| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Pancreatitis ✅
Related Subjects: | Acute Cholecystitis | Acute Appendicitis | Chronic Peritonitis | Abdominal Aortic Aneurysm | Ectopic Pregnancy | Acute Cholangitis | Acute Abdominal Pain | Assessing Abdominal Pain | Penetrating Abdominal Trauma | Acute Pancreatitis | Acute Diverticulitis
🧪 Lipase vs Amylase in Acute Pancreatitis Lipase is the preferred diagnostic enzyme test in suspected acute pancreatitis. It has similar sensitivity but higher specificity than amylase and remains elevated for longer.
- ⏳ Lipase: remains elevated for ~8–14 days
- ⏱️ Amylase: typically normalises within 3–5 days
- 📉 Enzyme level does NOT correlate with disease severity
- 🕒 Lipase is particularly useful in delayed presentation
| ⚡ Initial Management of Acute Pancreatitis |
|---|
|
ℹ️ Overview
- 🔥 Acute pancreatitis is an acute inflammatory condition of the pancreas.
- 🧬 Premature activation of pancreatic enzymes causes autodigestion of pancreatic tissue.
- ⚠️ Severe disease can trigger SIRS, multi-organ failure, and pancreatic necrosis.
- 📈 Incidence is increasing in the UK due to gallstone disease, alcohol use, and metabolic disease.
🎯 Causes (Common UK Causes)
- 🪨 Gallstones – most common cause in the UK
- 🍷 Alcohol
- 📈 Hypertriglyceridaemia
- 🧬 Post-ERCP pancreatitis
- 💊 Drug-induced: azathioprine, valproate, thiazides, steroids, tetracyclines, didanosine
- 🧪 Metabolic: hypercalcaemia (e.g., hyperparathyroidism)
- 🦠 Infections: mumps, CMV, HIV
- 🚑 Trauma
🩺 Diagnosis (Need 2 of 3)
- 🔥 Typical abdominal pain (severe epigastric pain radiating to the back)
- 🧪 Lipase or amylase >3× upper limit of normal
- 🩻 Imaging consistent with pancreatitis
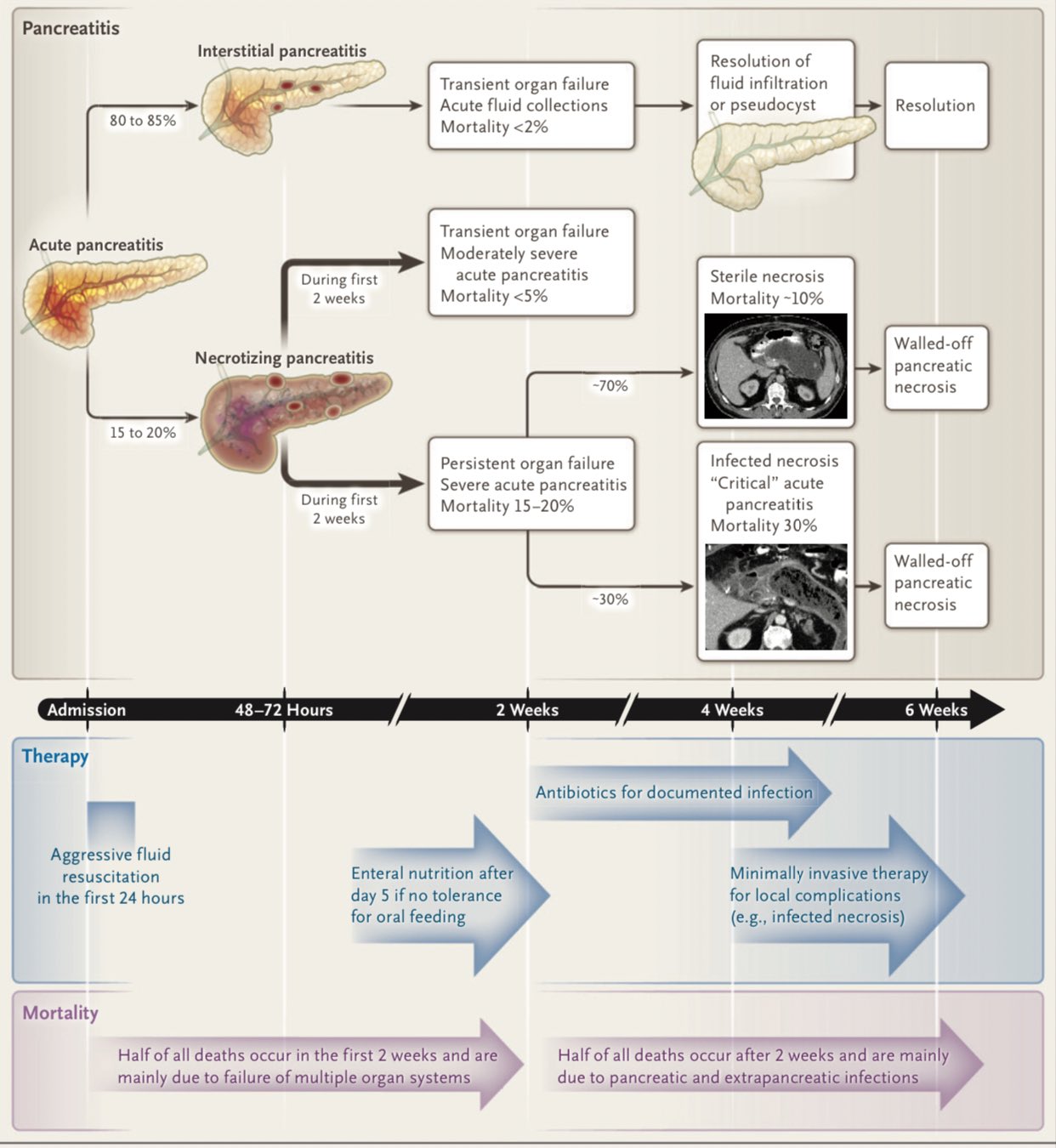
🧬 Pathophysiology
- 🧪 Premature activation of trypsin within pancreatic acinar cells.
- 🔥 Enzyme cascade activates lipase, elastase, and phospholipase.
- ➡️ Leads to fat necrosis, haemorrhage, oedema, and inflammation.
- 🫀 Severe disease triggers SIRS and multi-organ dysfunction.
🩹 Clinical Features
- 🔥 Severe epigastric pain radiating to the back
- 🤢 Nausea and vomiting
- 📉 Tachycardia, hypotension, fever
- ⚠️ Cullen’s sign (periumbilical bruising)
- ⚠️ Grey Turner’s sign (flank bruising)
📊 Severity Assessment
- 📈 CRP >150 mg/L at 48h suggests severe pancreatitis
- 🧮 Glasgow–Imrie score commonly used in UK
- ⚠️ Persistent organ failure >48h defines severe pancreatitis
🔬 Investigations
- 🧪 FBC, U&E, CRP, Ca²⁺, LFTs, glucose
- 🧪 Lipase (preferred) or amylase
- 📈 Triglycerides
- 🩻 Ultrasound within 24 hours to look for gallstones
- 🖥️ CT abdomen if diagnosis uncertain or severe disease suspected (usually after 72h)
- 🔧 ERCP if gallstone pancreatitis with cholangitis or biliary obstruction
⚠️ Complications
- 🫀 Local: necrosis, pseudocyst, abscess
- 🫁 Systemic: ARDS, sepsis, renal failure
- 🧪 Metabolic: hypocalcaemia, hyperglycaemia
- ➡️ Recurrent disease may lead to chronic pancreatitis
- 💧 IV Fluids & Electrolyte Correction: - Start with isotonic crystalloid (e.g., 0.9% saline or Ringer’s lactate) aiming for urine output ≥0.5 mL/kg/h. - Monitor daily: electrolytes, renal function, haematocrit. - Correct hypocalcaemia, hypomagnesaemia, and hypokalaemia promptly.
- 💊 Pain Control: - Opioids are first-line (e.g., morphine or oxycodone). - Avoid NSAIDs if renal impairment or coagulopathy. - Consider PCA for severe pain or ICU setting.
- 🥤 Nutrition: - Early enteral feeding (via NG or NJ tube) within 24–48 hours is preferred to parenteral nutrition. - Reduces infectious complications and supports gut mucosal integrity. - Oral diet resumed once tolerated (low-fat diet initially). - Parenteral nutrition only if enteral feeding not possible.
- 🚫 Antibiotics: - Not used prophylactically. - Only indicated if infected necrosis is suspected (clinical deterioration, sepsis, imaging with gas in necrotic areas). - Choice guided by microbiology; usually broad-spectrum covering Gram-negative and anaerobes (e.g., meropenem or piperacillin-tazobactam).
- 🔧 ERCP (Endoscopic Retrograde Cholangiopancreatography): - Urgent (<24 hrs) if gallstone pancreatitis with cholangitis (Charcot’s triad: fever, jaundice, RUQ pain). - Not indicated in mild pancreatitis without cholangitis.
- 🔪 Cholecystectomy: - Interval cholecystectomy recommended during same admission for gallstone pancreatitis once acute inflammation settles. - Reduces risk of recurrence.
- 🏥 HDU/ICU Care: - Required for patients with organ failure (renal, respiratory, cardiovascular). - Monitor for systemic complications: SIRS, ARDS, shock, acute kidney injury. - Consider invasive monitoring (arterial line, central venous line) if severe.
- 🧬 Monitoring & Investigations: - Daily clinical review, vitals, fluid balance. - Repeat labs: amylase/lipase trending, CBC, LFTs, renal panel, CRP (rising CRP can indicate necrosis). - Imaging (CT with contrast) reserved for patients not improving by 72 hrs or suspicion of complications (necrosis, abscess, pseudocyst).
- ⚠️ Supportive Measures: - Thromboprophylaxis (LMWH) if not contraindicated. - Oxygen supplementation for hypoxaemia. - Glycaemic control (hyperglycaemia common due to stress and pancreatic injury).
🩺 Case 1 – Gallstone Pancreatitis
A 52-year-old woman presents with sudden severe epigastric pain radiating to the back. Lipase is markedly elevated and ultrasound shows gallstones. Management: 💧 IV fluids, analgesia, monitoring. ⚙️ Perform ERCP if cholangitis or obstruction. 🔪 Definitive treatment = laparoscopic cholecystectomy during same admission. Key learning: Early cholecystectomy reduces recurrence.
🩺 Case 2 – Alcohol-Related Pancreatitis with Pseudocyst
A 45-year-old man with alcohol dependence develops persistent abdominal fullness 4 weeks after pancreatitis. CT shows a 6 cm pseudocyst. Management: If symptomatic or large → endoscopic drainage. Important principle: ⏳ Wait ≥4 weeks for the pseudocyst wall to mature before intervention.
🩺 Case 3 – Severe Necrotising Pancreatitis
A 63-year-old patient develops hypotension, hypoxia, and rising CRP. CT confirms necrotising pancreatitis. Management:
- 🚑 HDU/ICU admission
- 💧 Aggressive fluid resuscitation
- 🫁 Respiratory support
- 🥤 Enteral nutrition
- 🦠 Antibiotics only if infected necrosis
- 🔧 Radiological or surgical debridement if infection confirmed
📚 References – Acute Pancreatitis
- NICE NG104: Acute pancreatitis (2018) – Diagnosis and management
- British Society of Gastroenterology (BSG) Guidelines: Management of Acute Pancreatitis
- Royal College of Paediatrics and Child Health – Acute Pancreatitis Guidance
- Tenner S, Baillie J, DeWitt J, Vege SS. “American College of Gastroenterology guideline: management of acute pancreatitis.” Am J Gastroenterol. 2013;108(9):1400–1415.
- Forsmark CE, Baillie J. “A review of acute pancreatitis.” JAMA. 2007;298(20):2381–2391.
- NICE Guideline NG187: Nutrition support in adults – Enteral vs parenteral feeding recommendations
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
