| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Pyoderma gangrenosum ✅
Related Subjects: |Cellulitis |Impetigo |Pyoderma gangrenosum |Pemphigus Vulgaris |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Necrotising fasciitis |Gas Gangrene (Clostridium perfringens) |Anatomy of Skin |Skin Pathology and lesions |Skin and soft tissue and bone infections |Lymphangitis
💥 Always consider Pyoderma Gangrenosum (PG) when assessing ulcerated skin lesions. PG is a rare, non-infectious, inflammatory neutrophilic dermatosis characterized by painful ulcers. It is often associated with systemic diseases like IBD, rheumatoid arthritis, and haematologic disorders.
ℹ️ About Pyoderma Gangrenosum
- ⚠️ Often mistaken for common ulcers - always think beyond “just venous ulcers.”
- 👩⚕️ Consider differential diagnoses including skin cancers, atypical infections, and vasculitis.
- 🧪 Urgent referral to dermatology if suspected; consider biopsy to exclude other causes.
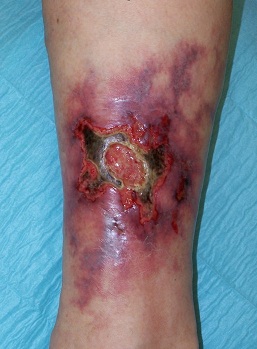
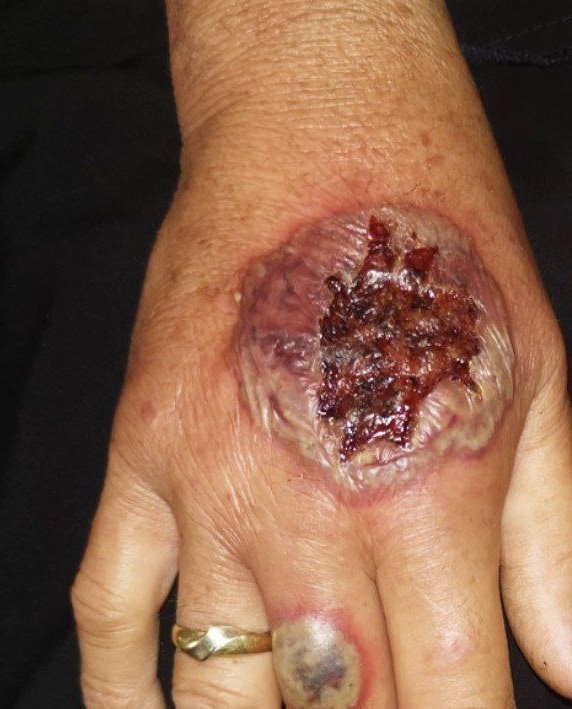
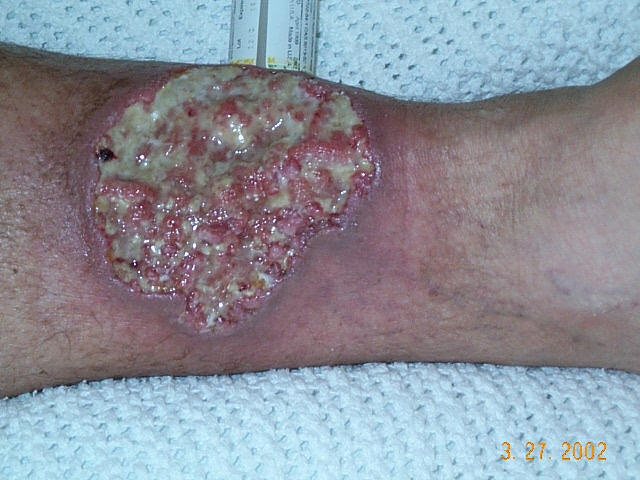
🩺 Clinical Features
- 🔥 Pain: Severe pain, often disproportionate to appearance.
- 🟣 Edges: Undermined, violaceous/blue borders.
- ⚫ Base: Necrotic with purulent/granulomatous tissue.
- 📏 Size: May start small → rapidly expanding ulcers.
- 📍 Sites: Lower legs, surgical wounds, stomas (pathergy phenomenon).
- 🔄 Onset: Often begins as papules, pustules, or vesicles → ulcerates.
- 💥 Trigger: Minor trauma (pathergy) can precipitate.
- 🔗 Associated Diseases: RA, UC, Crohn’s, myeloma, haematologic malignancy.
- 💊 Drugs: Rarely hydroxyurea, GM-CSF.
🧬 Causes and Associations
- ❓ Idiopathic (~20–50%).
- 🧻 IBD: Crohn’s, ulcerative colitis.
- 🩸 Haematologic: Lymphoma, leukaemia, myeloma, myeloproliferative disease.
- 🛡️ Autoimmune: RA, primary biliary cirrhosis.
- 🦠 Other: Hepatitis, HIV, monoclonal gammopathies.
🔍 Investigations
- 📊 FBC, ESR, CRP (raised inflammatory markers).
- 🔬 Skin biopsy (from ulcer edge) → neutrophilic dermatosis (helps exclude other causes but not pathognomonic).
- 🧫 Exclude infection (cultures, swabs).
- 📋 Screen for underlying systemic disease (IBD, RA, haematology referral as needed).
🩹 Management
- 🚫 Avoid trauma: Surgery/skin grafting/debridement can worsen due to pathergy.
- 💊 Topical therapy: Potent/super-potent corticosteroids (e.g., clobetasol), tacrolimus ointment.
- 💊 Pain relief: Analgesia is essential (often very painful ulcers).
- 🩼 Wound care: Non-adhesive dressings, prevent secondary infection.
💉 Systemic Treatments
- 🌟 Corticosteroids: First-line for moderate–severe disease (high-dose oral prednisolone initially).
- 💊 Immunosuppressants: Ciclosporin, methotrexate, dapsone, tetracyclines (e.g., minocycline; steroid-sparing).
- 🧬 Biologics: TNF-α inhibitors (infliximab, adalimumab) - effective esp. in IBD-related/refractory PG.
- 🦠 Antibiotics: Only if secondary infection present (not primary therapy).
🚨 Key Teaching Point: PG is a neutrophilic dermatosis, not an infection. Surgical debridement often makes it worse (pathergy). Always treat underlying systemic disease. Urgent dermatology referral is recommended for suspected cases.
🩺 Case 1 - Associated with Inflammatory Bowel Disease
A 32-year-old woman with ulcerative colitis develops a rapidly enlarging, extremely painful ulcer on her left shin. The lesion has a violaceous undermined edge and a purulent base. She has no signs of cellulitis. Management: 💊 High-dose corticosteroids or ciclosporin; optimise underlying IBD therapy. Wound care and pain relief are essential. Avoid: ❌ Surgical debridement (pathergy phenomenon can worsen lesions); avoid unnecessary antibiotics unless secondary infection is proven.
🩺 Case 2 - Pyoderma Gangrenosum with Rheumatoid Arthritis
A 60-year-old man with long-standing rheumatoid arthritis presents with an ulcer on his right calf, which started as a pustule and progressed to a painful necrotic ulcer with bluish borders. Blood cultures are negative. Management: 🩺 Systemic immunosuppression (steroids, ciclosporin, biologics such as TNF-α inhibitors in refractory cases). Multidisciplinary approach with dermatology and rheumatology input. Avoid: ❌ Mistaking for infective cellulitis and performing repeated surgical interventions; avoid stopping essential RA medications without rheumatology advice.
📚 Key References (as of March 2026)
- British Association of Dermatologists (BAD) Patient Information Leaflet: Pyoderma gangrenosum (updated October 2025).
- Primary Care Dermatology Society (PCDS) Clinical Guidance: Pyoderma gangrenosum (updated February 2026).
- George C et al. Pyoderma gangrenosum – a guide to diagnosis and management. Clin Med (Lond). 2019 (widely referenced in UK practice).
- Recent surveys/meta-analyses confirm steroids/ciclosporin first-line; biologics in refractory/IBD-linked (e.g., UKDCTN prescribing survey 2024; systematic reviews 2025).
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
