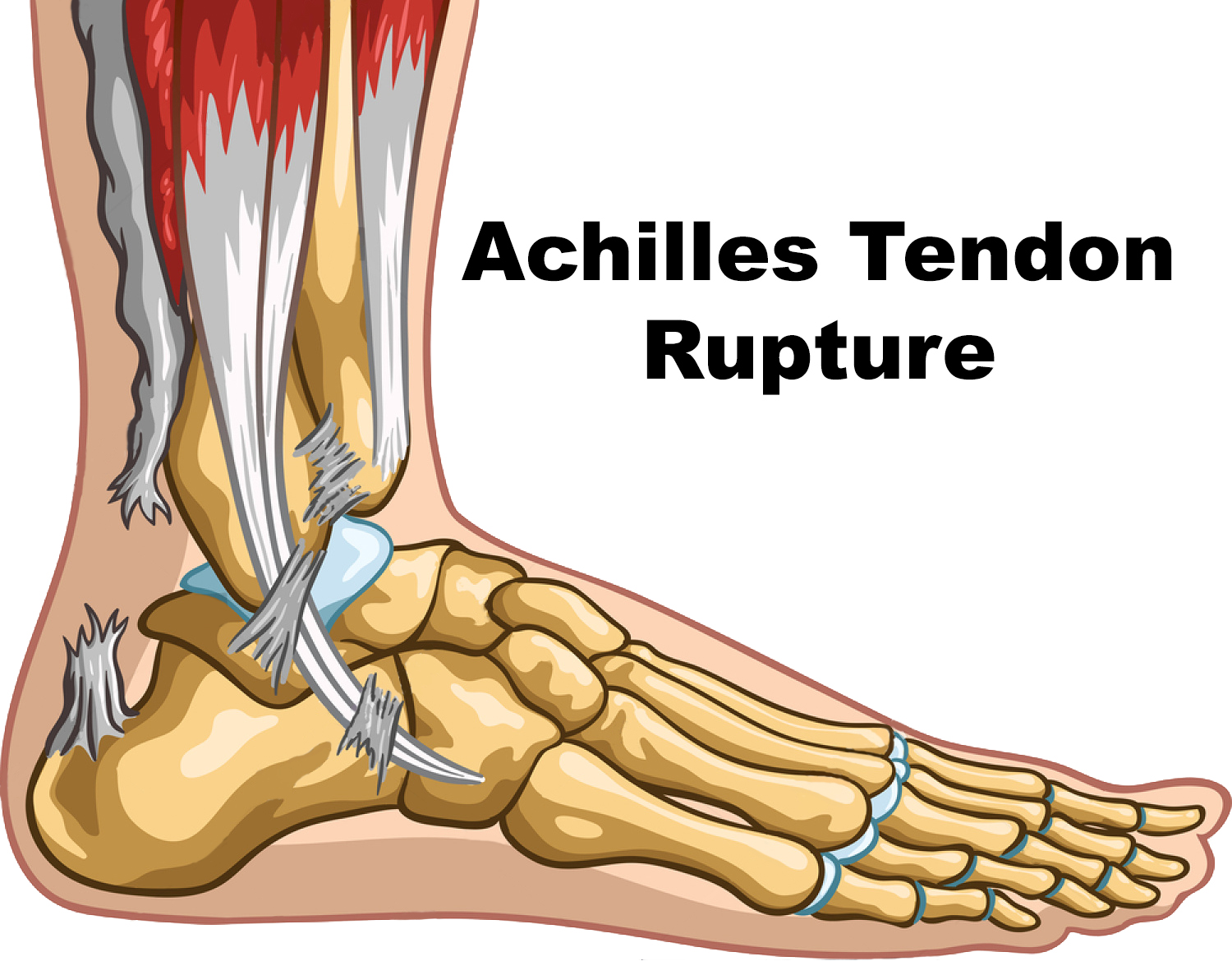
Achilles Tendon rupture
🦶 Achilles tendon rupture typically presents as a sudden “snap” or sensation of being kicked at the back of the ankle, most often during sporting activity. 🚫 Key risk factors: fluoroquinolones, corticosteroid injections, diabetes mellitus, obesity, and increasing age. 🔎 Hallmark sign: a positive Thompson calf squeeze test (absence of plantarflexion). ⚖️ Management trade-off: conservative treatment has a higher re‑rupture rate, whereas surgery lowers recurrence but increases wound and thrombotic risk.
📖 About Achilles Tendon Injury
- The Achilles is the strongest tendon in the human body, yet is vulnerable to rupture during sudden eccentric loading (e.g. jumping or sprinting).
- Often referred to as the “weekend warrior injury”, it most commonly affects middle‑aged recreational athletes.
⚠️ Aetiology & Risk Factors
- Sudden acceleration or deceleration during sport.
- Age‑related degenerative changes, exacerbated by diabetes or inflammatory arthritis.
- Medication‑associated: fluoroquinolones (e.g. ciprofloxacin) and repeated corticosteroid injections.
- Additional risks: obesity, poor conditioning, and systemic inflammatory disease.
🩺 Clinical Features
- Sudden sharp pain or audible “snap” in the posterior ankle or heel.
- Weak plantarflexion - patients may walk but cannot run or stand on tiptoe on the affected side.
- A palpable gap along the course of the tendon (best felt 2–6 cm proximal to insertion).
- Thompson test: squeezing the calf fails to produce plantarflexion.
- Partial ruptures may present subtly and still allow limited bilateral tiptoe standing.
🔍 Investigations
- Ultrasound: first‑line investigation; dynamic and readily identifies rupture location and severity.
- MRI: reserved for indeterminate cases or pre‑operative planning.
💊 Management
- Non‑surgical: functional bracing or boot immobilisation in plantarflexion; appropriate for partial tears or less physically active patients.
- Surgical repair: end‑to‑end tendon suturing; preferred in complete ruptures and younger, active individuals. Enables earlier rehabilitation but carries wound and DVT risk.
- Rehabilitation: physiotherapy is essential for all patients. Gradual strengthening, stretching, and proprioceptive training; return to sport typically takes 6–12 months.
⚡ Complications
- Re‑rupture (higher with conservative management).
- Wound complications, infection, or adhesions following surgery.
- Chronic calf weakness or muscle atrophy.
- Venous thromboembolism related to immobilisation.
🩺 Case 1 – Sudden Sports Injury
A 34‑year‑old man experiences a sudden “pop” in the posterior ankle while playing football, followed by pain and difficulty walking. Examination reveals swelling, a positive Thompson’s test, and inability to stand on tiptoe.
Management: 🏥 Immobilisation in plantarflexion (cast or functional brace), urgent orthopaedic referral. Surgical repair often advised for young, active patients. Early physiotherapy is essential.
Avoid: ❌ Misdiagnosis as a simple ankle sprain; avoid weight‑bearing until stabilised.
🩺 Case 2 – Older Patient on Steroids
A 65‑year‑old man on long‑term prednisolone for COPD presents with sudden ankle pain after stepping off a curb. Examination reveals a palpable tendon gap and weak plantarflexion.
Management: 💊 Non‑surgical functional bracing may be appropriate given comorbidities, with analgesia and physiotherapy. Consider surgery if functionally independent and fit.
Avoid: ❌ Unreviewed continuation of steroids or fluoroquinolones; prolonged immobilisation without VTE prophylaxis.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
