| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Livedo Reticularis ✅
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
🌐 Livedo reticularis is caused by dilatation and stagnation of blood within dermal capillaries and venules, producing a mottled, net-like discoloration of the skin.
📖 About
- Livedo reticularis is a cutaneous vascular pattern characterised by a mottled, reticular (net-like) violaceous discoloration of the skin.
- It may be physiological (benign) or associated with vascular, autoimmune, or thrombotic disease.
- Physiological forms are often triggered by cold exposure and resolve with warming.
- Pathological forms may persist and are sometimes referred to as livedo racemosa.
🩺 Clinical Features
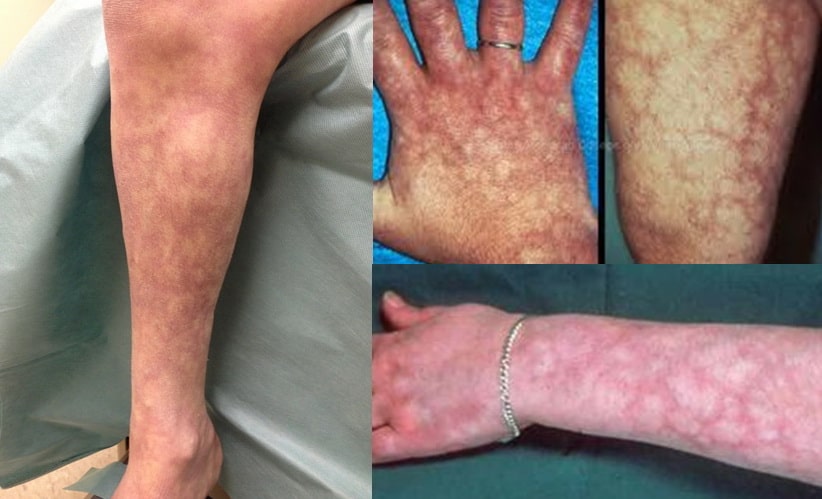
- Mottled blue-red or violaceous reticular pattern on the skin.
- Most commonly affects the legs, thighs, arms, and trunk.
- Physiological livedo typically worsens in cold environments ❄️ and improves with warming.
- Persistent or irregular livedo may indicate underlying vascular or autoimmune disease.
- Associated systemic symptoms may include headache, dizziness, or neurological deficits, particularly in disorders such as Sneddon syndrome.
🧾 Causes
- Physiological: Cold-induced cutis marmorata (common and benign).
- Autoimmune/connective tissue disease: systemic lupus erythematosus, rheumatoid arthritis, dermatomyositis.
- Vasculopathy or vasculitis: polyarteritis nodosa, antiphospholipid syndrome.
- Haematological or thrombotic disorders: hypercoagulable states, cryoglobulinaemia.
- Infective associations: hepatitis C (particularly with cryoglobulinaemia).
- Embolic disease: cholesterol embolisation following vascular procedures.
- Inherited/metabolic: homocystinuria.
- Sneddon syndrome: persistent livedo with cerebrovascular disease and increased stroke risk 🚨.
🔬 Investigations
- Blood tests: FBC, U&E, inflammatory markers, autoimmune screen (ANA, dsDNA), rheumatoid factor.
- Coagulation tests: antiphospholipid antibodies and clotting profile if thrombophilia suspected.
- Infection screening: hepatitis C serology where clinically appropriate.
- Further testing: vascular imaging or biopsy if vasculitis or embolic disease suspected.
💊 Management
- Identify and treat the underlying cause where present.
- Conservative measures: keep warm and avoid vasoconstrictive triggers such as smoking or sympathomimetic drugs.
- Autoimmune disease: immunosuppressive therapy may be required.
- Thrombotic disorders: anticoagulation may be indicated.
- Infective causes: treat underlying infection (e.g., antiviral therapy for hepatitis C).
🧠 Exam Tip
- Antiphospholipid syndrome and Sneddon syndrome are classic associations → think “livedo + stroke risk.”
📚 Guideline & Reference Sources
- NICE Clinical Knowledge Summaries – Antiphospholipid syndrome https://cks.nice.org.uk/topics/antiphospholipid-syndrome/
- British Association of Dermatologists – Vascular skin disorders resources https://www.bad.org.uk/
- British National Formulary – Anticoagulation and immunosuppressive therapy https://bnf.nice.org.uk/
- DermNet NZ Dermatology Reference – Livedo Reticularis https://dermnetnz.org/topics/livedo-reticularis

Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
