| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Developmental Dislocation (Dysplasia) of the Hip (DDH)
Related Subjects: | Developmental Dysplasia of the Hip (DDH) | Slipped Upper Femoral Epiphysis (SUFE) | Perthes Disease (Osteochondritis of the Hip)
👶 Babies swaddled tightly with hips/knees straight have a much higher risk of DDH. ⏰ Early detection is critical → late diagnosis often means major surgery, poorer outcomes, and long-term disability.
📖 About
- Occurs in ~1–2 per 1,000 babies needing treatment.
- A spectrum: from mild acetabular dysplasia → subluxation → frank dislocation.
- Ball (femoral head) is unstable in socket (acetabulum) → may dislocate.
⚙️ Aetiology
- Hip is a ball-and-socket joint but is malformed in DDH.
- Femoral head may be loose, subluxed, or fully dislocated.
- Multifactorial: mechanical (breech), genetic, intrauterine factors.
📌 Risk Factors
- 👧 Female sex, 🍼 first-born child.
- 🤰 Breech delivery (all breech girls need hip USS).
- 👨👩👧 Family history (parents/siblings).
- 💧 Oligohydramnios (reduced amniotic fluid).
🗂️ Classification
- Dislocated: femoral head completely outside socket.
- Dislocatable: head in acetabulum but easily displaced on exam.
- Subluxatable: femoral head loose, moves within socket but not fully dislocated.
🔍 Key neonatal tests: - Ortolani’s test (reduce dislocated hip). - Barlow’s test (provoke dislocation).
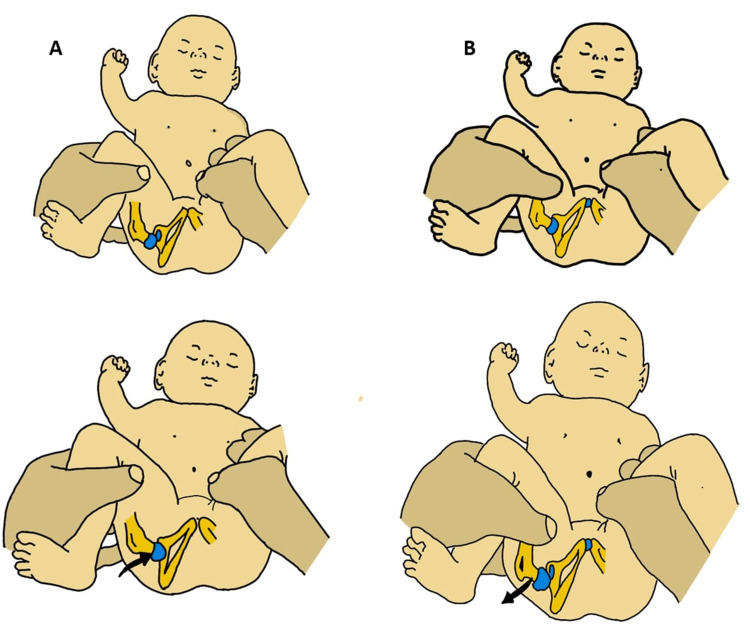
🩺 Clinical Signs (<3 months)
- Asymmetrical skin folds (inguinal, gluteal, thigh).
- Klisic line: from greater trochanter to ASIS → should pass through umbilicus; falls below if DDH.
- Ortolani & Barlow positive → USS indicated.
- USS preferred <6 months (femoral head cartilaginous). X-ray useful >6 months.
🔍 Clinical Presentation
- Routine hip screen: birth + 6–8 weeks.
- Unequal leg length, asymmetric movement, limited abduction.
- Older infants: limp, toe-walking, waddling gait.
🧪 Investigations
- Ultrasound (USS): gold standard <6 months. Detects subtle instability.
- X-ray (>6 months): - Hilgenreiner’s line (through triradiate cartilages). - Perkins line (perpendicular from acetabular edge). - Shenton’s line (should be continuous curve). - Acetabular index: normally 27.5° at birth → 20° by age 2;>30° abnormal.
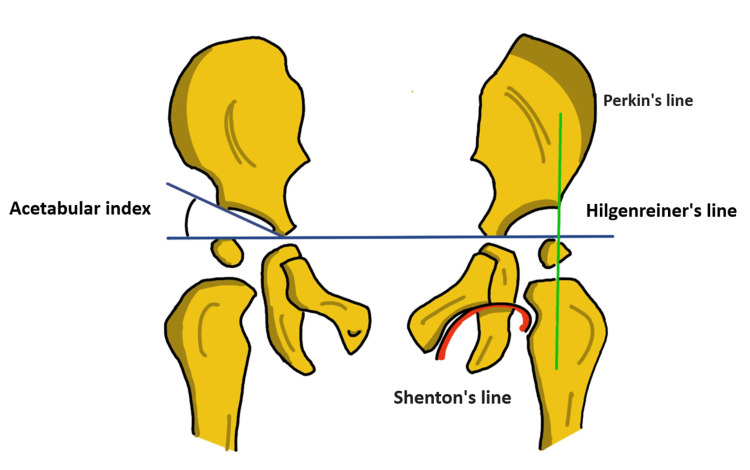
🚨 Complications
- Untreated → early hip OA, chronic pain, gait disturbance.
- Leg length difference, persistent limp, “duck-like” gait.
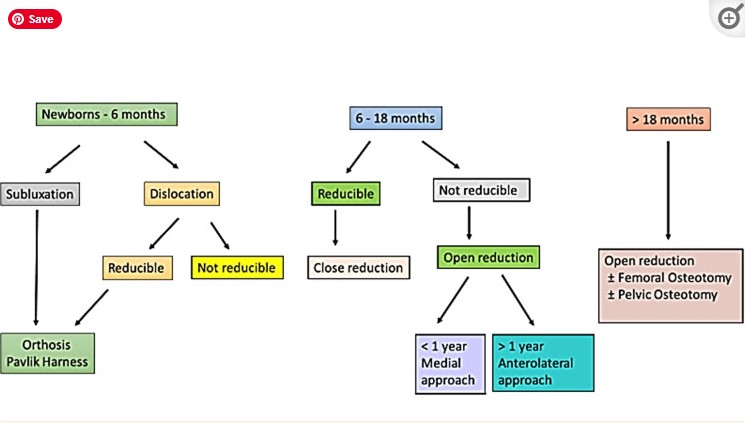
🩹 Management
- 0–6 months: Pavlik harness or brace (keeps femoral head in socket).
- 6–12 months: Harness or brace, sometimes spica casting after reduction.
- 12–24 months: Closed reduction + spica cast. Skin traction sometimes pre-reduction. If fails → open reduction + spica cast.
- >2 years / severe cases: Often require open surgery ± pelvic/femoral osteotomies.
- Even after treatment → socket may remain shallow, may need later corrective surgery.
💡 Teaching Pearls
- Always check hip abduction in newborns. Limited abduction is a red flag. - Breech girls always get a hip USS regardless of exam findings. - Late presentation = much harder to treat and worse outcomes. - “Pavlik harness saves hips” – but only if used early!
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
