| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cerebral Arterial Perfusion and Clinical Correlates
Related Subjects:
|Neurological History taking
|Causes of Stroke
|Ischaemic Stroke
|Subarachnoid Haemorrhage
|Small Vessel Disease
|Vascular Dementia
|Capsular and Pontine Warning Syndromes
|Dementias
|CADASIL
|CARASIL
|Cerebral Arterial Perfusion and Clinical Correlates
|Anterior circulation Brain
|Posterior circulation Brain
|Acute Stroke Assessment (ROSIER&NIHSS)
|Carotid Artery dissection
|Vertebral artery dissection
|Acute Stroke Assessment (ROSIER&NIHSS)
|Atrial Fibrillation
|Atrial Myxoma
|Causes of Stroke
|Ischaemic Stroke
|Cancer and Stroke
|Cerebral Venous thrombosis
|Cardioembolic stroke
|CT Basics for Stroke
|Endocarditis and Stroke
|Haemorrhagic Stroke
|Stroke Thrombolysis
|Hyperacute Stroke Care
|AP of the Brain
|Cryptogenic stroke
|Carotid Web
|Anterior / Medial Medullary Infarct (Dejerine Syndrome)
🧠 Vascular Territories of the Brain
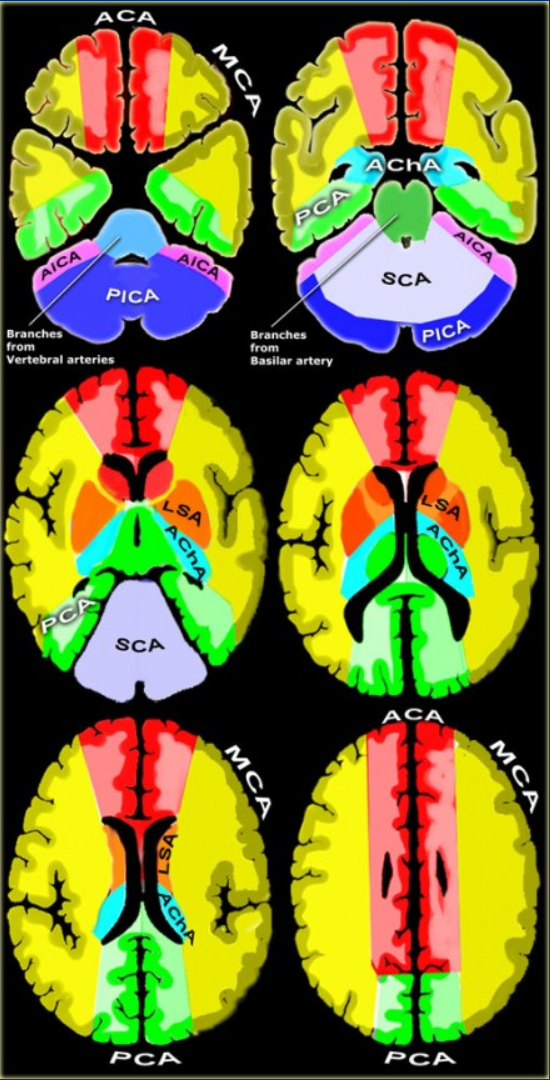
🔴 Internal Carotid Artery (ICA)
👁 Ophthalmic Artery
🔗 Posterior Communicating Artery
🟡 Anterior Choroidal Artery
🟥 Anterior Cerebral Artery (ACA)
🟦 Middle Cerebral Artery (MCA)
🟣 Posterior Cerebral Artery (PCA)
🟤 Basilar Artery
🌐 Midbrain Syndromes
🔵 Pons Syndromes
🟢 Medullary Syndromes
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
