| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
The Aorta
Related Subjects: |Aorta |Acute Coronary Syndrome (ACS) General |Aortic Dissection |Acute Heart Failure and Pulmonary Oedema |Aortic Regurgitation (Incompetence) |Aortic Stenosis |Aortic Sclerosis |Transcatheter aortic valve implantation (TAVI)
🫀 The aorta is the body’s largest elastic artery, carrying oxygenated blood from the left ventricle to the systemic circulation. It functions as a pressure reservoir (Windkessel effect): elastic recoil during diastole sustains forward flow and protects microcirculation from extreme pulsatility. Anatomically, it is best understood as aortic root → ascending aorta → arch → descending thoracic aorta → abdominal aorta, each with distinct relations, branch patterns, and clinical syndromes.
🔗 Helpful links: | NHS AAA Screening (patient) | NICE NG156: AAA (diagnosis & management) | RCEMLearning: Aortic dissection classification | Radiopaedia: Abdominal aorta (radiology)
🧩 Macro-anatomy: segments, vertebral levels, and key landmarks
- Aortic root (within pericardium)
- Includes the aortic valve, aortic annulus, and sinuses of Valsalva.
- Right and left coronary ostia arise from the right and left aortic sinuses.
- Sinotubular junction marks transition from root to ascending aorta.
- Clinical: dilation of the root can cause aortic regurgitation; aneurysm here risks coronary ostial compromise.
- Ascending aorta
- Begins at the aortic valve and runs superiorly within the pericardial sac.
- Relations (high-yield): pulmonary trunk anterior/left; right atrium to the right; SVC nearby.
- Ends at the level of the sternal angle where it becomes the arch.
- Aortic arch
- Curves posteriorly and to the left over the left main bronchus (“arch over the root of the left lung”).
- Landmarks:
- Arch branches (proximal → distal): brachiocephalic trunk, left common carotid, left subclavian.
- Aortic isthmus: just distal to left subclavian; tethered by the ligamentum arteriosum (ductus arteriosus remnant).
- Relations (applied anatomy):
- Near trachea and oesophagus → large aneurysm may cause cough, dysphagia, or hoarseness.
- Left recurrent laryngeal nerve loops under the arch near ligamentum arteriosum → hoarseness can be a “mediastinal red flag”.
- Descending thoracic aorta
- Runs in the posterior mediastinum, typically left of midline, then approaches midline lower down.
- Passes through the diaphragm via the aortic hiatus (classically at T12).
- Abdominal aorta
- Begins below the diaphragm at the aortic hiatus (≈ T12) and ends at the bifurcation (≈ L4).
- Lies anterior to the vertebral bodies; the IVC is usually to the right.
- Clinical: a pulsatile epigastric mass may be felt in thin patients; expansile pulsation raises concern for AAA.
🧱 Micro-anatomy: why the aorta behaves the way it does
- Tunica intima: endothelial lining; site of atherosclerotic plaque development and intimal tears in dissection.
- Tunica media: rich in elastin and smooth muscle; provides compliance. “Cystic medial degeneration” (e.g., connective tissue disease) predisposes to aneurysm/dissection.
- Tunica adventitia: collagen-rich support; contains the vasa vasorum and autonomic nerves.
- Vasa vasorum: supply outer media/adventitia (especially thoracic aorta). Compromise can contribute to medial ischemia and weakening.
🌿 Branches of the aorta (organise by segment and by ‘visceral vs parietal’)
1) Ascending aorta
- Coronary arteries: right and left coronary arteries arise from the aortic sinuses to perfuse myocardium.
2) Aortic arch branches
- Brachiocephalic trunk → right common carotid + right subclavian.
- Left common carotid → head/neck.
- Left subclavian → left upper limb; gives vertebral artery to posterior circulation.
3) Descending thoracic aorta branches
- Posterior intercostal arteries (classically 3–11) + subcostal artery → chest wall; collateral pathways in coarctation.
- Bronchial arteries → bronchial tree (systemic, oxygenated supply).
- Oesophageal branches → oesophagus.
- Mediastinal/pericardial branches → mediastinal tissues/pericardium.
- Superior phrenic arteries → diaphragm.
4) Abdominal aorta branches (high-yield table)
| Category | Branches | Core territory (clinical angle) |
|---|---|---|
| Unpaired visceral (midline) |
🌟 Coeliac trunk
🟦 Superior mesenteric artery (SMA) 🟩 Inferior mesenteric artery (IMA) |
Foregut / Midgut / Hindgut supply (think: bowel ischaemia territories, collateral arcades) |
| Paired visceral (lateral) |
Renal arteries
Gonadal (testicular/ovarian) arteries Middle suprarenal arteries |
Kidney perfusion and renovascular HTN; gonadal pain patterns; adrenal vascular richness |
| Parietal |
Inferior phrenic arteries
Lumbar arteries Median sacral (small midline) |
Diaphragm, posterior abdominal wall; collaterals to pelvis |
| Terminal | Common iliac arteries (R/L) at L4 | Pelvis and lower limbs (internal vs external iliac territories) |
🧠 Exam memory hook: Abdominal midline unpaired branches = “CSI” (Coeliac, SMA, IMA). Pair them with renal + gonadal laterally, and finish with the L4 bifurcation.
📍 Relations and surface anatomy (why symptoms happen)
- Thoracic aorta lies close to oesophagus and left main bronchus → aneurysm may cause dysphagia, cough, or recurrent laryngeal nerve palsy (hoarseness).
- Abdominal aorta is retroperitoneal; AAA can erode vertebral bodies (back pain) or compress adjacent structures.
- Left renal vein crosses anterior to aorta under the SMA (“nutcracker” region) - helpful landmark in imaging.
- Aortic plexus (sympathetic fibres) surrounds the aorta; irritation can contribute to visceral pain patterns.
🧫 Embryology (make it clinically relevant)
- Aortic arch derivatives: largely from pharyngeal arch arteries (key for congenital arch anomalies).
- Ligamentum arteriosum is the remnant of the ductus arteriosus and anchors the isthmus.
- Coarctation often occurs near the ductal region; collaterals develop via intercostals → classic rib notching.
📷 Anatomy images (keep)
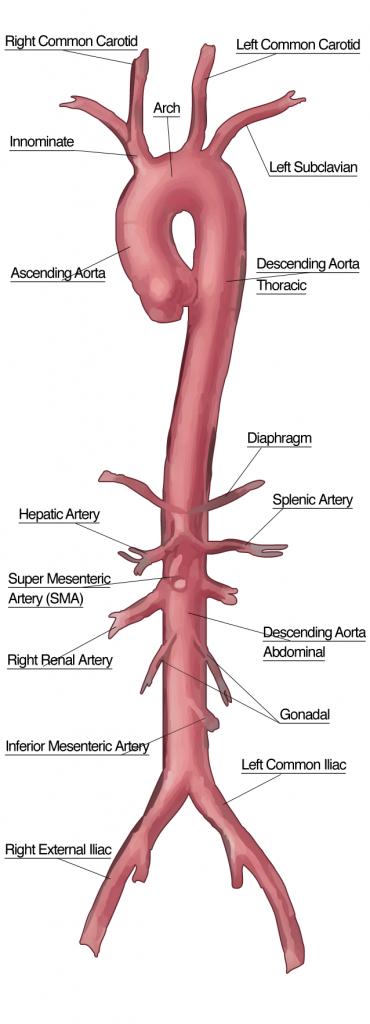
📸 Lateral Radiology (keep)
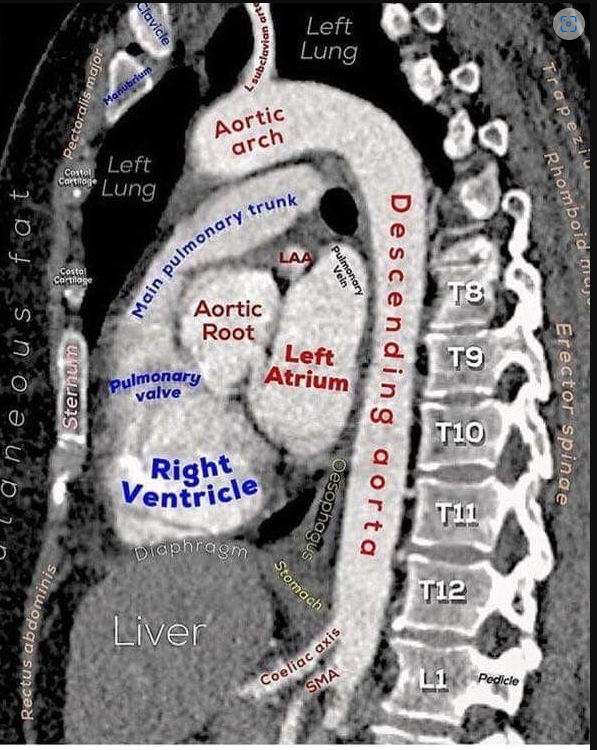
⚙️ Key functions (link anatomy to physiology)
- Oxygenated blood distribution: conduit from LV to all systemic beds.
- Pressure reservoir (Windkessel): elastin-rich media stores systolic energy → diastolic recoil.
- Pulse dampening: reduces pulsatile stress downstream; loss of compliance increases pulse pressure.
- Pulse wave velocity: rises as the aorta stiffens (ageing/atherosclerosis) and correlates with cardiovascular risk.
🧪 Imaging anatomy (what each modality shows best)
- Ultrasound: first-line for AAA screening and surveillance; best for diameter measurement.
- CT angiography: defines anatomy for operative planning (neck length, branch involvement) and dissection mapping.
- Chest X-ray: may show widened mediastinum/abnormal aortic contour (non-specific but important context).
- MRI/MRA: useful in selected cases; avoids ionising radiation.
🚨 Clinical relevance (retain, but tighten and anatomise)
- 🔴 Aortic aneurysm
- Most commonly abdominal (infrarenal), but can be thoracic/root.
- Risk factors: smoking, hypertension, atherosclerosis; connective tissue disorders (thoracic/root).
- Applied anatomy: infrarenal aneurysms relate to renal arteries (suprarenal involvement raises operative complexity).
- UK: men are invited for AAA screening in the year they turn 65 (England).
- 🩸 Aortic dissection
- Intimal tear → blood tracks into media → false lumen; branch vessels may be occluded (malperfusion).
- Stanford A involves ascending aorta; Stanford B does not involve ascending aorta.
- Applied anatomy: ascending involvement risks coronary ostia, aortic valve, and pericardial tamponade.
- 🍼 Coarctation
- Typically juxtaductal (near ligamentum arteriosum).
- Collateral circulation via intercostals → rib notching.
- Clinical: radio-femoral delay; upper limb HTN with lower limb hypotension.
- ⚖️ Aortic valve disorders
- Root/ascending aorta pathology can coexist with bicuspid aortic valve disease.
- Root dilation → regurgitation; calcific stenosis → LV pressure overload.
📝 Summary
The aorta is an elastic conduit and pressure reservoir whose anatomy maps directly to clinical presentations: root and ascending disease affects the valve/coronaries; arch disease can affect airway/oesophagus and the left recurrent laryngeal nerve; thoracic branches supply chest wall and viscera; abdominal branches follow a predictable pattern (CSI + paired laterals) before bifurcating at L4. A strong mental model of segments + branches + relations makes aneurysm, dissection, and coarctation far easier to recognise and localise.
📷 Anatomy (keep)
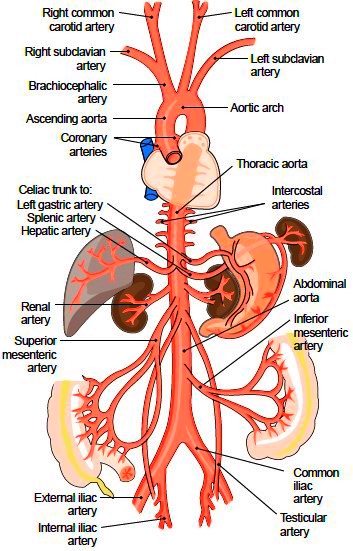
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
