| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Benign Prostatic Hyperplasia✅
Related Subjects: |Urothelial tumour s |Haematuria |Acute Urinary Retention |Anuria and Oliguria |Bladder cancer |Renal cell carcinoma |Benign Prostatic Hyperplasia |IgA nephropathy |Prostate Cancer |Henoch-Schonlein purpura |Glomerulonephritis
🔵 Benign Prostatic Hyperplasia (BPH) / Male LUTS usually affects the peri-urethral (transition) zone of the prostate. 📏 Importantly, prostate size does not always correlate with urinary obstruction.
📌 About
- Male LUTS may arise from BPH, detrusor overactivity, impaired contractility, or mixed mechanisms 🚻.
- Prostate size alone is not a reliable predictor of obstruction 🚫.
- Assessment guided by IPSS score, DRE, PSA, and symptom diary aligns with NICE CG97 guidance.
🧬 Pathology
- Represents hyperplasia (increase in cell number) rather than hypertrophy.
- Confined mainly to the peri-urethral (transition) zone.
- Chronic obstruction → detrusor hypertrophy → trabeculation → impaired emptying.
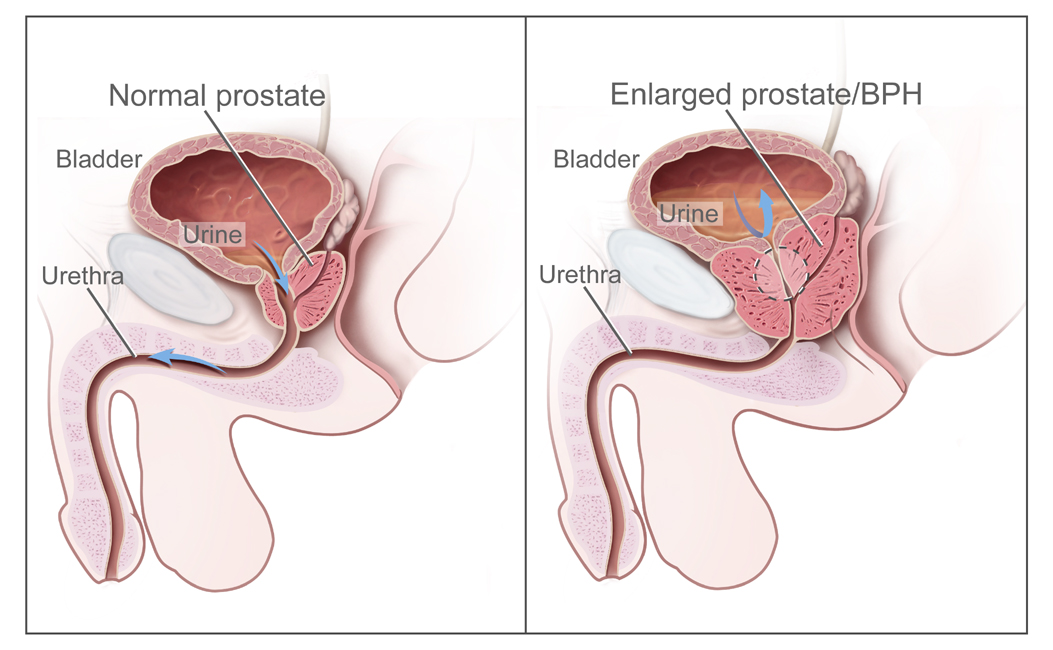
👨 Clinical Features
- Common in men >50 yrs; prevalence: Black > White > Asian.
- Voiding symptoms: weak stream, hesitancy, terminal dribbling 🚽.
- Storage symptoms: frequency, urgency, nocturia ⏰.
- Incomplete emptying → chronic retention with large bladder.
- Exam: smooth enlarged prostate, palpable bladder.
⚠️ Complications
- Acute urinary retention (may be worsened by drugs ❗ e.g., anticholinergics, antihistamines, antidepressants).
- Recurrent UTIs 🦠.
- Hydroureter, hydronephrosis, renal impairment 🩸.
- Bladder calculi & infection.
🔍 Investigations
- Symptom assessment: IPSS or AUASS score.
- Urinalysis (MSU if positive); haematuria → rule out malignancy 🔎.
- Bloods: U&E, FBC, PSA (interpret carefully: ↑ in BPH, infection, recent catheterisation).
- Post-void residual (PVR) via bladder scan or ultrasound; >150 mL may indicate impaired emptying.
- Frequency-volume chart (2–3 days) to assess LUTS patterns.
- Abdominal ultrasound: kidney size, hydronephrosis, bladder wall changes.
- Flexible cystoscopy if haematuria, obstruction, or uncertain diagnosis.
- Urodynamics: only in complex cases (neurogenic bladder or failed prior surgery).
💡 General Lifestyle Advice
- Limit alcohol 🍺, caffeine ☕, and evening fluids.
- Avoid decongestants/antihistamines as they worsen retention.
- Bladder training: urinate regularly (every 4–6 hrs), double voiding helps empty residual urine.
- Maintain healthy weight & stay active 🏃 – reduces retention risk.
- Keep warm 🧥 – cold exposure may trigger urinary retention.
💊 Medical Management (NICE CG97)
- Alpha-blockers (Tamsulosin, Alfuzosin): relax smooth muscle → rapid symptom relief (days–weeks). ⚠️ SE: postural hypotension, dizziness.
- 5-alpha reductase inhibitors (Finasteride, Dutasteride): shrink prostate gradually (3–6 months), reduce long-term risk of retention/surgery. ⚠️ SE: retrograde ejaculation, reduced libido.
- Combination therapy: alpha-blocker + 5-ARI for large prostates or severe symptoms.
- Anticholinergics (Oxybutynin): for storage symptoms; caution in elderly/frail (delirium risk).
- Mirabegron: β3 agonist alternative for overactive bladder; SE: hypertension.
🧴 Catheterisation & TWOC
- Acute retention: catheterise + start alpha-blocker → trial without catheter (TWOC) in 2–7 days.
- If TWOC fails: intermittent self-catheterisation or long-term catheter (urethral/suprapubic).
- Severe chronic retention (>800–1000 mL) may require long-term catheterisation.
📤 Indications for Urology Referral
- Suspicion of malignancy (hard nodular prostate, elevated PSA).
- Obstructive uropathy: AKI, raised urea/creatinine.
- Large bladder, recurrent retention, or hydronephrosis.
- Rapidly worsening LUTS or failure of medical therapy.
🔪 Surgical Options
- TURP: gold standard for moderate prostate size; removes obstructive tissue via resectoscope. SE: bleeding, TURP syndrome, clot retention, stricture, retrograde ejaculation, incontinence.
- HoLEP (Holmium Laser Enucleation): preferred for large prostates; less bleeding, durable results, shorter catheter time.
- Minimally invasive: UroLift, Rezūm (for select patients prioritising ejaculation preservation).
- Open prostatectomy: for very large prostates or complex anatomy.
Case 1 – Mild Symptoms
58-year-old with daytime frequency and nocturia ×2. DRE normal, PSA normal, PVR 40 mL. Implement lifestyle modifications. If symptoms persist, start an alpha-blocker and review in 4–6 weeks.
Case 2 – Moderate Symptoms, Enlarged Prostate
66-year-old, IPSS 18, smooth prostate, PSA 2.4 µg/L, volume ~45 mL, PVR 120 mL. Start tamsulosin and 5-alpha-reductase inhibitor. Consider mirabegron if storage symptoms persist and PVR is low.
Case 3 – Acute Urinary Retention
74-year-old unable to void. Catheterise, start alpha-blocker, check for UTI or culprit meds. Plan TWOC in 2–7 days. If failure or complications, refer for surgery (TURP/HoLEP) depending on prostate size and patient fitness.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
