| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Pityriasis or Tinea versicolor infections
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
📖 About
- Pityriasis (Tinea) Versicolor is a common superficial fungal infection caused by yeasts of the Malassezia genus.
- Seen mainly in adolescents and young adults 👩🦱👨🦱, especially in warm and humid climates 🌴.
- Most patients are otherwise healthy, though immunocompromised individuals are at increased risk.
- Previously called Malassezia furfur infection.
🧬 Aetiology & Pathophysiology
- Caused by Pityrosporum orbiculare (round yeast form) and Pityrosporum ovale (oval form).
- Thrives in oily (sebaceous) areas – the organism metabolises skin lipids (free fatty acids & triglycerides).
- Alters melanocyte function → causes hypo- or hyperpigmentation due to uneven melanin production.
- Relapse is common because the organism is part of the normal skin flora.
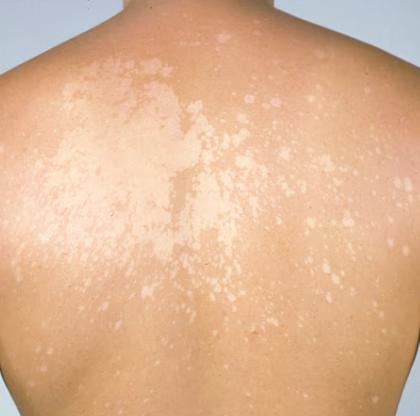
👀 Clinical Features
- Usually asymptomatic, but may cause mild pruritus.
- Multiple small, circular macules – colour may vary (white, pink, brown).
- Often on trunk, neck, upper arms; more obvious after sun exposure ☀️ (hypopigmented patches fail to tan).
- Risk factors: oily skin, sweating, immunosuppression, humid climates.
🔎 Investigations
- Wood’s lamp: yellow-green fluorescence ✨ of affected areas.
- Microscopy (KOH prep): shows the “spaghetti and meatballs” pattern (hyphae + spores).
- Skin biopsy: rarely needed, only if atypical.
💊 Management
- Topical therapy first-line:
- Ketoconazole 2% shampoo – applied scalp → thighs, left 5 min, once daily for 3 days (or single application).
- Alternatives: Selenium sulphide or other azole creams (ketoconazole/clotrimazole BD for small areas).
- Systemic therapy: Reserved for extensive/refractory disease:
- Itraconazole 200 mg daily × 7 days → ~90% cure rate at 4 weeks.
- Griseofulvin ineffective ❌.
- Recurrence is common: intermittent use of medicated shampoo (weekly/monthly) as prophylaxis.
- Note: pigmentary changes may take months to resolve – reassure patients that this does not reflect treatment failure.
✅ Key Exam Pearls
- Caused by Malassezia species → not dermatophytes.
- “Spaghetti and meatballs” appearance on microscopy 🍝.
- Wood’s lamp = yellow-green fluorescence.
- First-line = ketoconazole shampoo, not griseofulvin.
- Pigmentary changes may persist for months despite cure.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
