| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Promyelocytic Leukaemia (APML)
Related Subjects: | Leukaemias in General | Acute Promyelocytic Leukaemia | Acute Myeloblastic Leukaemia (AML) | Acute Lymphoblastic Leukaemia (ALL) | Chronic Lymphocytic Leukaemia (CLL) | Chronic Myeloid Leukaemia (CML) | Hairy Cell Leukaemia | Differentiation Syndrome | Tretinoin (All-trans-retinoic acid (ATRA)) | Haemolytic Anaemia | Immune (Idiopathic) Thrombocytopenic Purpura (ITP)
Here is the cleaned, semantically improved, and compliant HTML for Acute Promyelocytic Leukaemia (APML), including the addition of relevant NICE guidelines in the references section. ```htmlAcute Promyelocytic Leukaemia (APML) is a subtype of Acute Myeloid Leukaemia (AML) 🧬 characterized by the accumulation of abnormal promyelocytes in the bone marrow 🦴 and blood. It is distinct due to the translocation t(15;17), producing the PML-RARα fusion protein, which blocks normal differentiation of myeloid cells. APML carries a particularly high risk of Disseminated Intravascular Coagulation (DIC) ⚠️ but is also one of the most treatable forms of AML when identified promptly and treated with ATRA (all-trans-retinoic acid) and arsenic trioxide. ✨
ℹ️ About
- A rare AML subtype, accounting for \~10–15% of AML cases.
- Notable for its strong association with DIC at presentation and during treatment.
- ATRA therapy directly targets the differentiation block caused by PML-RARα, making APML highly curable compared to other AMLs. 🎯
🧪 Key teaching point: Always suspect APML if a patient presents with cytopenias, abnormal promyelocytes on film, and unexplained bleeding/DIC → start ATRA immediately, even before confirmation.
🧬 Aetiology
- Genetic driver: Reciprocal translocation t(15;17).
- PML gene (chr 15) fuses with RARα gene (chr 17) → PML-RARα protein.
- This fusion protein blocks myeloid cell maturation and promotes apoptosis resistance.
- Result: Accumulation of promyelocytes, marrow failure, coagulopathy, and infection risk.
Auer Rods in APML
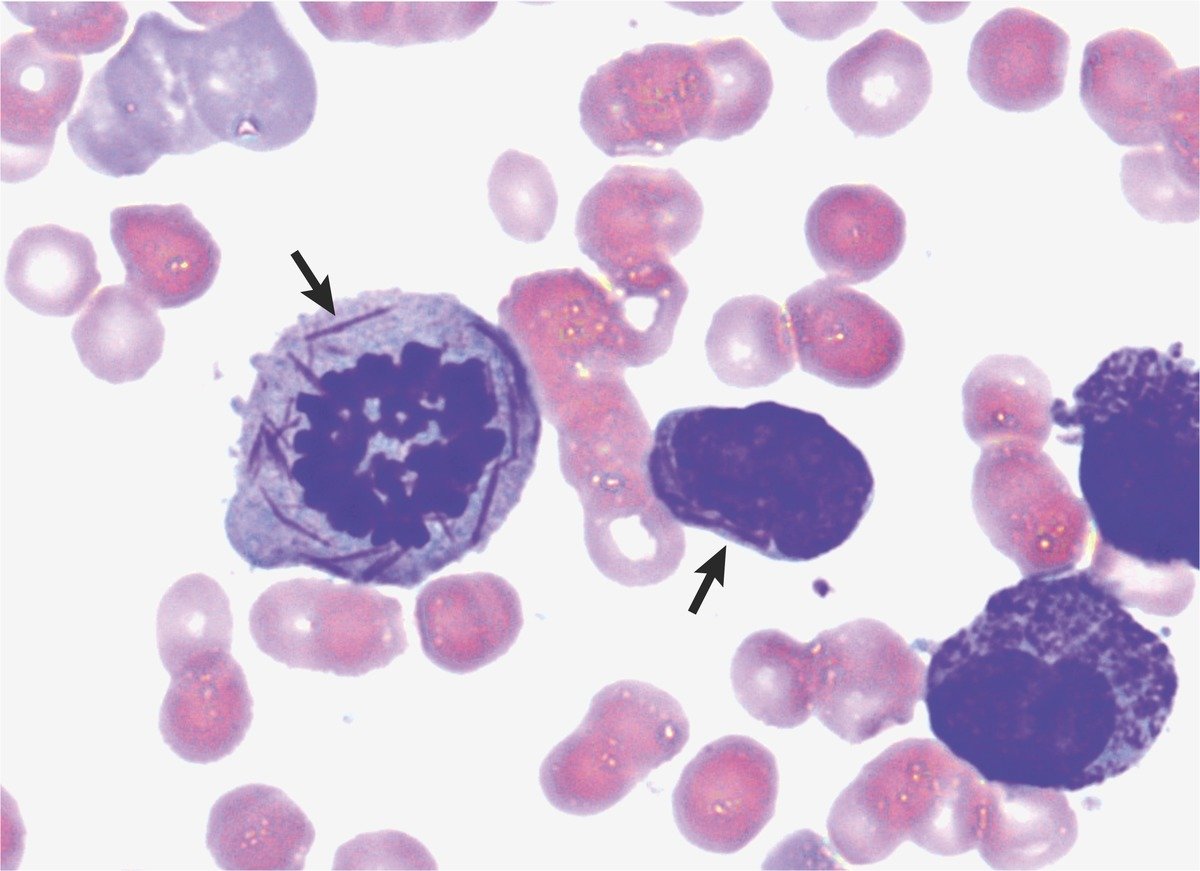
Auer rods (needle-like azurophilic inclusions) are often multiple and bundled (“faggot cells”) in APML 🔬
🩺 Clinical Features
- General AML symptoms: fatigue 😴, weight loss, anorexia.
- Marrow failure → anaemia, infections 🤒, bleeding 🩸.
- Bleeding risk disproportionately severe due to DIC (epistaxis, GI bleeding, intracranial haemorrhage).
- Low or high WCC possible, with abnormal promyelocytes visible on smear.
🔎 Investigations
- FBC: Pancytopenia with circulating promyelocytes.
- Coagulation screen: Prolonged PT/aPTT, low fibrinogen, raised D-dimer → DIC ⚠️
- Bone marrow biopsy: Abundant promyelocytes, often with “faggot” Auer rods.
- Cytogenetics: t(15;17) confirming diagnosis.
- Flow cytometry: Myeloid immunophenotype (CD33+, MPO+).
💊 Management
- Urgent ATRA therapy: Vitamin A derivative that releases the differentiation block, allowing promyelocytes → mature neutrophils. ⭐
- Arsenic trioxide: Now standard with ATRA for front-line therapy; excellent remission rates.
- Anthracyclines (e.g. daunorubicin): Sometimes combined in high-risk disease.
- DIC management: Platelet transfusions (maintain >30–50 × 10&sup9;/L), FFP, cryoprecipitate for fibrinogen support.
- Tumour lysis prophylaxis: Hydration + allopurinol/rasburicase 💧
⚠️ Differentiation Syndrome (formerly Retinoic Acid Syndrome)
- Occurs in up to 25% of patients within 3 weeks of ATRA initiation.
- Symptoms: Fever 🌡️, weight gain, dyspnoea, pulmonary infiltrates, pleural/pericardial effusions.
- Pathophysiology: Cytokine storm from rapidly differentiating myeloid cells.
- Management: High-dose IV dexamethasone 💊; temporary interruption of ATRA in severe cases.
🏁 Prognosis
- APML is now considered the most curable AML subtype 🎉
- Cure rates >85% with ATRA + arsenic-based regimens.
- Biggest danger = early death from haemorrhage (esp. intracranial) → emphasises need for immediate recognition and treatment.
🧑⚕️ Case Examples - Acute Promyelocytic Leukaemia (APML)
-
Case 1 (Bleeding & DIC at presentation): ⚠️
A 29-year-old woman presents with gum bleeding, epistaxis, and widespread petechiae. Bloods: Hb 8.5 g/dL, WCC 3.0 × 10&sup9;/L, platelets 18 × 10&sup9;/L. Coagulation: prolonged PT, low fibrinogen, raised D-dimer. Blood film shows abnormal promyelocytes with Auer rods.
Diagnosis: APML complicated by disseminated intravascular coagulation (DIC).
Management: Start all-trans retinoic acid (ATRA) immediately (before cytogenetic confirmation), aggressive clotting factor replacement (cryoprecipitate, platelets, FFP), and urgent haematology referral. -
Case 2 (Incidental cytopenias): 🩸
A 42-year-old man referred by GP for unexplained bruising and fatigue. FBC shows Hb 9.1 g/dL, WCC 2.5 × 10&sup9;/L, platelets 30 × 10&sup9;/L. Coagulation screen shows early derangement. Peripheral smear: promyelocytes with heavy granules. Cytogenetics: t(15;17) translocation (PML-RARA fusion).
Diagnosis: Acute Promyelocytic Leukaemia.
Management: Immediate ATRA + arsenic trioxide initiated, with supportive transfusion strategy. Patient placed on tumour lysis prophylaxis (rasburicase, IV fluids). Prognosis good with rapid treatment. -
Case 3 (High WCC hyperleukocytosis): 🫁
A 36-year-old woman presents with dyspnoea, headache, and blurred vision. Bloods: WCC 85 × 10&sup9;/L, blasts with promyelocyte morphology, abnormal coagulation.
Diagnosis: APML with hyperleukocytosis and risk of leukostasis.
Management: Start ATRA immediately, plus induction chemotherapy (idarubicin + arsenic trioxide). ICU support for TLS risk, hydroxycarbamide to reduce leukocyte count. Close monitoring for differentiation syndrome once therapy initiated (managed with steroids if develops).
📋 References & NICE Guidelines
- Cancer Research UK - APML
- Leukaemia Care - APML
- NCCN AML Guidelines
- NICE NG47: Haematological cancers: improving outcomes
- NICE TA526: Arsenic trioxide for treating acute promyelocytic leukaemia – Guidance on the use of arsenic trioxide (often in combination with ATRA) for untreated, low-to-intermediate risk APML.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
