| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Ankylosing spondylitis
Related Subjects: |Monoarticular arthritis |Polyarticular arthritis |Seronegative Spondyloarthropathies |Ankylosing spondylitis |Enteropathic Spondyloarthritis |Reactive Arthritis |Psoriatic Arthritis |Adult Onset Still's Disease |Alkaptonuria
🦴 Ankylosing Spondylitis (AS) is a chronic, progressive inflammatory disease of the axial skeleton. It causes loss of lumbar lordosis, ↑ thoracic kyphosis, and sacroiliitis, with systemic extra-articular features. 💡 Classic: young man with back pain + morning stiffness that improves with exercise but not rest! 🏃♂️
ℹ️ About
- Part of the seronegative spondyloarthritides (RF negative, HLA-B27 linked).
- Onset: age 15–40, male:female ≈ 4:1.
- Inflammatory back pain starts in sacroiliac joints → ascends spine.
- Associated with enthesitis, peripheral arthritis, and systemic features.
⚙️ Pathology
- Chronic enthesitis (inflammation where ligaments/tendons attach to bone).
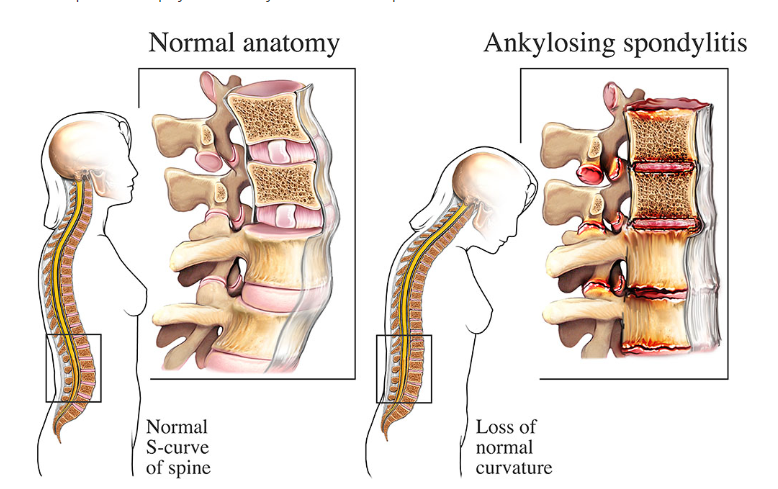
- New bone formation → syndesmophytes → gradual spinal fusion (bamboo spine on X-ray).
- Loss of lumbar lordosis, ↑ thoracic kyphosis, fixed flexion deformity.
- Costovertebral joint involvement → ↓ chest expansion.
🧬 Aetiology
- Strong genetic link: HLA-B27 present in >90% of patients.
- Environmental/infective triggers suggested (e.g. Klebsiella pneumoniae molecular mimicry).
📊 HLA-B27 Association
- Caucasian general population: ~8% carry HLA-B27.
- Ankylosing spondylitis: 90%.
- Reactive arthritis (Reiter’s): 70%.
- Enteropathic arthritis: 50%.
- Psoriatic arthritis: 20%.
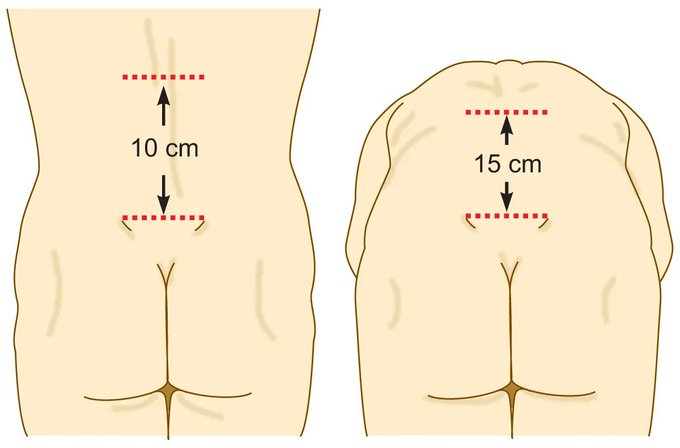
Modified Schober Test
👨⚕️ Clinical – Spinal
- Young male, insidious onset chronic low back pain + morning stiffness >1h.
- Symptoms improve with exercise, not with rest.
- Loss of lumbar lordosis, ↑ thoracic kyphosis → “question-mark posture ❓”.
- Alternating buttock pain (sacroiliitis).
- Spinal rigidity → risk of fractures, cauda equina, cord compression.
🌍 Clinical – Extra-articular
- 👁️ Acute anterior uveitis (red, painful eye, photophobia, blurred vision).
- ❤️ Aortic regurgitation, aortitis, AV block.
- 🫁 Apical pulmonary fibrosis → restrictive lung disease.
- 🦵 Peripheral arthritis (hips, shoulders); enthesitis (Achilles, plantar fascia).
- 🧪 Rare: secondary AA amyloidosis.
📝 Aide-Mémoire – “9 A’s”
- Ankylosis (spinal fusion)
- Anterior uveitis
- Amyloidosis
- Aortic regurgitation / Aortitis
- AV block
- Apical pulmonary fibrosis
- Achilles tendonitis
- Anderson lesion (spinal fracture)
- Anti-TNF therapy (treatment)
📏 Clinical Tests of Spinal Mobility
- Modified Schober Test: lumbar flexion ↑ >3 cm normally.
- Lateral flexion: fingertip–floor distance ↓ >10 cm.
- Chest expansion: normally >3 cm at 4th intercostal space.
- Occiput–wall distance: normally 0 cm.
- Chin–sternum distance: should touch sternum.
- Cervical rotation: >50° normally.
- Intermalleolar distance: reduced if hip involvement.
🔎 Investigations
- Inflammatory markers: ESR, CRP often ↑.
- HLA-B27: supportive but not diagnostic.
- X-ray pelvis: bilateral sacroiliitis, squaring of vertebrae, syndesmophytes → “bamboo spine”.
- MRI sacroiliac joints: detects early inflammation before X-ray changes.
💊 Management
- 🏃 Physiotherapy + exercise: cornerstone of management.
- 💊 NSAIDs (naproxen, indomethacin) first-line for pain/stiffness.
- 🧴 Biologics: anti-TNF (etanercept, adalimumab) or IL-17 inhibitor (secukinumab) if refractory.
- 💊 DMARDs (e.g. sulfasalazine, methotrexate): helpful for peripheral arthritis, not axial disease.
- 🦴 Bisphosphonates if osteoporosis risk.
- 👁️ Treat uveitis promptly with steroids (ophthalmology input).
- 💉 Surgery: joint replacement if severe hip involvement.
📚 Teaching Pearls
💡 Key exam clue = young man + inflammatory back pain that improves with activity. 🔍 Always check for extra-articular features (esp. uveitis, cardiac). ⚠️ Complication to remember = spinal fractures + cauda equina. 🏥 Long-term monitoring: bone density, echo (aortic regurg), chest imaging, ophthalmology.
Cases - Ankylosing Spondylitis (AS)
- Case 1 - Classic young man with back pain 🧍♂️: A 24-year-old man presents with 1 year of progressive low back pain and stiffness, worse in the mornings and improving with activity. Exam: reduced lumbar flexion (positive Schober’s test) and tenderness over sacroiliac joints. X-ray: sacroiliitis. HLA-B27 positive. Diagnosis: ankylosing spondylitis. Managed with exercise and NSAIDs.
- Case 2 - Extra-articular features 👁️: A 32-year-old man with known AS develops acute painful red eye with photophobia. Exam: reduced vision and ciliary injection → acute anterior uveitis. Treated urgently with topical steroids and ophthalmology referral. His AS is escalated to biologic therapy (anti-TNF).
- Case 3 - Advanced disease 🦴: A 45-year-old man presents with progressive spinal stiffness and limited chest expansion. Lateral spine X-ray shows “bamboo spine” from syndesmophyte formation. He also has restrictive lung defect on spirometry. Managed with physiotherapy, biologics, and respiratory support as needed.
Teaching Point 🩺: Ankylosing spondylitis is a seronegative spondyloarthropathy (HLA-B27 associated) with hallmark inflammatory back pain, sacroiliitis, and extra-articular features (uveitis, aortitis, restrictive lung disease). Early physiotherapy and biologics are key to improving outcomes.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
