| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Bleeding Antepartum
⚠️ Antepartum haemorrhage (APH) = vaginal bleeding after 24 weeks until delivery. Occurs in ~3–5% of pregnancies and is a major cause of maternal & perinatal morbidity/mortality. 💡 Uterine blood flow at term is 600–800 mL/min → even short delays can be catastrophic.
📊 Incidence
- 3–5% of pregnancies.
- Still one of the leading causes of maternal and fetal death worldwide.
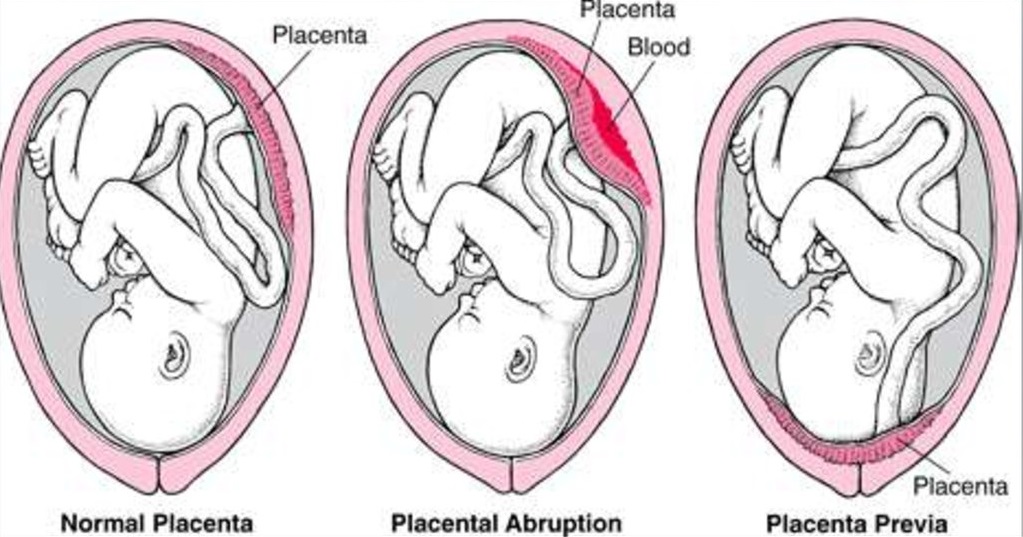
🔎 Causes of APH
- 🌸 Placenta praevia (~1:200 pregnancies) – Painless bright red bleeding. – Placenta partially/completely covers os. – Diagnosed by TVS (transvaginal safest). – ⚠️ Never do PV exam before praevia excluded.
- 💥 Placental abruption – Premature detachment of placenta. – Painful, tense (“woody”) uterus, bleeding (revealed or concealed). – RFs: pre-eclampsia, smoking, cocaine, trauma. – Complications: DIC, fetal compromise, renal failure.
- 🚨 Vasa praevia (~1:2500) – Fetal vessels cross near os → rupture after ROM. – Presents with PV bleed + fetal HR decelerations. – Dx: USS with Doppler. – ⚡ Emergency C-section needed.
- 🧩 Other: circumvallate placenta, cervicitis, cervical polyps, malignancy.
- ❓ Unexplained: ~50% have no identifiable cause but still ↑ perinatal risk.
🩺 Clinical Features
- Praevia: painless, soft uterus, normal FHR.
- Abruption: painful, tense uterus, abnormal FHR.
- Vasa praevia: bleeding + fetal HR changes after ROM.
- Maternal obs, fetal movements, CTG essential.
- ⚠️ Avoid PV exam until praevia excluded on scan.
📏 Severity of Bleed
- Spotting → minor (<50 mL, settled).
- Major → 500–1000 mL, stable.
- Massive → >1000 mL ± maternal shock.
🧪 Investigations
- 🩸 Bloods: FBC, group & save / X-match ≥4 units, clotting, U&E, LFTs.
- 💉 Kleihauer test if Rh− → guides anti-D.
- 🧪 Urinalysis: check proteinuria (pre-eclampsia).
- 📊 CTG: assess fetal wellbeing.
- 🧲 USS: TVS for placental localisation, Doppler for vasa praevia.
🏥 Management
- 🚑 Resuscitation (ABC): O₂, 2x wide-bore IVs, fluids, blood products (O-neg if urgent).
- 📞 Call senior help: obstetrician, anaesthetist, neonatology team.
- 💊 Steroids: 24–34+6 wks if preterm delivery likely.
- 🚺 Placenta praevia: elective C-section if placenta <2 cm from os.
- 💥 Abruption: manage shock (concealed bleed often > visible loss), correct DIC, expedite delivery if unstable.
- ⚡ Massive haemorrhage: Activate major obstetric haemorrhage protocol → immediate delivery (often C-section).
- ➕ Don’t forget: anti-D for Rh−, catheter for fluid balance, monitor urine output.
⚠️ Maternal Complications
- Anaemia, hypovolaemic shock.
- DIC, renal failure (ATN).
- PPH (~25% after abruption).
- Infection, Sheehan’s syndrome, transfusion risks.
⚠️ Fetal Complications
- Hypoxia, IUFD.
- Prematurity, growth restriction.
📌 Exam Pearls
- Praevia = painless + normal FHR.
- Abruption = painful + abnormal FHR.
- Vasa praevia = bleed + FHR drop post-ROM.
- Shock may be concealed → treat aggressively.
- Always ask: maternal stability? fetal compromise? → delivery timing depends on both.
📖 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
