| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Chemosis
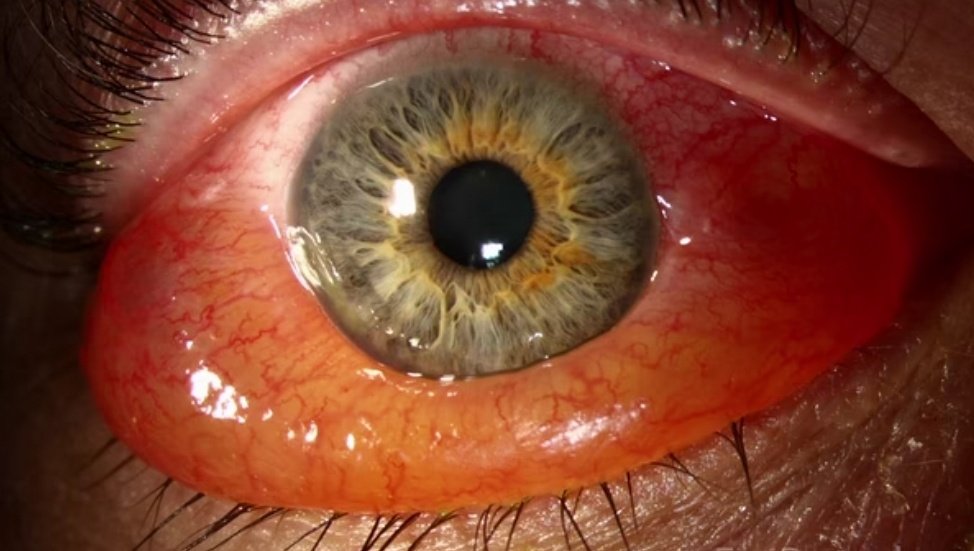
🧠 Chemosis = swelling/oedema of the conjunctiva (often looks like “jelly” or ballooning around the cornea). Pathophysiology is usually either ↑ vascular permeability (allergy/inflammation/infection) or venous/lymphatic congestion (orbital pressure, thyroid eye disease, impaired venous drainage). The key clinical skill is spotting the few dangerous causes where chemosis is a marker of orbital pathology rather than simple conjunctivitis.
✅ First assessment (always)
- 📌 Check vision (acuity), pupils (RAPD), and pain level.
- 👀 Look for proptosis, reduced eye movements, diplopia, corneal exposure, photophobia.
- 🌡️ Ask about fever, sinus symptoms, trauma/surgery, contact lenses, anaphylaxis symptoms.
- 🧪 If discharge: watery vs mucopurulent; consider fluorescein if pain/photophobia/contact lenses (corneal involvement).
🚨 Red flags (same-day urgent ophthalmology / ED)
- 🔻 Reduced visual acuity or RAPD
- 😖 Severe pain, marked photophobia, or headache
- 👁️🗨️ Proptosis, restricted eye movements, diplopia
- 🌡️ Fever/toxicity, sinusitis + eye signs (think orbital cellulitis)
- 🩸 Recent facial/orbital trauma or eye surgery (think retrobulbar haemorrhage)
- 🧪 Chemical splash / alkali injury
- 🦠 Copious purulent discharge + rapid swelling (think gonococcal infection)
🧩 Causes of chemosis
- 🌼 Allergic conjunctivitis (itching, watery discharge, lid swelling; often bilateral)
- 🦠 Viral conjunctivitis (gritty, watery, contagious; pre-auricular nodes)
- 🧫 Bacterial conjunctivitis (mucopurulent discharge, lids stuck; usually mild)
- 🦠 Chlamydial conjunctivitis (chronic redness/discharge; follicular changes)
- ☣️ Severe hyperacute conjunctivitis (e.g., gonococcal) - can cause dramatic chemosis
- 🧠 Orbital cellulitis / post-septal infection (chemosis + proptosis + painful/restricted EOM)
- 🩸 Trauma / post-op swelling; retrobulbar haemorrhage (time-critical vision threat)
- 🦋 Thyroid eye disease (exposure, lid retraction, proptosis; chemosis from congestion)
- 🧠 Venous outflow obstruction (e.g., cavernous sinus thrombosis, carotid–cavernous fistula, SVC obstruction)
- 😮💨 Angioedema/anaphylaxis (rapid onset lid/conjunctival swelling + systemic features)
- 🌙 Exposure/lagophthalmos (dryness + conjunctival oedema, especially overnight)
💊 Management (practical approach)
1) If red flags → urgent escalation
- 📞 Same-day ophthalmology/ED if any red flags (vision threat/orbital disease).
- 🧠 Suspected orbital cellulitis/CST: treat as emergency (IV antibiotics + imaging per local pathway).
- 🩸 Suspected retrobulbar haemorrhage: emergency decompression pathway (do not delay).
- 🧪 Chemical injury: immediate irrigation + urgent ophthalmology.
2) If uncomplicated (no red flags) → treat the common causes
🌼 Allergic chemosis
- 🧊 Cold compresses; avoid rubbing (rubbing worsens mast-cell mediator release).
- 💧 Lubricants (preservative-free artificial tears) regularly.
- 🧪 Topical antihistamine/mast-cell stabiliser drops (e.g., olopatadine/cromoglicate depending on local formulary).
- 💊 Oral non-sedating antihistamine if systemic allergy symptoms.
- 🧑⚕️ If severe/persistent: consider short supervised course topical steroid only with ophthalmology input (risk of HSV/glaucoma).
🦠 Viral conjunctivitis
- 💧 Lubricants + cold compresses; hygiene advice (handwashing, avoid sharing towels).
- 🚫 Avoid routine antibiotics (usually self-limiting).
- 🚩 If significant photophobia/pain or reduced vision: consider keratitis → urgent eye review.
🧫 Mild bacterial conjunctivitis
- 🧼 Lid hygiene, warm compress if crusting.
- 💊 Consider topical antibiotic if marked purulence, contact-lens wearer, or not improving (local formulary e.g., chloramphenicol).
- 🧴 Stop contact lenses until fully resolved; replace lenses/case to prevent reinfection.
🦠 Chlamydial / hyperacute (gonococcal) suspicion
- 📞 Same-day sexual health/ophthalmology advice.
- 💉 Gonococcal eye infection is an emergency (systemic therapy + urgent ophthalmology; corneal perforation risk).
🦋 Thyroid eye disease / exposure-related chemosis
- 💧 Aggressive lubrication (drops by day, ointment at night), consider taping lids closed overnight if exposure.
- 🚭 Smoking cessation (major modifiable risk factor for TED severity).
- 🧑⚕️ Refer to ophthalmology/TED service if proptosis, diplopia, pain, or corneal exposure.
🏠 Patient advice
- ✅ Seek urgent help if vision worsens, pain increases, new diplopia, or swelling rapidly progresses.
- 🧼 Avoid rubbing; wash hands; don’t share towels/makeup.
- 👓 Avoid contact lenses until symptoms fully settle.
🔑 Clinical pearl: chemosis is a sign, not a diagnosis. The “big divider” is whether there are features of orbital disease or vision compromise. If the eye is painful, proptosed, movement-limited, febrile, or vision is reduced, treat it as urgent until proven otherwise.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
