| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Larva Currens (Strongyloides stercoralis)
Larva currens (“racing larva”) is a characteristic, rapidly migrating, itchy, serpiginous rash caused by Strongyloides stercoralis. It reflects autoinfection (larvae re-entering the host via the gut/perianal skin), which is why Strongyloides can persist for years and can become life-threatening if the patient later receives steroids or other immunosuppression. In UK practice, think of it in migrants, travellers, veterans, and anyone with eosinophilia plus intermittent GI/skin symptoms.
🦠 Organism & Life Cycle (Why it matters clinically)
- Strongyloides stercoralis is a soil-transmitted nematode (tropical/subtropical, but seen globally).
- Infective filariform larvae penetrate intact skin (often barefoot soil exposure) → bloodstream → lungs → swallowed → small intestine.
- Unique feature: autoinfection (rhabditiform larvae become filariform inside the host and re-penetrate mucosa/skin).
- Clinical implication: infection may be chronic and silent, then “explodes” into hyperinfection when immunity is suppressed (especially steroids).
🔬 Pathophysiology of Larva Currens
- Autoinfective larvae migrate within superficial dermis causing a type I hypersensitivity-type wheal/flare response.
- The rash moves fast (often several cm per hour), so lesions can appear, disappear, and reappear elsewhere over hours.
- Common sites: perianal region, buttocks, groin, lower trunk, thighs (reflecting perianal autoinfection).
Teaching point: The “speed” is the clinical giveaway: hookworm cutaneous larva migrans creeps slowly over days; larva currens races over hours.
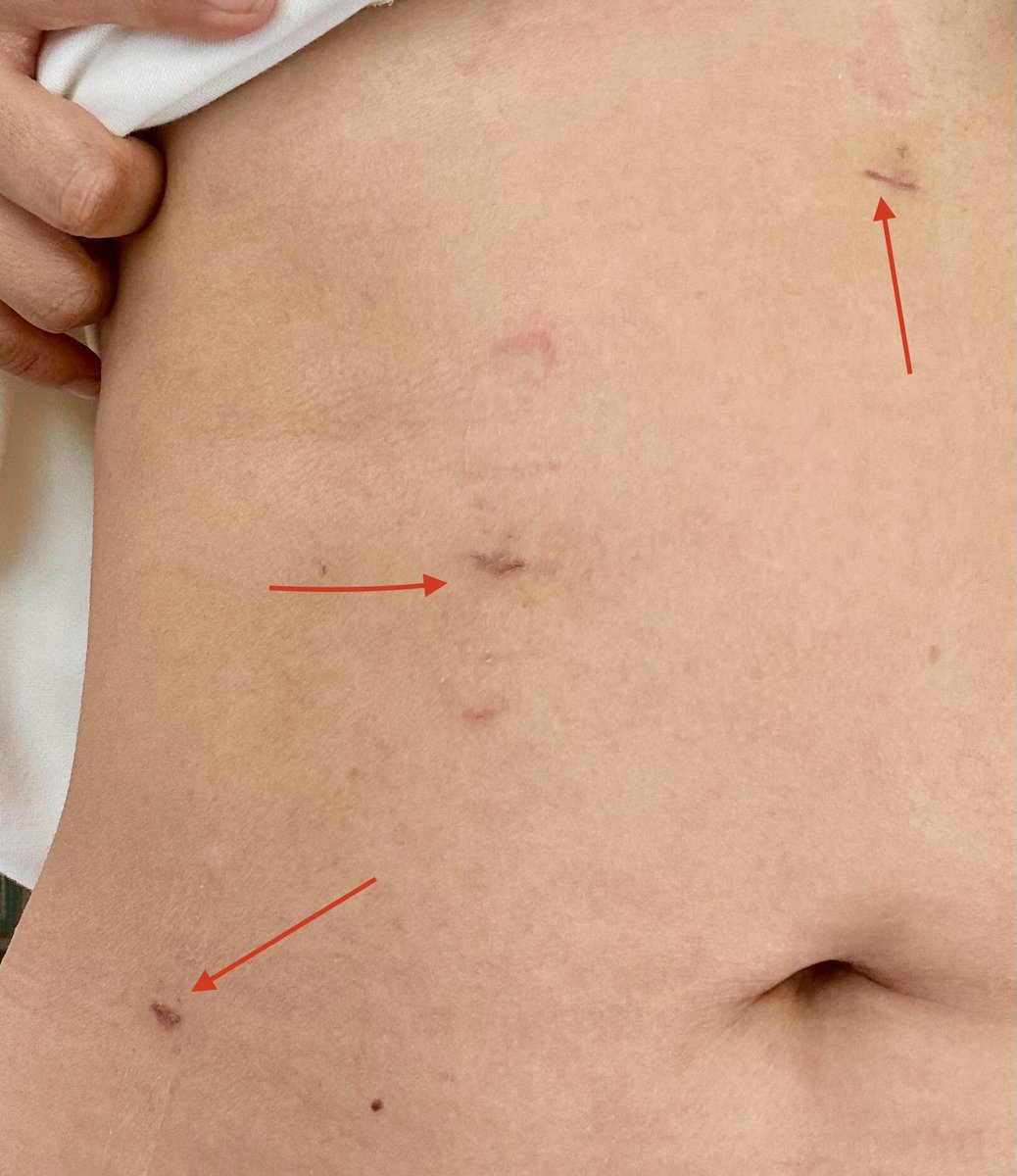
👀 Clinical Features
- Rash: erythematous, serpiginous/linear, urticarial, intensely pruritic, fleeting and migratory.
- Systemic clues: intermittent abdominal pain, diarrhoea/constipation, bloating, nausea, weight loss.
- Respiratory clues: cough/wheeze during larval migration (may mimic asthma).
- Bloods: eosinophilia is common in chronic infection (but may be absent in severe/hyperinfection or on steroids).
🚨 Red Flags: Hyperinfection & Disseminated Strongyloidiasis
- Who is at risk? Current/recent systemic corticosteroids (even short courses), transplant recipients, haematological malignancy, advanced HIV, biologics, malnutrition; consider HTLV-1 as a classic association.
- What happens? Massive increase in larval burden in GI + lungs (hyperinfection) and spread beyond (dissemination).
- Clinical picture: severe diarrhoea/ileus, GI bleeding, pneumonitis/ARDS, sepsis.
- Key danger: larvae can carry gut bacteria into the bloodstream → Gram-negative bacteraemia/meningitis.
UK practical pearl: If a patient from an exposure-risk background needs steroids/chemo/transplant work-up, screen for Strongyloides first (and treat if positive) to prevent catastrophic hyperinfection.
🧾 Differential Diagnosis (Fast vs slow “tracks”)
- Cutaneous larva migrans (hookworm): slower advancing track over days, often feet after beach/sand exposure.
- Urticaria: transient wheals but no consistent serpiginous “track” or rapid migration pattern.
- Scabies: burrows (thin, short), typical distribution (web spaces, wrists) and household spread.
- Dermographism/contact dermatitis: pattern relates to friction/exposure rather than “racing” migration.
🧪 Diagnosis (UK-friendly approach)
- Strongyloides serology (IgG ELISA): often the best single test for chronic infection.
- Stool microscopy for larvae: sensitivity is limited; send multiple samples and request concentration/culture techniques if available.
- Full blood count: eosinophilia supports the diagnosis but is not required (and may disappear in severe disease or on steroids).
- In hyperinfection: larvae may be detectable in sputum/BAL and stool; involve Micro/ID urgently.
Reasoning tip: A classic history is “intermittent itchy, migrating rash near buttocks + eosinophilia” in someone with travel/migration exposure. Don’t wait for the rash to be present on the day you examine them.
💊 Management
- First-line: Ivermectin (typical adult regimen for uncomplicated disease is 200 micrograms/kg orally, often as a single day dose or daily for 1–2 days; many clinicians repeat a dose around 14 days to cover autoinfection cycles-local protocols vary).
- Hyperinfection/dissemination: daily ivermectin and specialist management; continue until clinical improvement and repeated specimens are negative (often for at least 2 weeks beyond clearance).
- If unable to take oral therapy: urgent specialist input (alternative routes/regimens may be considered under expert guidance).
- Stop/avoid steroids if possible until treated, or treat presumptively if risk is high and immunosuppression is unavoidable.
- Supportive care: manage sepsis aggressively; consider broad-spectrum antibiotics if bacterial translocation suspected.
🛡️ Prevention & Screening (High-yield for UK wards)
- Screen (serology ± stool) in people with exposure risk before steroids, biologics, chemotherapy, transplant.
- Treat confirmed infection even if asymptomatic (because chronic carriage can later become fatal).
- Advise travellers: avoid barefoot soil exposure in endemic regions; sanitation matters.
🧠 Mini “Consultant-to-Junior” Commentary
Larva currens is a bedside clue to Strongyloides, and the key physiology is autoinfection: the parasite can keep reinfecting the host internally, so “remote travel” is still relevant years later. The rash is essentially an allergic response to larvae migrating in the superficial dermis, which is why it’s urticarial and fast-moving-a big discriminator from hookworm larva migrans. Clinically, the reason we care so much in the UK is the steroid link: immunosuppression removes the brakes on larval replication, leading to hyperinfection with Gram-negative sepsis that can be rapidly fatal. If you see eosinophilia plus intermittent GI/skin symptoms in someone with exposure risk, think “screen and treat early” rather than “watch and wait.”
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
