| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cellulitis and Erysipelas ✅
Related Subjects: |Cellulitis |Impetigo |Pyoderma gangrenosum |Pemphigus Vulgaris |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Necrotising fasciitis |Gas Gangrene (Clostridium perfringens) |Anatomy of Skin |Skin Pathology and lesions |Skin and soft tissue and bone infections |Lymphangitis
🦵 Cellulitis is an acute bacterial infection of the dermis and subcutaneous tissue causing hot, tender, spreading erythema. It is usually unilateral and most often due to Streptococcus pyogenes (non-purulent cellulitis) or Staphylococcus aureus (more likely if purulent/abscess). “Bilateral red legs” are common in practice, but if both legs are red and cool/normal temperature (or mainly itchy/scaly), cellulitis is less likely-think venous eczema/stasis dermatitis or lipodermatosclerosis.
🧠 Pathophysiology (why it looks the way it does)
- Entry point (often tiny): toe-web fissures (tinea pedis), eczema cracks, ulcers, insect bites, trauma, injection sites.
- Innate immune response drives erythema, warmth and swelling: vasodilatation + capillary leak → oedema; neutrophil recruitment → tenderness.
- Lymphatic involvement is common: lymphangitis (red streaks) and reactive lymphadenopathy; recurrent episodes can damage lymphatics → chronic oedema → higher recurrence risk.
🦠 Common pathogens
- Non-purulent cellulitis: usually β-haemolytic streptococci (esp. Group A).
- Purulent infection/abscess: more likely Staphylococcus aureus.
- Diabetic/ischaemic limb or foul-smelling wounds: consider polymicrobial infection (including anaerobes) and seek senior/micro advice.
⚠️ Risk factors
- Skin barrier disruption: eczema, psoriasis, ulcers, athlete’s foot, trauma, surgery.
- Chronic oedema/lymphoedema, chronic venous insufficiency, obesity.
- Diabetes, peripheral arterial disease, immunosuppression, liver/renal disease.
- Previous cellulitis episode (risk of recurrence increases).
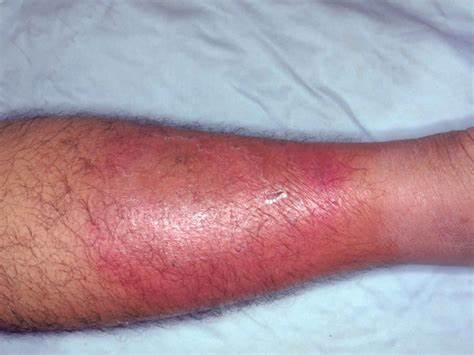
👩⚕️ Clinical features
- Acute onset of unilateral erythema, warmth, swelling, and tenderness.
- Ill-defined margins are typical (erysipelas is usually more sharply demarcated).
- Possible systemic features: fever, rigors, malaise, tachycardia.
- Look for: toe-web maceration (tinea), eczema, ulcers, bite marks, wounds, foreign body.
- 🖊️ Practical tip: mark the edge with a pen + date/time to monitor spread.
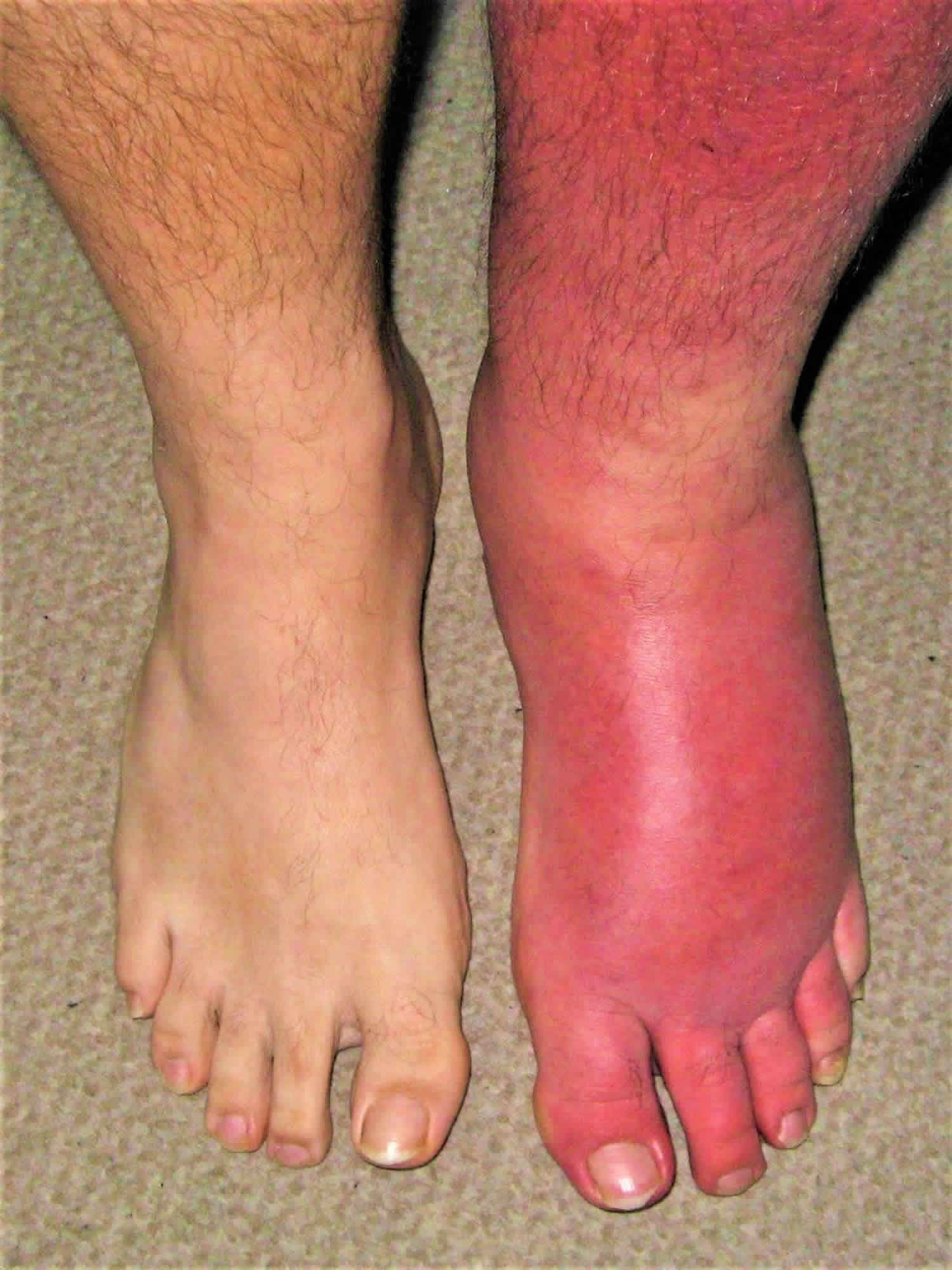
🧩 Differential diagnosis (common mimics)
- Venous eczema / stasis dermatitis (often bilateral, itchy, scaly, chronic oedema, less tender/less hot).
- Lipodermatosclerosis (chronic venous disease; “inverted champagne bottle” legs; painful, indurated, brown haemosiderin staining).
- DVT (unilateral swelling/pain; skin may be less erythematous/hot than cellulitis; consider Wells + ultrasound if uncertain).
- Superficial thrombophlebitis (linear tender cord along vein).
- Gout/pseudogout (very focal joint pain/swelling; systemic upset can mimic infection).
- Contact dermatitis/drug eruption (itch predominant; often sharply demarcated; vesicles).
- Erythema nodosum (tender nodules, usually shins; systemic triggers).
- 🚨 Serious mimics: necrotising fasciitis, septic arthritis, osteomyelitis.
🚨 Red flags (think “not simple cellulitis”)
- Pain out of proportion, rapidly progressive swelling/erythema, skin necrosis, bullae, crepitus.
- Marked systemic illness: hypotension, confusion, persistent tachycardia, high NEWS2.
- Failure to improve after 24–48 hours of appropriate antibiotics (some early progression can occur, but trend should stabilise).
- High-risk sites: face/orbit, hand, perineum.
- Immunocompromise, severe PAD/critical limb ischaemia, diabetic foot with deep infection signs.
🧪 Diagnostic approach (UK practical)
- Cellulitis is largely a clinical diagnosis.
- Record observations (temperature, HR, BP, RR, SpO₂) and assess for sepsis.
- Check limb neurovascular status if swelling is marked.
- Assess for abscess (fluctuance/pus) - if present, incision & drainage may be key.
🔬 Investigations
- Bloods: FBC, CRP (helpful for severity/trend), U&E (antibiotic dosing/AKI risk), glucose/HbA1c if relevant.
- Blood cultures: consider if febrile/systemically unwell or immunocompromised.
- Swab: only if there is a wound, ulcer, or discharge/pus.
- Ultrasound: if abscess suspected or DVT is a realistic alternative diagnosis.
- X-ray: if concern for foreign body, gas, or osteomyelitis (clinical context dependent).
📊 Cellulitis severity (Eron classification) + what it means
| Class | Typical features | Practical management |
|---|---|---|
| I | No systemic toxicity; no significant comorbidity affecting treatment. | Oral antibiotics + self-care; safety-net and review if not improving. |
| II | Systemically unwell or significant comorbidity (e.g., diabetes, venous disease, chronic oedema). | Consider IV/oral depending on severity and ability to take PO; consider SDEC/ambulatory IV. |
| III | Marked systemic upset (e.g., tachycardia, tachypnoea, hypotension) or unstable comorbidities. | Hospital assessment; IV antibiotics; monitor closely; exclude deep infection. |
| IV | Sepsis or life-threatening infection (e.g., necrotising fasciitis). | Resus + urgent senior/surgical input; broad-spectrum IV antibiotics per local policy. |
🛏️ Supportive care (often forgotten, but high impact)
- 🦵 Elevate the affected limb to reduce oedema and pain.
- 🧦 Manage swelling: consider compression once acute infection is improving (and only if arterial supply is adequate).
- 💊 Analgesia (paracetamol ± NSAID if appropriate) and encourage fluids.
- 🧼 Treat the portal of entry: antifungal for tinea pedis, emollients/steroid for eczema when infection controlled, wound care for ulcers.
- 🖊️ Mark borders and document size/appearance; photos can help follow progression.
💊 Antibiotic treatment (adult) - typical UK first line
| Scenario | First choice | Penicillin allergy (examples) | Notes |
|---|---|---|---|
| Mild–moderate cellulitis (oral) | Flucloxacillin (PO) | Clarithromycin (PO) (or doxycycline depending on local guidance/patient factors) | Review if not improving within 2–3 days; course length commonly 5–7 days, extend if slow response. |
| Severe/systemically unwell (IV) | Flucloxacillin (IV) | IV alternative (e.g., clarithromycin/other per local guideline) | Switch to oral when clinically improving; reassess diagnosis if deterioration. |
| Purulence/abscess suspected | Drainage + antibiotics guided by severity | As above | Source control matters: fluctuance/pus → think abscess rather than “simple” cellulitis. |
🏥 When to admit / seek urgent specialist input
- Sepsis features or Eron class III–IV.
- Concern for necrotising fasciitis, deep abscess, septic arthritis, osteomyelitis.
- Unable to tolerate oral antibiotics, significant vomiting, poor social support, or rapid progression.
- High-risk anatomical sites (face/orbit/hand/perineum) or immunocompromised patient.
🔁 Recurrent cellulitis (prevention)
- Address modifiable risks: treat tinea pedis, optimise eczema care, reduce chronic oedema (compression/lymphoedema input), weight management.
- Consider referral for venous/lymphoedema assessment if recurrent episodes or chronic swelling.
- Some patients with frequent recurrences may need prophylactic antibiotics via local/lymphoedema pathways.
📚 References (UK)

Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
