| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Aortic Dissection ✅
Related Subjects: |Assessing Chest Pain |Acute Coronary Syndrome (ACS) General |Aortic Dissection |Pulmonary Embolism |Acute Pericarditis |Diffuse Oesophageal Spasm |Gastro-oesophageal reflux |Oesophageal Perforation Rupture |Pericardial Effusion Tamponade |Pneumothorax |Tension Pneumothorax |Shingles | Ankle-Brachial pressure Index (ABPI) and Peripheral Vascular Disease | Peripheral Arterial Disease (PAD) | Abdominal Aortic Aneurysm (AAA) | Carotid Endarterectomy | Buerger's disease (Thromboangiitis obliterans ) | Leriche syndrome (aortoiliac occlusive disease)
🚨 Aortic Dissection is a life-threatening emergency caused by a tear in the aortic intima, allowing blood to enter the media and create a false lumen. Early recognition is critical: misdiagnosis as MI ❤️🔥 or PE 🩸 is dangerous, as anticoagulation can worsen outcomes. Urgent imaging and specialist referral are essential.
| 🩺 Management of Acute Aortic Dissection |
|---|
|
📖 Overview
- Mortality: ~40% die before reaching hospital ⚰️; an additional 10% peri/post-op.
- High-risk features: severe sudden chest/back pain, BP differences, syncope, neurologic deficits.
- Types: Stanford A (ascending aorta) and B (descending aorta), guiding management.
- NICE and ESC guidelines emphasise rapid recognition, blood pressure control, imaging, and cardiothoracic referral.
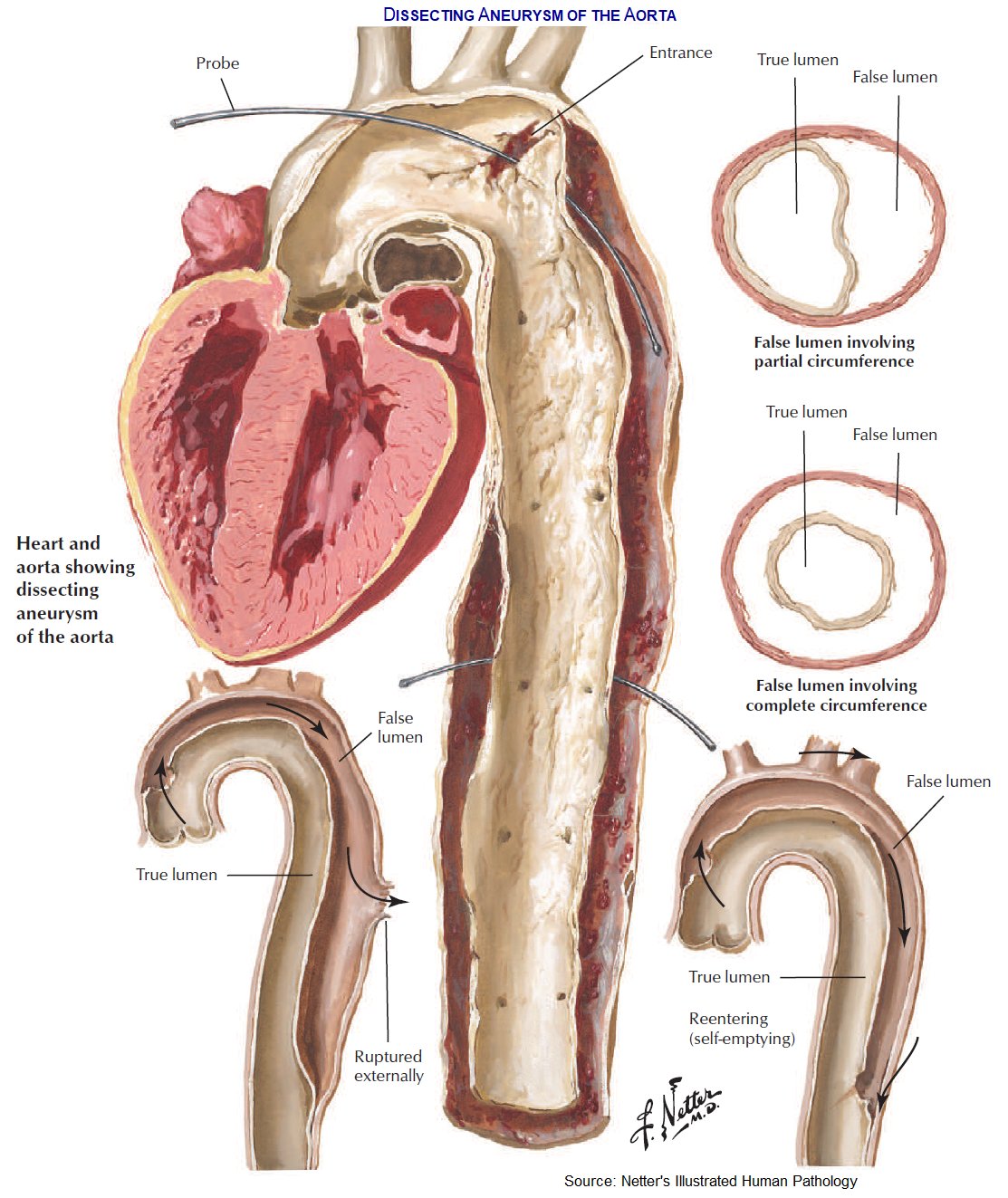
🧬 Pathophysiology
- The aortic wall has three layers: intima, media, adventitia.
- A tear in the intima allows blood under high pressure to dissect into the media → formation of a false lumen.
- Complications: rupture, tamponade, branch vessel obstruction, acute aortic regurgitation, MI, stroke.
- Extension can be antegrade (distal vessels) or retrograde (aortic valve/coronaries).
- Shear stress and hypertension exacerbate propagation; connective tissue disorders weaken the media.
🌍 Epidemiology
- Incidence: ~3–4 per 100,000/year; more common in males ♂, age >60.
- Type A: ~2/3 of cases; Type B: ~1/3.
- Risk factors: chronic hypertension, connective tissue disease (Marfan, Ehlers–Danlos), bicuspid aortic valve, pregnancy (3rd trimester), cocaine, trauma, aortitis.
- Mortality rises 1–2% per hour if Type A dissection is untreated.
🧬 Causes / Risk Factors
| Category | Examples / Details |
|---|---|
| Hypertension | Chronic uncontrolled hypertension in elderly patients; most common predisposing factor |
| Connective tissue disorders | Marfan, Ehlers–Danlos, Loeys–Dietz → medial cystic degeneration |
| Aortitis / Vasculitis | Takayasu arteritis, Giant Cell Arteritis, syphilitic aortitis |
| Congenital / Structural | Bicuspid aortic valve, coarctation, post-surgical aorta repair |
| Trauma / Iatrogenic | Blunt chest trauma, catheterisation, aortic surgery |
| Drugs / Toxins | Cocaine, amphetamines, sympathomimetics (↑ shear stress) |
| Pregnancy / Peripartum | 3rd trimester or early postpartum due to hormonal and haemodynamic changes |
🩺 Clinical Presentation
- Sudden severe chest/back pain: “tearing”, radiates to interscapular area ⚡🖤.
- BP asymmetry between arms >20 mmHg.
- New diastolic murmur of aortic regurgitation.
- Syncope (15%), neurological deficits, limb ischemia, abdominal pain.
- Shock or hypotension → tamponade or rupture.
- Pulsus paradoxus or absent peripheral pulses indicate major compromise.
❗ Complications
- Type A: cardiac tamponade, aortic regurgitation, MI, stroke, rupture, death 💥
- Type B: renal or mesenteric ischemia ⚠️, spinal cord ischemia 🦽, distal limb ischemia, rupture
- Chronic dissection: aneurysm formation, persistent pain, heart failure
🔎 Investigations
- Bloods: FBC, U&E, creatinine, troponin, D-dimer (helps rule out if normal).
- ECG: may mimic MI if coronary involved; usually non-specific.
- CXR: widened mediastinum, pleural effusion.
- Transthoracic echocardiography (TTE): limited, proximal ascending aorta only.
- Transoesophageal echo (TOE): bedside, rapid, sensitive for unstable patients.
- CT Aortogram (spiral CT): gold standard for diagnosis and anatomy delineation 🖥️.
- MRI: useful in chronic cases or if contrast contraindicated.
🩺 Initial Management (Acute Phase)
- ABC: oxygen, IV access, monitor vitals 💨❤️
- Pain control: IV morphine 2.5–5 mg titrated
- Blood pressure & heart rate control: IV beta-blocker (labetalol first-line), target HR ~60 bpm, systolic BP 100–120 mmHg
- Avoid anticoagulants, antiplatelets, and thrombolytics ❌
- Urgent imaging and cardiothoracic referral for Type A dissection
- Type B: medical management if uncomplicated (strict BP control, analgesia, monitoring)
🩺 Definitive Management
| Type | Management |
|---|---|
| Type A (ascending) | Urgent cardiothoracic surgery: repair ± aortic root replacement, graft. Pre-op BP control. ICU post-op care. |
| Type B (descending) | Medical: IV antihypertensives, analgesia. Endovascular stenting (TEVAR) if complications: rupture, malperfusion, persistent pain. |
💊 Pharmacological Management
- IV Beta-blockers: labetalol or esmolol (reduce shear stress, HR)
- Vasodilators: nitroprusside if BP not controlled after beta-blocker
- Analgesia: IV opioids
- Avoid anticoagulation unless otherwise indicated
- Post-op: long-term antihypertensive therapy, surveillance imaging (CTA or MRI at 3, 6, 12 months)
🧪 Monitoring & Follow-up
- Continuous telemetry in acute phase
- Serial imaging: CT or MRI to monitor false lumen, aneurysm formation
- BP & HR targets lifelong: systolic 100–120 mmHg, HR 60–70 bpm
- Patient education: avoid high-intensity isometric exercise
- Genetic counseling if connective tissue disorder suspected
📚 Guidelines & NICE Compliance
- 2014 ESC Guidelines: “Acute aortic syndromes – diagnosis, imaging, and treatment”
- NICE (NG136, NG206): recommend urgent imaging for suspected dissection, avoid anticoagulation until diagnosis, early cardiothoracic referral, BP control, and long-term follow-up
- Conservative vs surgical management based on type, comorbidities, and complications
- Emphasis on structured care: ED recognition, ICU management, MDT review
🧑⚕️ Case Examples
- Case 1 – Type A: 58M, sudden tearing chest/back pain, unequal arm BP. ECG non-diagnostic. CT confirms ascending aorta dissection. Managed with IV labetalol, urgent surgery.
- Case 2 – Type B: 70F, interscapular back pain, hypertensive, no malperfusion. CT confirms descending dissection. Managed medically with IV antihypertensives, analgesia, monitored in ICU. TEVAR reserved for complications.
- Case 3 – Complicated: 65M, Marfan’s, chest pain, syncope, left leg weakness, hypotension. CT: Type A with branch vessel compromise. Emergency surgery + ICU care.
📊 Key Teaching Points
- Always consider dissection in acute chest/back pain, especially if tearing, radiating to back, with BP asymmetry
- Do not give anticoagulants before ruling out dissection
- Type A = surgical emergency; Type B = usually medical
- CT aortogram is gold standard; TOE useful if unstable
- Rapid BP control and pain management reduce mortality
- Follow-up imaging and lifelong BP control are essential to prevent recurrence or aneurysm formation
📚 References
- 2014 ESC Aortic Disease Guidelines
- NICE Guideline NG136: Acute chest pain assessment
- NICE Guideline NG206: Cardiac conditions emergency care
- Hiratzka LF et al., Circulation, 2010; 121: e266–369 – ACC/AHA Guidelines on Thoracic Aortic Disease
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
