| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Putaminal Haemorrhage
Related Subjects: |Subarachnoid Haemorrhage |Perimesencephalic Subarachnoid haemorrhage |Haemorrhagic stroke |Cerebellar Haemorrhage |Putaminal Haemorrhage |Thalamic Haemorrhage |ICH Classification and Severity Scores
🧠 Putaminal Haemorrhage is a common form of deep primary intracerebral haemorrhage, usually related to long-standing hypertension. It occurs within the putamen (part of the basal ganglia), which is central to motor control. Accounts for ~30–40% of all ICH cases and carries significant morbidity and mortality.
📊 Epidemiology
- Incidence: 30–40% of intracerebral haemorrhages.
- Age: Predominantly >60 years.
- Sex: More common in males.
- Geography: Higher prevalence in Asian populations.
🧬 Pathophysiology
- Rupture of deep penetrating arteries (lenticulostriates) due to chronic hypertension.
- Expanding clot raises ICP and compresses adjacent structures.
- Damage to the internal capsule → profound motor and sensory deficits.
⚠️ Causes
- Chronic hypertension (most common)
- Cerebral amyloid angiopathy (elderly)
- Anticoagulation / coagulopathy
- Brain tumours or metastases
- Substance misuse (esp. cocaine, amphetamines)
- Vascular malformations (rare)
🧾 Clinical Correlation with Location
- Anterior putamen:
- Left: aphasia, abulia, contralateral weakness.
- Right: behavioural changes, poor insight, aggression.
- Mid-putamen:
- Compression of adjacent structures.
- Left: global aphasia.
- Right: neglect syndrome.
- Posterior putamen: contralateral hemianopia, sensory loss, limb ataxia.
- Medial bleeds: risk of rupture into ventricles → hydrocephalus, coma.
🩺 Clinical Presentation
- Sudden severe headache, nausea, vomiting.
- Focal neurological deficits (motor/sensory loss, speech disturbance).
- Altered consciousness → coma in severe cases.
- Raised ICP signs: papilloedema, bradycardia, hypertension, irregular breathing (Cushing’s triad).
⚠️ Complications
- Expansion of bleed → brainstem compression, herniation.
- Obstructive hydrocephalus.
- Seizures.
- Infection risk with CSF drains.
- Long-term disability (motor + cognitive).
🔬 Investigations
- CT head (non-contrast): first-line to identify bleed size, site, ventricular extension.
- MRI: for underlying lesions or delayed imaging.
- CTA / DSA: if vascular malformation suspected.
- Bloods: FBC, coagulation, U&E.
- ECG: monitor for arrhythmias due to raised ICP/stress.
💊 Management
- Stabilisation: ABCs, BP control (target SBP <140 mmHg).
- Reverse anticoagulation: e.g. Octaplex / Beriplex for warfarin.
- Medical therapy: antihypertensives, ICP control (mannitol, hypertonic saline), anticonvulsants if seizures.
- Surgery:
- Ventriculostomy for hydrocephalus.
- Clot evacuation in selected cases.
- Rehabilitation: MDT input – physio, OT, speech therapy, neuropsychology.
📈 Prognosis
- Mortality: high with large bleeds or intraventricular extension.
- Outcome depends on bleed size, GCS at presentation, and comorbidities.
- Survivors often left with significant neurological disability.
🛡️ Prevention
- Strict hypertension control (lifestyle + medication).
- Avoid unnecessary anticoagulation in high-risk patients.
- Substance misuse counselling.
- Regular follow-up for vascular risk factors.
🧪 Recent Advances
- Minimally invasive clot evacuation techniques (MIS, stereotactic aspiration).
- Neuroprotective agents in clinical trials.
- Advanced CT/MRI for prognostication and surgical planning.
📑 Clinical Guidelines
- Target systolic BP <140 mmHg (AHA/ESO guidelines).
- Immediate anticoagulant reversal if on warfarin/DOACs.
- Seizure prophylaxis considered if cortical involvement.
📚 References
- Hemphill JC et al. (2015). Guidelines for management of spontaneous ICH. Stroke.
- Broderick JP et al. (1993). Baseline NIHSS predicts outcome after ICH. Stroke.
🔗 Additional Resources
🖼️ Images
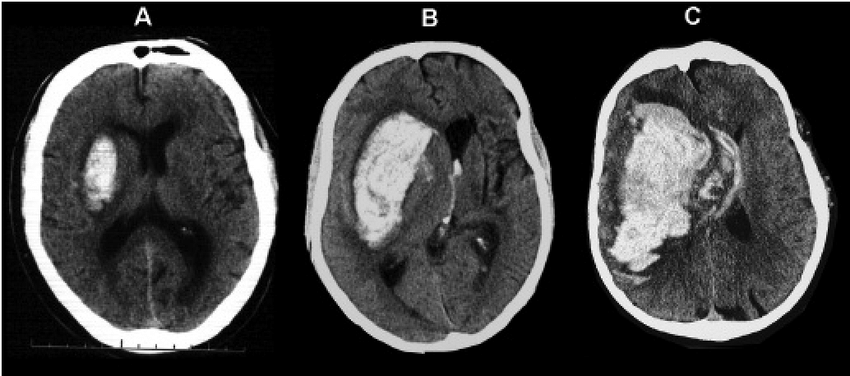 Figure 1: Anatomy of the putamen within the basal ganglia.
Figure 1: Anatomy of the putamen within the basal ganglia.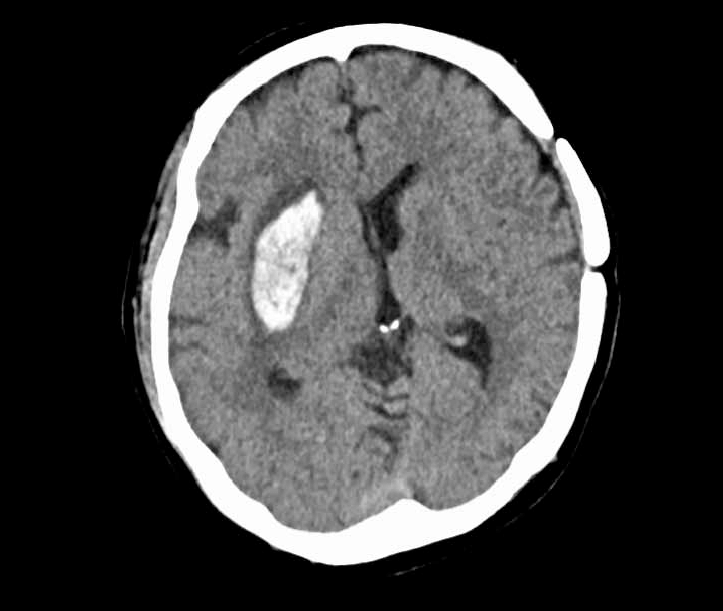 Figure 2: Common haemorrhage sites within the putamen.
Figure 2: Common haemorrhage sites within the putamen.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
