| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Pericardial Effusion and Tamponade ✅
Related Subjects: | Assessing Breathlessness | Acute Hypotension | Respiratory Failure | Pulmonary Embolism | Deep Vein Thrombosis | DVT/PE in Pregnancy | CTPA
💉 Cardiac tamponade is a medical emergency where rising intrapericardial pressure impairs ventricular filling → ↓ stroke volume → ↓ cardiac output → obstructive shock and cardiac arrest 🚨. 👉 Classic Beck’s triad: ↑ JVP, hypotension, muffled heart sounds (often incomplete in practice). 👉 Immediate pericardial decompression is life-saving — do NOT delay for imaging if unstable. 🩺 Point-of-care echocardiography confirms diagnosis (RA/RV diastolic collapse). ⚡ Emergency options: ultrasound-guided pericardiocentesis (first-line) or surgical drainage.
📖 Overview of Pericardial Effusion
- 💧 Pericardial effusion = fluid accumulation (serous, blood 🩸, pus 🦠, chyle).
- ⚖️ Normal volume: 10–50 mL
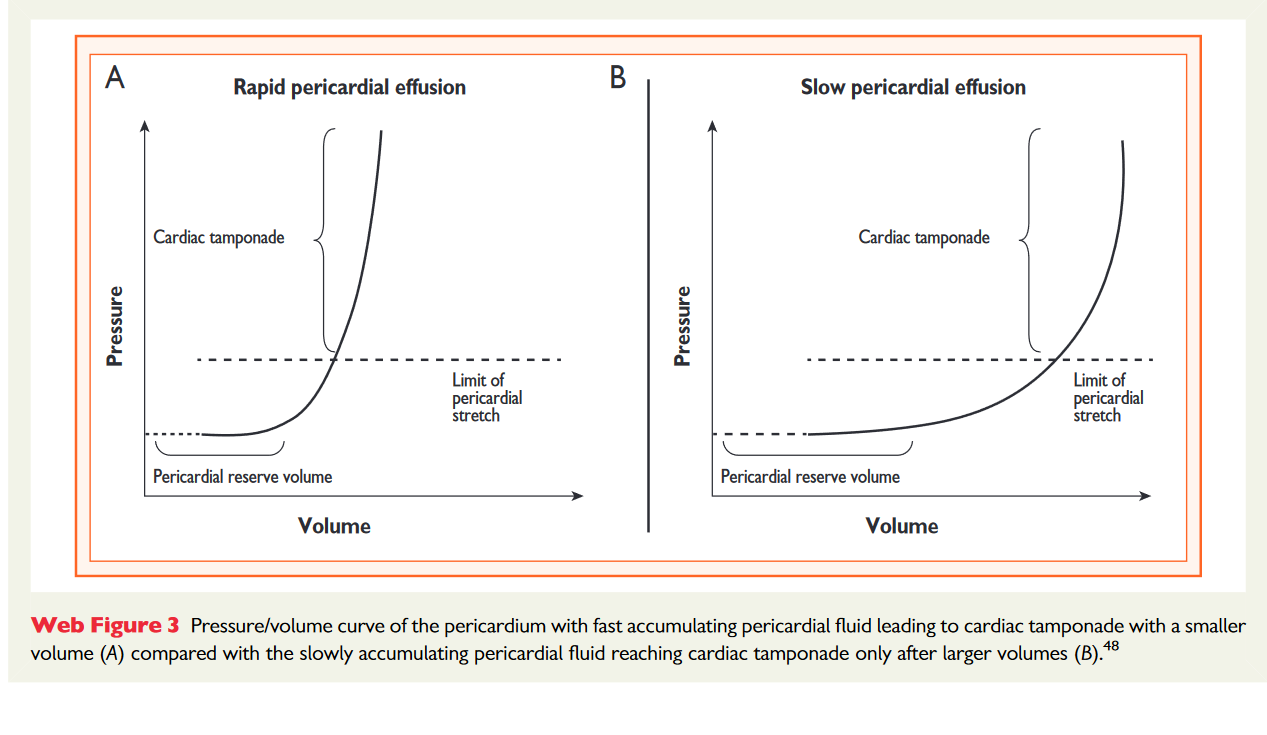
- 📈 Slow accumulation → pericardium stretches → large volumes tolerated
- ⚡ Rapid accumulation (even 100–200 mL) → sharp pressure rise → tamponade
- 🧠 Key concept: rate of accumulation matters more than absolute volume
🩺 Aetiology
- 🦠 Infective: Viral (commonest), TB (important globally), bacterial
- 🔥 Autoimmune: SLE, RA, vasculitis
- 🎗️ Malignancy: Lung, breast, lymphoma, melanoma
- 💔 Post-cardiac injury: MI (Dressler’s), surgery, trauma
- 🧪 Metabolic: Uraemia, hypothyroidism
- 🩸 Vascular: Aortic dissection, free wall rupture post-MI
- 💊 Iatrogenic: Anticoagulation → haemopericardium
📊 Classification
- ⏱️ Time: Acute / Subacute (<3 months) / Chronic (>3 months)
- 📐 Size (echo): Mild (<10 mm), Moderate (10–20 mm), Large (>20 mm)
- 🫀 Haemodynamic: No compromise / Tamponade / Effusive-constrictive
- 📍 Distribution: Circumferential vs loculated
⚠️ Causes of Tamponade (High-Yield)
- 🚑 Trauma or iatrogenic (procedures, pacing wires)
- 🎗️ Malignancy (common cause of large effusions)
- 🦠 TB (important in endemic populations)
- 🩸 Aortic dissection (life-threatening cause)
- 💔 Post-MI free wall rupture (3–10 days)
- 💊 Anticoagulation → haemopericardium
👩⚕️ Clinical Features (Effusion without Tamponade)
- Dyspnoea, fatigue, chest discomfort
- Orthopnoea, PND
- Systemic features: fever, weight loss (TB/malignancy)
- Pressure effects: dysphagia, hoarseness
💡 Pulsus paradoxus = inspiratory drop in SBP >10 mmHg (mechanism: ↑ RV filling → septal shift → ↓ LV filling)
⚠️ Always consider life-threatening differentials: PE, ACS/MI, Type A aortic dissection, tension pneumothorax
🚨 Clinical Features of Cardiac Tamponade
- Severe dyspnoea, tachycardia, hypotension → shock
- Beck’s triad:
- ↑ JVP
- ↓ BP
- 🔇 Muffled heart sounds
- ❗ Narrow pulse pressure
- ❗ Tachycardia almost universal
- ❗ Absent Y descent (distinguishes from constriction)
🔎 Investigations
- ECG: Sinus tachycardia, low voltage, electrical alternans
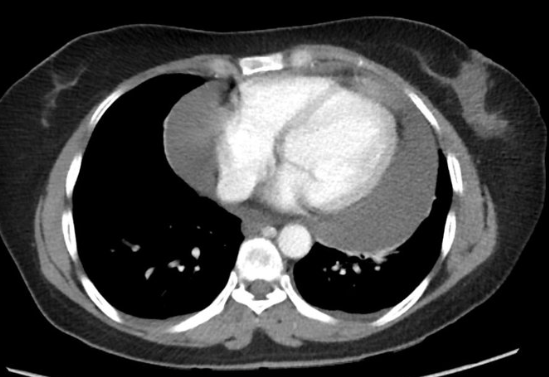
- CXR: “Water bottle” heart (large chronic effusion)
- Echo (GOLD STANDARD):
- RA/RV diastolic collapse 🚨
- Dilated non-collapsing IVC
- Swinging heart
- Bloods: FBC, CRP, U&E, TFTs, troponin
- CT/MRI: For complex/loculated effusions
- Pericardial fluid analysis: Cytology, culture, TB PCR
💊 Management (Guideline-Aligned)
🚨 Tamponade = IMMEDIATE DRAINAGE Do NOT delay for definitive diagnosis if unstable.
- 🅰️ ABC approach + oxygen
- 💧 IV fluids → temporising (↑ preload)
- 🩺 Urgent pericardiocentesis (ultrasound-guided) = first-line
- 🔪 Surgical drainage if traumatic, recurrent, or loculated
- ❗ Leave drain in situ to prevent re-accumulation
- 💊 Cause-specific treatment:
- NSAIDs + colchicine → inflammatory pericarditis
- Dialysis → uraemic
- Oncology input → malignant
- Anti-TB therapy → tuberculous
⚠️ Avoid:
- ❌ Diuretics (↓ preload → worsens tamponade)
- ❌ Positive pressure ventilation (↓ venous return)
- ❌ Delays to drainage
🩺 Case 1 — Subacute Effusion
Malignancy-related effusion → gradual symptoms, large volume tolerated. 👉 Drain if symptomatic or haemodynamic compromise.
🩺 Case 2 — Acute Tamponade
Post-surgical patient with shock → echo confirms RA collapse. 👉 Immediate drainage + surgical involvement.
🩺 Case 3 — Anticoagulation-Related
DOAC → haemopericardium → tamponade. 👉 Reverse anticoagulation + urgent drainage.
📚 References
- 2015 ESC Guidelines for the diagnosis and management of pericardial diseases 👉 Gold-standard guideline for pericardial effusion, tamponade physiology, and management strategies European Society of Cardiology (ESC)
- Resuscitation Council UK – Advanced Life Support (ALS) Guidelines 👉 Covers obstructive shock, cardiac arrest, and emergency management principles including tamponade Resuscitation Council UK ALS
- NICE Clinical Knowledge Summary (CKS): Pericarditis 👉 UK primary care–focused guidance on causes, investigation, and initial management NICE CKS Pericarditis
- NICE Guideline NG158 – Acute coronary syndromes 👉 Relevant for post-MI complications (e.g. free wall rupture → tamponade) NICE NG158
- NICE Guideline NG51 – Sepsis 👉 Important differential when patients present with shock and raised inflammatory markers NICE NG51
- Oxford Handbook of Clinical Medicine (11th Edition) 👉 Concise bedside summary of tamponade signs (Beck’s triad, pulsus paradoxus) and management
- Kumar & Clark’s Clinical Medicine (10th Edition) 👉 Detailed pathophysiology of pericardial disease and haemodynamic compromise
- UpToDate – Cardiac tamponade 👉 Comprehensive, regularly updated review of diagnosis and treatment (subscription required) UpToDate
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
