| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Langerhans cell histiocytosis (LCH)
🧩 Langerhans Cell Histiocytosis (LCH) is a rare histiocytic disorder with features overlapping cancer, immune dysregulation, and inflammation. ⚖️ Experts still debate whether it should be considered a true cancer or a clonal immune disorder.
📖 About
- Rare disorder of proliferating Langerhans cells (specialised dendritic immune cells).
- Typically affects children and young adults.
- Historical term: Histiocytosis X.
- Pediatric form is often called eosinophilic granuloma.
🧬 Aetiology & Pathogenesis
- BRAF V600E mutations present in ~50% of cases → abnormal MAPK signalling.
- Leads to clonal expansion of histiocytes with cytokine release and tissue damage.
- Granuloma formation may occur in multiple organs (skin, bone, lungs, pituitary, thyroid, lymph nodes).
- Adult pulmonary LCH strongly associated with cigarette smoking.
🔎 Variants / Clinical Syndromes
- Hashimoto–Pritzker disease → congenital, self-healing skin form.
- Letterer–Siwe disease → acute, disseminated, severe, often in infants.
- Hand–Schüller–Christian disease → chronic, triad of diabetes insipidus, exophthalmos, lytic bone lesions.
- Eosinophilic granuloma → solitary or few bone lesions; most benign end of spectrum.
🩺 Clinical Features
- Bone lesions (esp. lytic skull lesions).
- Pulmonary involvement → cysts, pneumothorax, haemoptysis.
- Endocrine dysfunction → hypothalamic involvement causing diabetes insipidus (polyuria, hypernatraemia).
- CNS → cerebellar demyelination and neurodegeneration (rare).
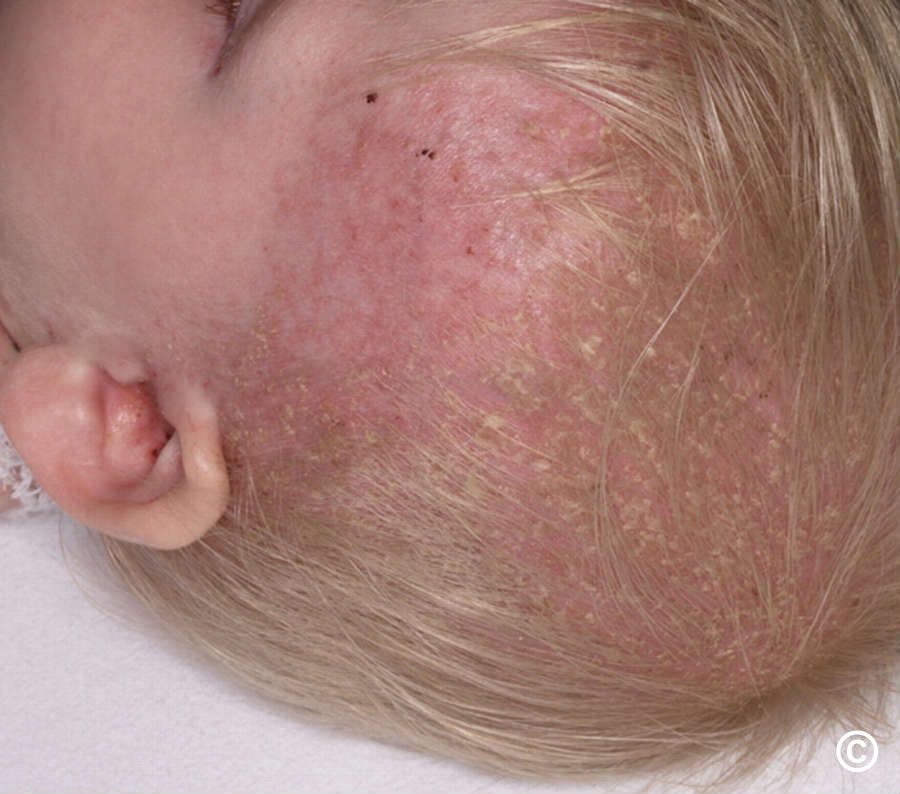
- Cutaneous, oral, and nail lesions possible.
🧪 Investigations
- X-ray / CT: lytic bone lesions, especially skull.
- HRCT chest: apical cysts and nodules (risk of recurrent pneumothorax).
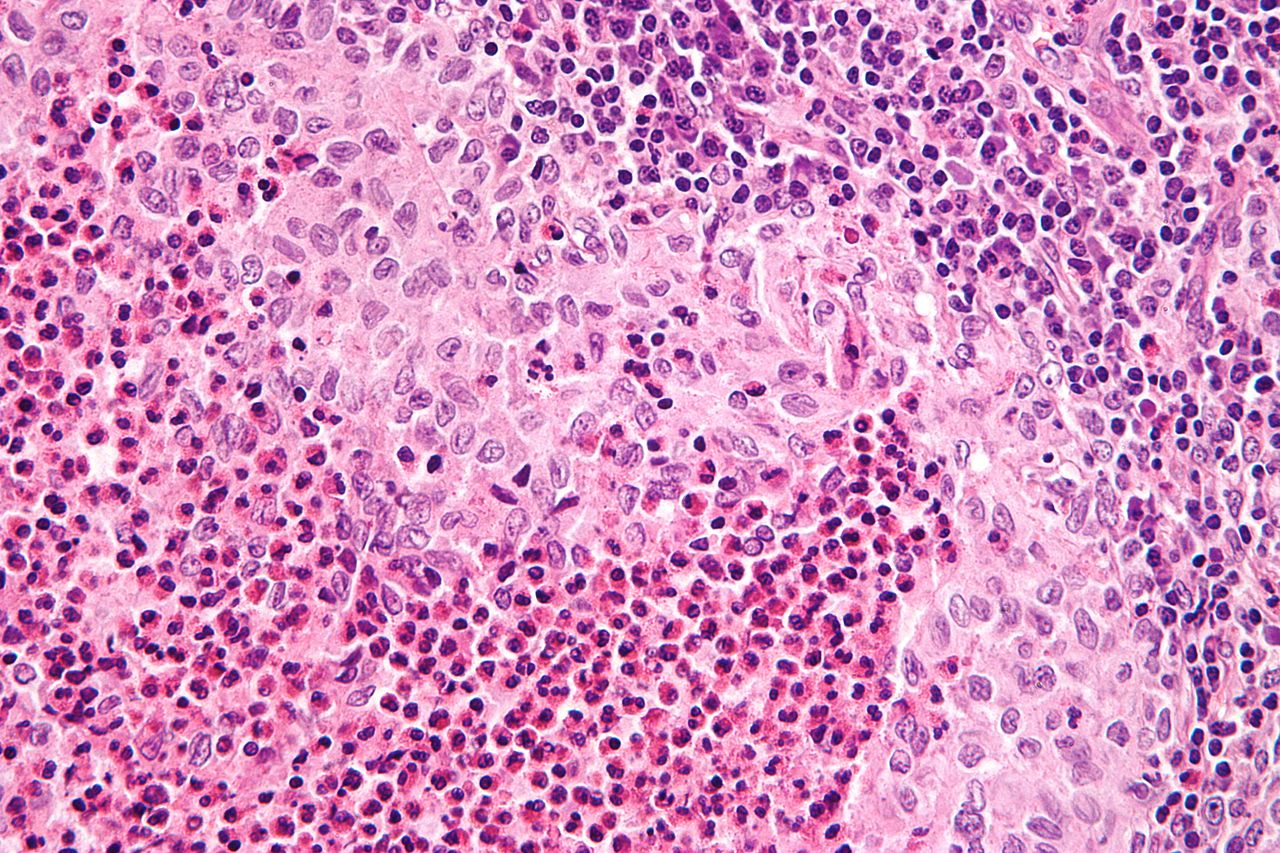
- Biopsy: Langerhans cells with coffee-bean nuclei, mixed with eosinophils. Immunohistochemistry: CD1a+, S100+, langerin+ (Birbeck granules on EM).
- Bloods: Hypernatraemia from diabetes insipidus, variable cytopenias.
⚖️ Differential Diagnosis
- Sarcoidosis.
- Lymphoma or metastatic bone disease.
- Granulomatous infections (TB, fungal).
💊 Management
- General: Multidisciplinary (haematology, oncology, respiratory, endocrinology).
- First-line: Corticosteroids for symptomatic disease.
- Systemic therapy: Vinblastine, cytarabine, methotrexate for multisystem disease.
- Targeted therapy: BRAF inhibitors (e.g., vemurafenib) in refractory BRAF-mutant cases.
- Supportive: Endocrine replacement for diabetes insipidus, stop smoking in pulmonary LCH.
- Prognosis variable: from self-resolving to progressive respiratory failure (~10% mortality in pulmonary LCH).
📚 References
3 Clinical Cases - Langerhans Cell Histiocytosis (LCH) 🧬🫁
- Case 1 - Smoker with cystic lung disease 🚬: A 32-year-old man, heavy smoker, presents with progressive dry cough and dyspnoea. HRCT shows bizarre-shaped cysts and nodules predominantly in the upper lobes, sparing the costophrenic angles. Teaching: Pulmonary LCH is strongly associated with cigarette smoking. Imaging shows characteristic cysts + nodules. Stopping smoking is the cornerstone of treatment; advanced disease may progress to pulmonary hypertension or require transplant.
- Case 2 - Young adult with bone lesions 🦴: A 24-year-old woman presents with persistent bone pain and swelling in the skull. Biopsy reveals CD1a+ and langerin+ cells. She later develops cough and recurrent pneumothoraces. Teaching: LCH can present with systemic disease affecting bone, skin, pituitary, and lung. In adults, lung involvement is often linked to smoking. Pneumothorax results from rupture of subpleural cysts. Multisystem disease may require chemotherapy (e.g. vinblastine).
- Case 3 - Child with systemic LCH 👶: A 7-year-old boy presents with skin rash, diabetes insipidus, hepatosplenomegaly, and recurrent chest infections. CXR shows bilateral nodular opacities and cystic changes. Teaching: Paediatric LCH often affects multiple systems - skin, bone, lung, pituitary, liver, and marrow. Lung disease in children is less commonly smoking-related but may cause chronic interstitial changes. Management depends on extent: local lesions may be observed; systemic disease often needs steroids + chemotherapy.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
