| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Heart Block
Related Subjects: |Resus:Bradycardia |Resus:Tachycardia | Syncope | Transient Loss of Consciousness | Aortic Stenosis | Breast Cancer
⚡ Severe Bradycardia - Management (UK ALS)
| Step | What you do (OSCE/ALS wording) | Key notes / triggers |
|---|---|---|
| 1) Recognise severity | 🔍 Confirm bradycardia on monitor/ECG, check pulse + BP, assess symptoms. | 🚨 Treat as unstable if any adverse features: shock, syncope, MI/ischaemia, acute HF. |
| 2) Call for help + monitor | 📞 Call resus team/senior help, attach defib/pacing pads, continuous ECG + SpO2 + NIBP. | Have pacing ready early if high-grade AV block suspected. |
| 3) ABCDE + access | 🫁 ABCDE, oxygen only if hypoxic, 2 IV cannulas, take bloods (U&E, Mg, glucose, VBG/ABG if unwell). | Look for reversible causes: drug toxicity (β-blocker, digoxin, CCB), hyperkalaemia, hypoxia, MI. |
| 4) ECG | 📈 Get a 12-lead ECG (rhythm + PR/QRS, ischaemia, AV block). | High-risk ECG: Mobitz II, complete heart block, broad QRS escape, long pauses. |
| 5) First-line drug | 💉 Atropine 500 micrograms IV; repeat as needed to max 3 mg. | Less effective in infra-His block; avoid/seek specialist advice in transplanted heart. |
| 6) If no response / unstable | ⚡ Start transcutaneous pacing (with analgesia/sedation support) while preparing for definitive pacing. | Don’t delay pacing if high-grade AV block or recurrent syncope/shock. |
| 7) If pacing not available / bridging | 💧 Start an infusion per local protocol: adrenaline 2–10 micrograms/min OR isoprenaline 5 micrograms/min OR dopamine. | Use as a bridge to pacing; monitor for tachyarrhythmia/ischaemia. |
| 8) Definitive management | 🧑⚕️ Arrange temporary transvenous pacing ± permanent pacemaker; treat cause (MI pathway, stop culprit drugs, treat hyperkalaemia). | Complete heart block / Mobitz II usually needs pacing; document decisions + escalation. |
⚡ Heart block (AV block) describes delayed or failed conduction from atria → ventricles. A slow heart rate - cunt QRS complexes can lead to low blood pressure and even shock. This may need emergent treatment. Exam focus: recognise the ECG pattern, assess stability, correct reversible causes, and escalate early for pacing when needed.
🧠 What “heart block” actually means
- 🔌 The AV node–His–Purkinje system is the only normal electrical bridge from atria to ventricles.
- ⛔ “Block” can be partial (delay or intermittent failure) or complete (no impulses conducted).
- 🫀 When ventricles don’t receive atrial impulses, they rely on an escape rhythm:
- ⬆️ Higher (junctional) escape → faster rate, usually narrow QRS.
- ⬇️ Lower (ventricular) escape → slower rate, usually wide QRS.
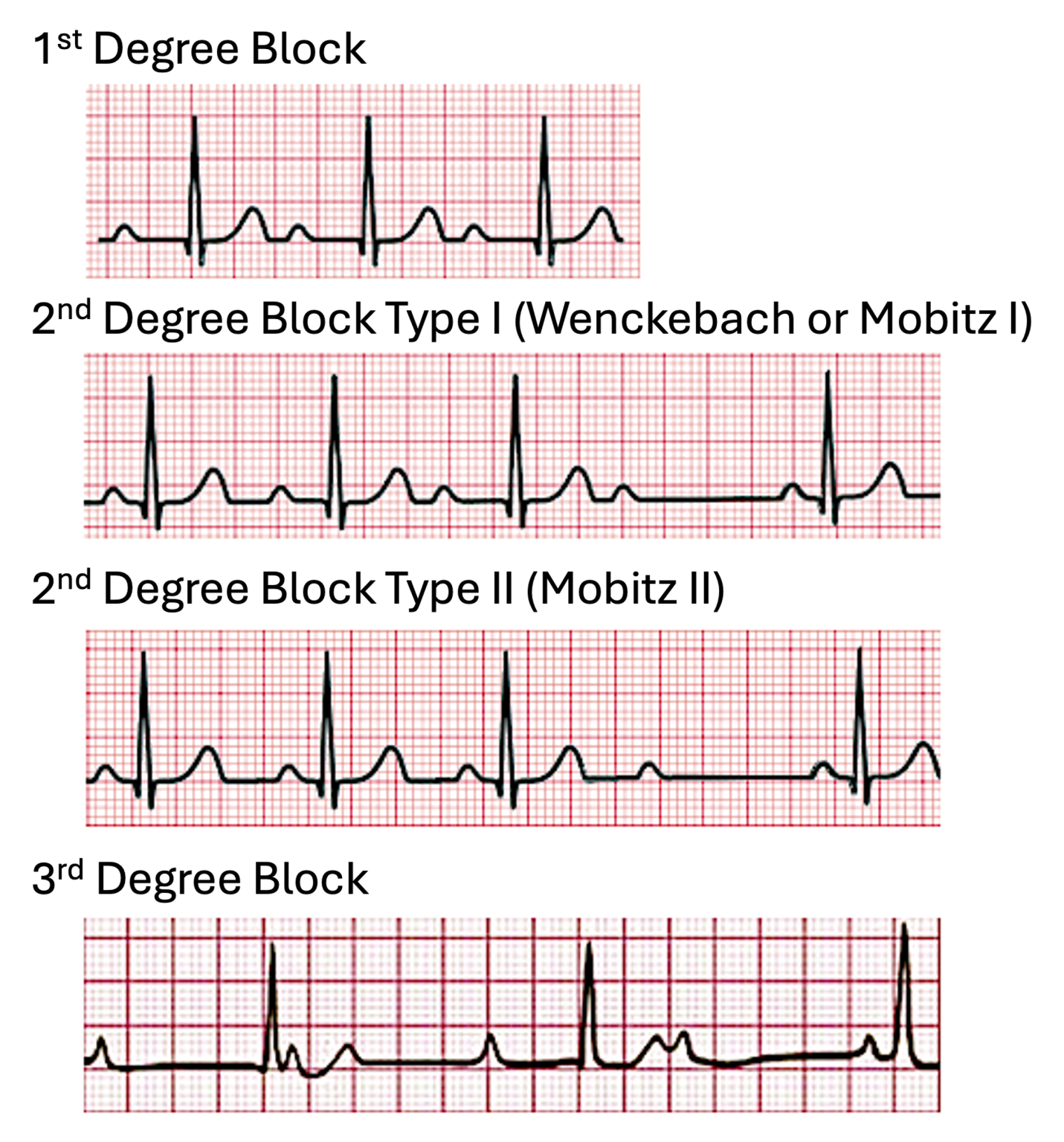
📊 First vs Second vs Third Degree AV Block (high-yield comparison)
| Type | ECG hallmark | What you do (exam / ward) |
|---|---|---|
| 1️⃣ First-degree AV block | PR > 200 ms, constant; every P followed by QRS | Usually observe ✅; review AV-nodal drugs; check U&E (K+/Mg), TFTs; treat underlying cause |
| 2️⃣a 🔁 Mobitz I (Wenckebach) | Progressive PR prolongation → then dropped QRS | If stable: remove triggers/hold AV-nodal drugs, observe; if symptomatic/unstable: manage bradycardia + senior/cardiology review |
| 2️⃣b ⚠️ Mobitz II | Fixed PR with intermittent dropped QRS (often wide QRS) | High-risk 🚨: urgent cardiology; prepare for pacing (often pacing-likely even if transient); treat instability per ALS (pacing preferred) |
| 3️⃣ 🚑 Third-degree (complete) heart block | AV dissociation: P waves and QRS regular but independent; escape rhythm (narrow if high, wide if low) | Time-critical: ABCDE, stop causative drugs, treat reversible causes; atropine may help if nodal; isoprenaline/temporary pacing if needed → usually permanent pacemaker |
🚨 Red flags that should make you escalate immediately
- 🧠 Syncope, recurrent presyncope, confusion
- 🫀 Hypotension, shock, chest pain, acute heart failure, ischaemic ECG changes
- 🧍 Very slow ventricular rate (especially < 40 bpm) or broad-complex escape rhythm
- ⚡ Mobitz II, high-grade AV block (multiple consecutive dropped beats), or complete heart block
🧩 Causes of AV block (exam-friendly table)
| Category | Examples | Clues |
|---|---|---|
| ❤️ Ischaemia / MI | Inferior MI (RCA → AV nodal branch), anterior MI (His–Purkinje damage) | Inferior MI block may respond to atropine and can be transient; anterior MI block is often extensive disease and higher risk. |
| 💊 Drugs | β-blockers, verapamil/diltiazem, digoxin, amiodarone (and other antiarrhythmics) | Recent dose change, renal impairment (digoxin), bradycardia + hypotension. |
| 🧓 Degenerative conduction disease | Fibrosis/sclerosis of the conduction system (age-related) | Older patient, bundle branch block, progressive conduction delay. |
| 🦠 Infective / inflammatory | Myocarditis, endocarditis (peri-annular abscess), Lyme disease, diphtheria | Fever, raised inflammatory markers, new murmur, travel/tick exposure. |
| 🧬 Infiltrative / metabolic | Sarcoid, amyloid, haemochromatosis; hyperkalaemia; hypothyroidism | Systemic features; abnormal K+ / thyroid; unexplained conduction disease. |
| 🛠️ Post-procedure | TAVI, valve surgery, septal myectomy, ablation | New conduction delay after intervention. |
🔎 Investigations (what to send in real life + OSCE)
- 📈 12-lead ECG + rhythm strip (confirm type of block; look for ischaemia).
- 🩺 Obs + perfusion: BP, mental status, cap refill; signs of heart failure.
- 🧪 Bloods: U&E (K+), Mg, Ca, glucose, FBC, CRP, TFTs; troponin if ACS suspected; digoxin level if relevant.
- 🖥️ Echocardiography if structural disease/MI suspected or ongoing instability.
- 🧷 Consider continuous monitoring / telemetry and cardiology review for unexplained or high-grade block.
⚡ Acute management of bradycardia due to AV block (UK ALS-style)
🚑 If unstable: treat as a peri-arrest bradycardia. Start with ABCDE + attach monitoring, then correct reversible causes while preparing for pacing.
| Step | What you do | Why |
|---|---|---|
| 1️⃣ Call for help | 📞 Senior + cardiology; if peri-arrest, resus team/ALS response. | High-grade AV block can deteriorate rapidly. |
| 2️⃣ Stabilise | 🫁 Oxygen if hypoxic, IV access, fluids if shocked, treat pain, correct electrolytes. | Improve perfusion while definitive therapy is arranged. |
| 3️⃣ Atropine (if appropriate) | 💉 Atropine 500 micrograms IV, repeat to a maximum of 3 mg if needed. | May improve AV nodal block (often helpful in inferior MI / nodal disease). |
| 4️⃣ If atropine fails / high-risk block | ⚡ Prepare transcutaneous pacing early; consider isoprenaline infusion as a bridge if pacing not immediately available (specialist / local protocol). | In infranodal block, atropine may be ineffective; pacing prevents collapse. |
| 5️⃣ Definitive treatment | 🧷 Temporary pacing (wire) if needed → usually permanent pacemaker for persistent high-grade/complete AV block. | Prevents recurrence and improves long-term safety. |
🧠 Teaching pearls (sounds clever in vivas)
- 🧬 Nodal vs infranodal block: nodal block is more likely to respond to atropine and has a narrow QRS; infranodal block is more dangerous and often needs pacing.
- 🫀 Why syncope happens: slow escape rhythms reduce cardiac output → cerebral hypoperfusion (Stokes–Adams attacks).
- 🧯 Reversible causes matter: hyperkalaemia, AV nodal drugs, and ischaemia are the “big three” to look for quickly.
⛔ Complete (Third-degree) Heart Block - exam-ready
🚨 Complete heart block can be a medical emergency requiring atropine and pacing. It is defined by complete failure of conduction between atria and ventricles, so the ventricles rely on an escape rhythm.
ℹ️ About
- 🔌 There is a complete failure of communication between atria and ventricles.
- 💓 Atria depolarise regularly (P waves), but do not stimulate the ventricles.
- 🫀 Ventricles beat at an intrinsic escape rate, often ~30–40 bpm if ventricular, faster if junctional.
- 📏 The higher the escape rhythm (closer to AV node), the faster the rate and the narrower the QRS.
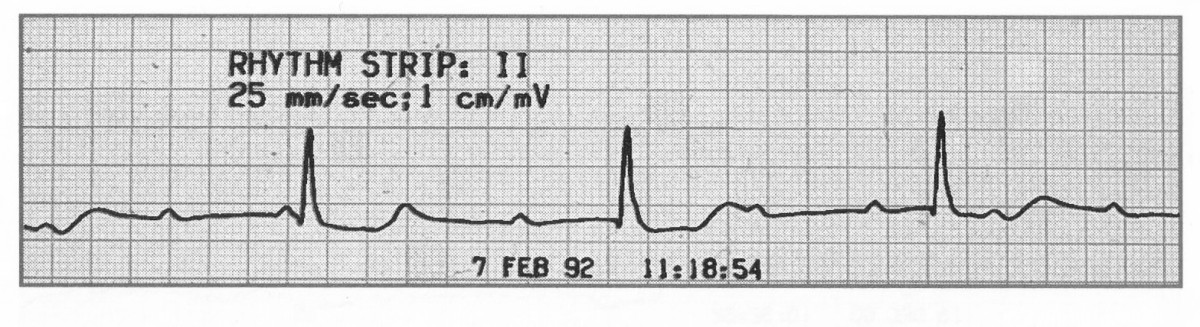
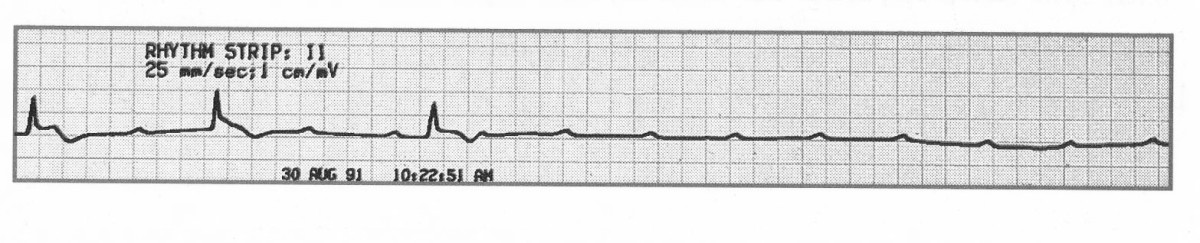
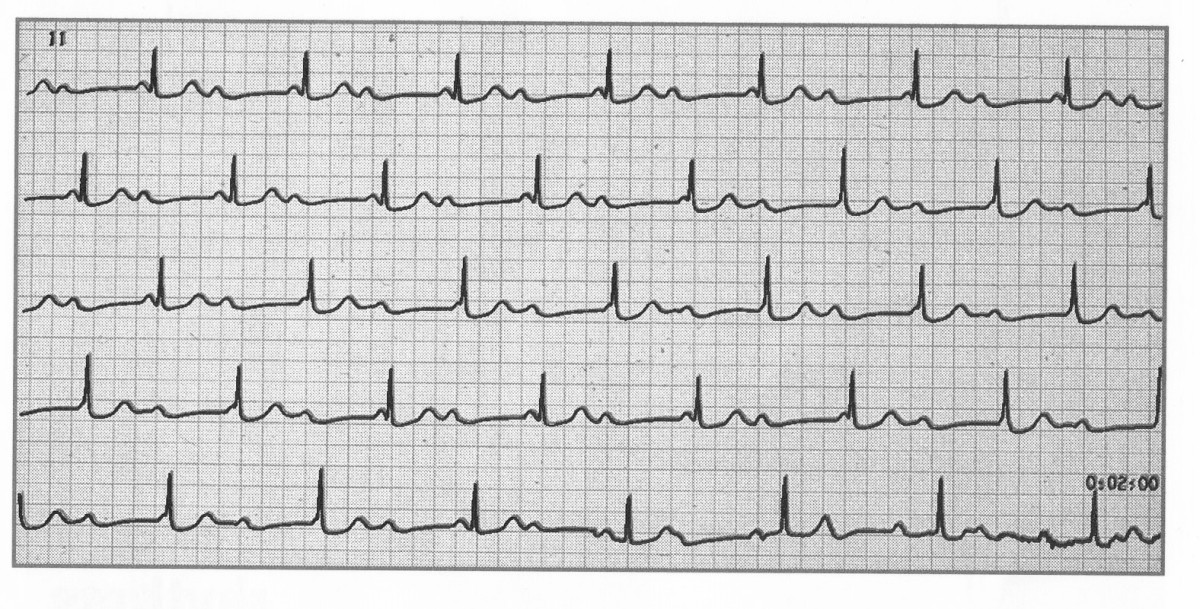
📈 ECG features
- Atrial rate: typically 60–100/min (sinus), independent of the ventricular rhythm (“dissociation”).
- Ventricular rate: depends on escape focus:
- 🐢 Ventricular escape typically ~20–40/min (often wide QRS).
- ⚡ Junctional escape typically ~40–60/min (often narrow QRS).
- Rhythm: atrial and ventricular rhythms are each regular but independent.
- PR interval: no fixed PR relationship (by definition).
- P waves: usually normal morphology (unless AF/atrial flutter etc.).
- QRS: narrow suggests higher escape; wide suggests lower (infranodal) escape.
- 🧠 Note: If the atrial rhythm is atrial fibrillation, there are no P waves-you’ll see a slow regular escape rhythm with AV dissociation.
🧩 Causes
- ❤️ Inferior MI (RCA involvement affecting AV nodal blood supply) - can be transient.
- 🧱 Anterior MI - suggests extensive myocardial/conduction system damage; often more unstable.
- 💊 Medications: β-blockers, digoxin, rate-limiting calcium-channel blockers (verapamil/diltiazem), and some antiarrhythmics.
- 🧓 Degenerative fibrosis/sclerosis of conduction tissue (older adults).
- 🦠 Myocarditis, endocarditis (incl. peri-annular abscess), post-surgery, rheumatic fever.
- 🪲 Lyme disease, diphtheria (rare in UK but classic exam causes).
🩺 Clinical features
- 🚑 Acute: symptomatic bradycardia, low BP, shock, syncope (Stokes–Adams), acute heart failure.
- 🧍 Chronic: reduced exercise tolerance, fatigue, dizziness/presyncope.
- 🌊 JVP: cannon “a” waves can occur due to atrial contraction against a closed tricuspid valve.
🔎 Investigations
- 📈 ECG (diagnostic) + continuous monitoring.
- 🧪 U&E (K+), Mg/Ca, TFTs, glucose; troponin if ACS suspected; drug levels where relevant (e.g., digoxin).
- 🖥️ Echo if structural disease/MI suspected or ongoing instability.
💊 Management
- 🛟 ABCDE and resuscitation as needed; treat shock/ACS in parallel.
- 💉 Consider atropine, isoprenaline infusion (bridge), and temporary pacing (transcutaneous → transvenous) depending on stability and ECG features.
- 🧯 Treat reversible causes: stop AV nodal drugs, correct hyperkalaemia, manage MI/myocarditis/infection.
- 🧷 Most patients with persistent complete heart block will require a permanent pacemaker after specialist assessment.
📚 References (UK + core)
- Resuscitation Council UK. Concise adult bradyarrhythmia guidance (includes atropine dosing and escalation to pacing).
- British Heart Rhythm Society (BHRS). Standards for implantation and follow-up of cardiac rhythm management devices in adults (2024).
- ESC Guidelines on cardiac pacing and cardiac resynchronization therapy (2021).
- ACC/AHA/HRS Guideline on the evaluation and management of bradycardia and cardiac conduction delay (2018).
- BMJ Best Practice. Atrioventricular block.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
