| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Anatomy and Physiology of the vagina
Related Subjects: |Causes of abnormal Vaginal bleeding |Vaginal Carcinoma |Cervical cancer |Endometrial (Uterine) Cancer |Post Menopausal Bleeding |AP of the Uterus and Fallopian Tubes |AP of the Ovary |Gynaecological History Taking |Colposcopy |Premature Menopause |Polycystic Ovary syndrome
Overview
- The vagina is a fibromuscular canal extending from the vulva to the cervix, forming part of the lower female genital tract.
- Functions include sexual intercourse, menstrual outflow, and acting as the birth canal during vaginal delivery.
📍 Location and Relations
- Runs posterosuperiorly from the vestibule to the cervix (typically ~7–10 cm, variable).
- Anterior: bladder base and urethra.
- Posterior: rectum (upper posterior wall related to the pouch of Douglas/peritoneum).
- Lateral: levator ani and pelvic fascia; ureters lie close to the cervix (clinically relevant in surgery).
🧱 Gross Structure
- Upper end: surrounds the cervix to form the vaginal fornices (anterior, posterior, and two lateral).
- Lower end: opens into the vaginal vestibule (between the labia minora).
- Anterior vs posterior walls: the posterior wall is usually longer due to the cervix position.
- The mucosa forms transverse folds called rugae (more prominent in premenopausal states).
🔬 Histology
- Mucosa: stratified squamous non-keratinised epithelium (protective; no glands).
- Lamina propria: elastic fibres, venous plexuses, immune cells (local defence).
- Muscularis: smooth muscle (inner circular + outer longitudinal) with variable thickness.
- Adventitia: connective tissue anchoring to pelvic structures; contains vessels and nerves.
- No vaginal glands: lubrication mainly from cervical mucus and transudation through the vaginal wall; vestibular glands contribute to vulval lubrication.
🩸 Blood Supply
- Arterial supply: predominantly from the vaginal artery (branch of internal iliac) and contributions from the uterine artery and internal pudendal artery.
- Venous drainage: vaginal venous plexus → internal iliac veins (rich venous plexus can bleed significantly with trauma).
🧠 Nerve Supply
- Upper vagina (autonomic): visceral afferents via the uterovaginal plexus (inferior hypogastric plexus) → pain tends to be poorly localised.
- Lower vagina (somatic): via pudendal nerve → touch/pain is well localised (important for procedures and childbirth pain).
🧬 Lymphatic Drainage
- Upper vagina: internal iliac ± external iliac nodes.
- Middle vagina: internal iliac nodes.
- Lower vagina and introitus: superficial inguinal nodes.
- Clinically important for vaginal and cervical malignancy staging and patterns of spread.
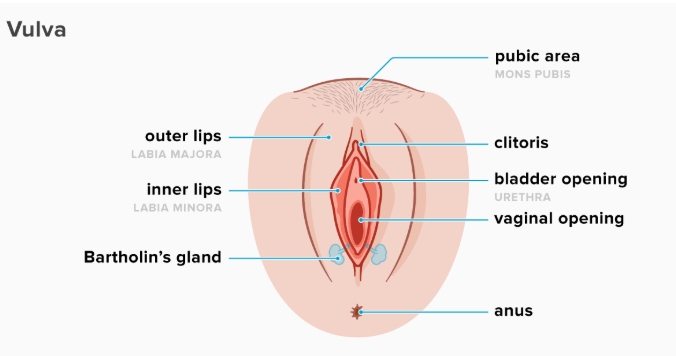
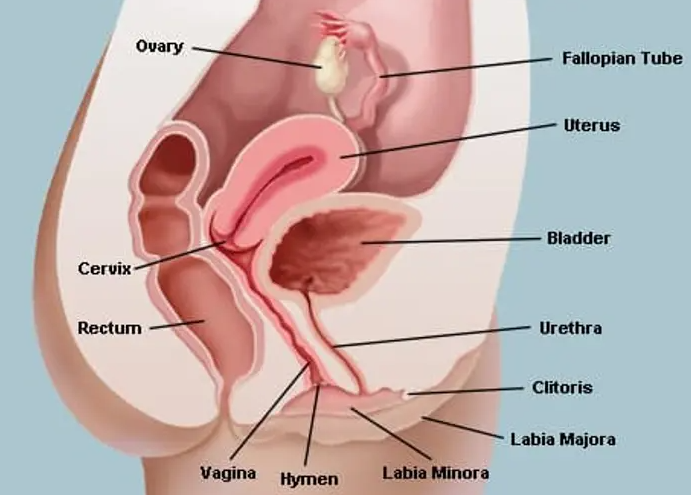
🏗️ Support and Pelvic Floor Relations
- Supported by the levator ani (especially pubococcygeus/puborectalis), perineal body, and endopelvic fascia.
- The perineal body is a key fibromuscular node (injury can contribute to pelvic organ prolapse).
⚙️ Physiology
- Vaginal environment: usually acidic in reproductive years (typically pH ~3.8–4.5).
- Oestrogen effect: increases epithelial thickness and glycogen content.
- Lactobacilli metabolise glycogen → lactic acid → maintains acidity and inhibits pathogens.
- Lubrication: largely via plasma transudate during arousal plus cervical secretions; integrity depends on oestrogen and mucosal health.
- Mechanical roles: distensible canal allowing intercourse and childbirth; rugae and elastic tissue support expansion and recoil.
🔄 Changes Across the Lifespan
- Prepubertal: thin epithelium, neutral/alkaline pH, reduced lactobacilli → higher infection/irritation susceptibility.
- Reproductive years: oestrogenised thick mucosa, acidic pH, prominent rugae, robust microbiome.
- Postmenopausal: low oestrogen → thin fragile mucosa, reduced glycogen/lactobacilli, higher pH → dryness, dyspareunia, and vulnerability to inflammation/UTI symptoms (often termed GSM).
🩺 Clinical Correlates
- Speculum examination: uses the distensibility and fornices; posterior fornix relates to the pouch of Douglas (site for fluid collection).
- Infection defence: acidity and lactobacilli are central-antibiotics, semen (alkaline), bleeding, and low oestrogen can alter pH and microbiome.
- Trauma/bleeding: rich venous plexus + mucosal fragility in low oestrogen states can make bleeding more likely.
- Lymph drainage patterns help explain node involvement in malignancy and guide assessment.
🧠 Teaching Commentary (Makindo-style)
- Think of the vagina as a hormone-responsive, immunologically active mucosa: oestrogen thickens epithelium and loads it with glycogen, which “feeds” lactobacilli to maintain an acidic pH-this is a key reason infection patterns differ prepubertally and postmenopausally.
- The upper vs lower innervation split matters clinically: upper vagina pain is visceral (vague), while the lower third is pudendal (sharp/well localised), explaining why procedures at the introitus often need more targeted local anaesthesia.
- Remember there are no vaginal glands; most lubrication is transudate plus cervical/vestibular contributions-so low oestrogen states disproportionately cause dryness and microtrauma.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
