| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Vagus Nerve (Cranial Nerve X)
Related Subjects: |Olfactory Nerve |Optic Nerve |Oculomotor Nerve |Trochlear Nerve |Trigeminal Nerve |Abducent Nerve |Facial Nerve |Vestibulocochlear Nerve |Glossopharyngeal Nerve |Vagus Nerve |Accessory Nerve
“Vagus” comes from the Latin vagus, meaning wandering or roving. That name fits because cranial nerve X “wanders” a very long way compared with the other cranial nerves: it leaves the brainstem, passes through the neck, and sends branches into the thorax and abdomen (heart, lungs, oesophagus, stomach, intestines). For medical students, it’s a handy memory hook: if a symptom involves voice/swallowing and/or autonomic gut–heart–lung effects, CN X is often on the shortlist because it’s the cranial nerve with the widest distribution.
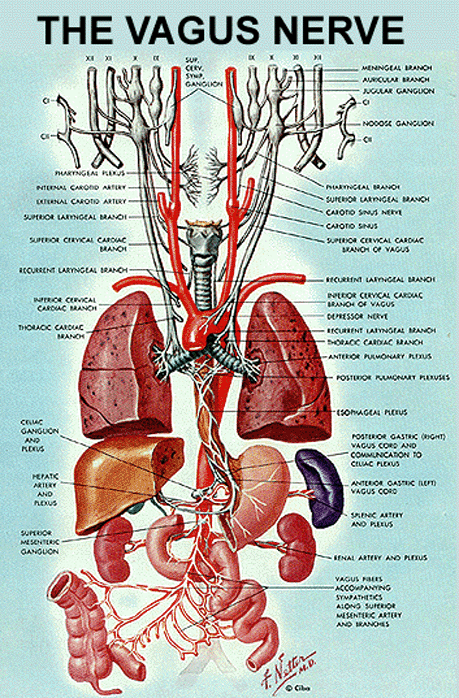
🧠 The vagus nerve (cranial nerve X) is the major parasympathetic outflow to the thorax and abdomen and a key mixed nerve in the head and neck. It carries motor fibres for swallowing and phonation, sensory fibres from the pharynx/larynx and visceral organs, and parasympathetic fibres that slow the heart, constrict bronchi, and drive gut motility and secretion. Because it interfaces with airway protection, voice, autonomic control, and “gut–brain” signalling, vagal pathology often presents as a combination of hoarseness + dysphagia + cough/aspiration risk + autonomic symptoms.
🧬 Brainstem nuclei
- Nucleus ambiguus (branchial motor): motor to pharynx/soft palate/larynx.
- Dorsal motor nucleus of vagus (parasympathetic): preganglionic parasympathetic to thoracoabdominal viscera.
- Nucleus solitarius (visceral sensory + taste): afferents from thorax/abdomen and taste from epiglottis.
- Spinal trigeminal nucleus (somatic sensory): small area of external ear/ear canal.
🧭 Course (med student version you can visualise)
- Exit: arises from lateral medulla → exits skull via jugular foramen (with CN IX, CN XI, IJV).
- Neck: descends in the carotid sheath (between internal jugular vein and carotid artery).
- Thorax: contributes to cardiac and pulmonary plexuses; gives recurrent laryngeal nerves.
- Oesophagus: forms oesophageal plexus → reorganises into vagal trunks entering the abdomen via the hiatus.
- Abdomen: parasympathetic supply to foregut and midgut (classically down to the proximal 2/3 of transverse colon).
⚙️ Functions (structured by fibre type)
- Branchial Motor (swallowing + voice)
- Soft palate: elevates palate to prevent nasal regurgitation (except tensor veli palatini = CN V3).
- Pharynx: coordinated pharyngeal constriction for swallowing (except stylopharyngeus = CN IX).
- Larynx: intrinsic muscles for phonation and airway protection.
- Parasympathetic (autonomic “rest-and-digest”)
- Heart: slows SA/AV node conduction via acetylcholine (M2) → bradycardia.
- Lungs: bronchoconstriction and increased mucus secretion.
- GI tract: increases peristalsis and secretion; relaxes sphincters in coordinated digestion.
- Visceral Sensory (afferents)
- Baroreceptor and chemoreceptor afferents (aortic arch) → reflex control of BP and respiration.
- Visceral sensation from thoracic and abdominal organs (often non-localising: nausea, fullness, discomfort).
- Somatic Sensory
- Small area of external ear/external auditory canal (auricular branch).
- Explains “ear-cough” reflex in some people (Arnold’s reflex).
🌿 Major branches (what they do + how they present clinically)
- Pharyngeal branch
- Main motor supply to pharynx and soft palate.
- Lesion → dysphagia, nasal speech, reduced palatal elevation.
- Superior laryngeal nerve
- Internal branch (sensory): laryngeal sensation above vocal folds (supraglottis) → cough reflex.
- External branch (motor): cricothyroid (tenses vocal cords) → pitch control.
- Injury (e.g., thyroid surgery) → weak voice, reduced ability to project/high pitch; aspiration risk if sensory loss.
- Recurrent laryngeal nerve (RLN)
- Right RLN loops under right subclavian artery; left RLN loops under aortic arch (near ligamentum arteriosum).
- Motor to all intrinsic laryngeal muscles except cricothyroid.
- Sensory to larynx below vocal folds.
- Lesion → hoarseness, weak cough, aspiration; bilateral lesion can cause airway compromise (cords near midline).
- Left RLN vulnerable in mediastinal pathology (e.g., enlarged left atrium, aortic aneurysm, bronchogenic carcinoma).
- Cardiac branches
- To cardiac plexus → slows heart rate and AV conduction.
- Important in vagal manoeuvres and vasovagal syncope.
- Pulmonary branches
- To pulmonary plexus → bronchomotor tone and secretion.
- Oesophageal plexus → vagal trunks
- Coordinate oesophageal peristalsis and lower oesophageal sphincter function.
- Relevant in dysmotility and after oesophageal surgery.
- Abdominal branches
- Foregut and midgut parasympathetic input: gastric acid secretion, pancreatic secretion, gallbladder contraction, peristalsis.
🩺 Bedside examination (simple but high value)
- Voice: listen for hoarseness/breathy voice (RLN dysfunction).
- Palate: ask patient to say “ah” → palate should elevate symmetrically; uvula deviates away from weak side.
- Swallow: cough after water, nasal regurgitation, “wet” voice → aspiration risk.
- Gag reflex: sensory limb mainly CN IX, motor limb mainly CN X (useful but uncomfortable-don’t rely on it alone).
🧠 Reasoning tip: If the main complaint is hoarseness, think RLN first (thyroid surgery, mediastinal mass, aortic arch pathology on the left). If it’s nasal speech + dysphagia, think pharyngeal branch/palatal weakness (often “high vagal” lesions near the skull base).
🚑 Clinical relevance (UK-style “what you’ll actually see”)
- Post-thyroid / parathyroid surgery
- RLN injury → hoarseness, aspiration; bilateral injury can obstruct airway.
- External SLN injury → loss of pitch/projection (singers notice this).
- Skull base / jugular foramen pathology
- Can affect CN IX, X, XI together → dysphagia + hoarseness + shoulder weakness (think jugular foramen syndromes).
- Vasovagal syncope
- Exaggerated vagal response → bradycardia and vasodilation → transient loss of consciousness.
- Triggers: pain, emotion, prolonged standing, venepuncture.
- Arrhythmias and vagal manoeuvres
- Valsalva (modified) can terminate some SVTs by increasing vagal tone to the AV node.
- Vagus nerve stimulation (VNS)
- Implanted device used in refractory epilepsy and some depression pathways.
- Side effects: hoarseness, cough, throat discomfort.
📌 Summary
The vagus nerve (CN X) is a mixed nerve from the medulla that exits via the jugular foramen and travels in the carotid sheath to the thorax and abdomen. It provides motor control of the palate/pharynx/larynx (swallowing + voice), visceral sensory input (including baro/chemoreceptor reflexes), and parasympathetic regulation of the heart, lungs, and gut. Clinically, remember: RLN = hoarseness, high vagal lesions = dysphagia + palatal weakness, and vagal overactivity can cause vasovagal syncope and influence SVT management.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
