| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Chronic Kidney Disease (CKD) ✅
Related Subjects: |Metabolic acidosis |Lactic acidosis |Acute Kidney Injury (AKI) / Acute Renal Failure |Renal/Kidney Physiology |Chronic Kidney Disease (CKD) |Anaemia in Chronic Kidney Disease |Analgesic Nephropathy |Medullary Sponge kidney |IgA Nephropathy (Berger's disease) |HIV associated nephropathy (HIVAN) |Balkan endemic nephropathy (BEN) |Autosomal Dominant Polycystic kidney disease
📖 About (NICE-aligned)
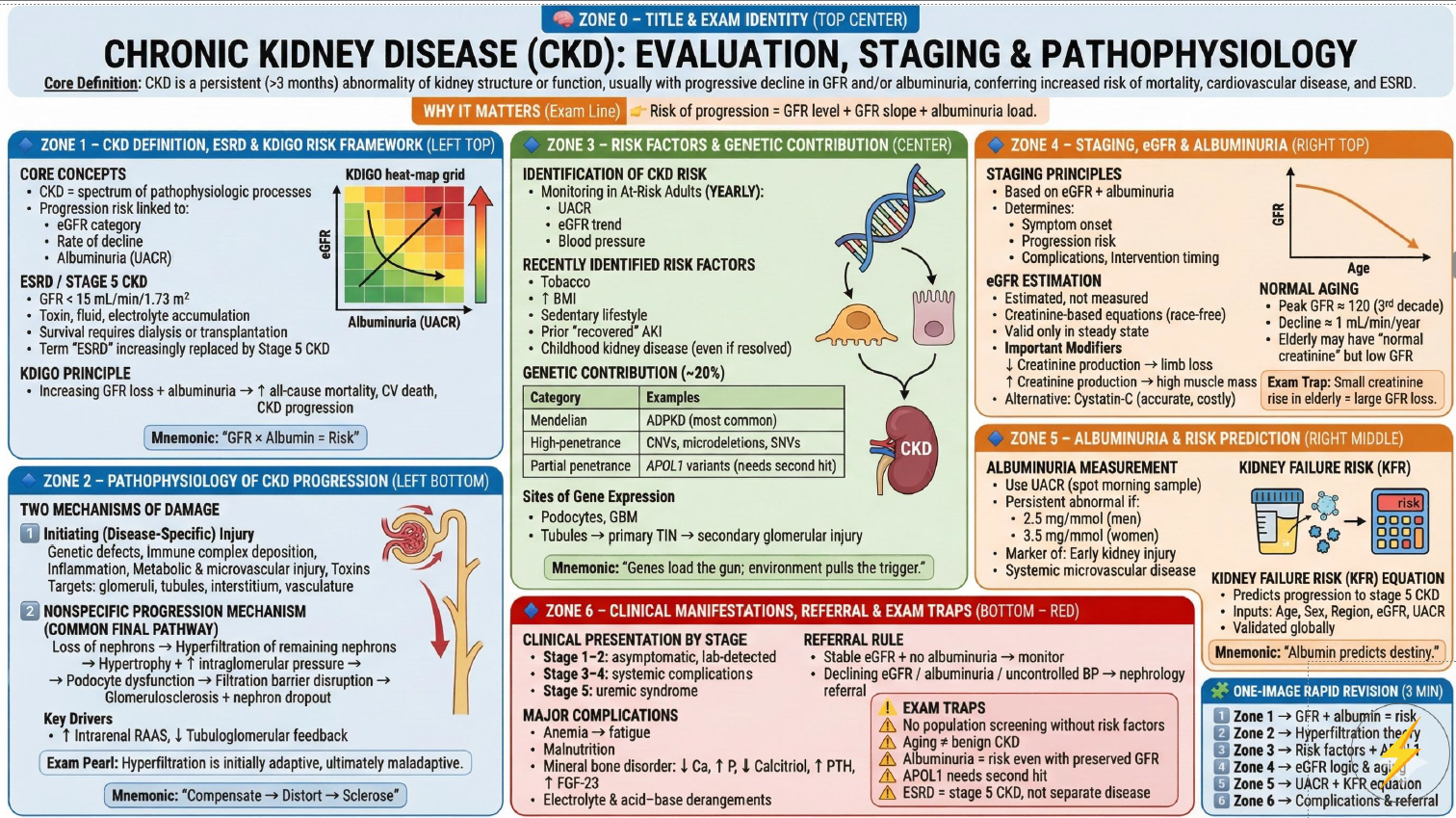
- Chronic Kidney Disease (CKD): abnormalities of kidney structure or function present for ≥3 months with implications for health.
- CKD includes: eGFR <60 mL/min/1.73m2 on ≥2 occasions ≥90 days apart (with or without markers), or markers of kidney damage (e.g. albuminuria, haematuria of renal origin, structural disease) even if eGFR is ≥60.
- Why it matters: increasing ACR and falling eGFR predict higher risk of CKD progression, AKI, and cardiovascular events.
📊 CKD Classification (use GFR + ACR)
- GFR categories (G):
- G1: ≥90 (CKD only if markers present)
- G2: 60–89 (CKD only if markers present)
- G3a: 45–59
- G3b: 30–44
- G4: 15–29
- G5: <15 (kidney failure)
- Albuminuria categories (A, by urine ACR):
- A1: <3 mg/mmol
- A2: 3–30 mg/mmol
- A3: >30 mg/mmol
🔖 Practical suffixes
- T = transplant recipient (e.g. CKD G3bA2T)
- D = dialysis (e.g. CKD G5D)
- Tip: NICE uses A1–A3 (ACR categories) rather than a “P” suffix; record the A category and the ACR value.
🧬 Aetiology (common)
- Diabetes mellitus
- Hypertension/vascular disease
- Glomerulonephritis.
- Polycystic kidney disease
- Reflux/tubulointerstitial disease
- Obstructive uropathy.
- Systemic disease (e.g. lupus, vasculitis)
- Medicines (e.g. NSAIDs, lithium)
- Myeloma (when suggested by phenotype).
🧠 Pathophysiology hook: falling eGFR reflects nephron loss; rising ACR reflects glomerular/endothelial injury. Albuminuria is a powerful “vascular damage” marker, so NICE stratifies BP targets and referral thresholds by ACR as well as GFR.
🧪 Diagnosis (NICE)
- Confirm chronicity: in a new reduced eGFR, repeat within 2 weeks to exclude AKI/acute deterioration; define progression using multiple readings over ≥90 days.
- Urine ACR: use ACR (more sensitive than PCR). If initial ACR 3–70, confirm on a repeat early-morning sample; no repeat needed if ACR ≥70.
- Urinalysis: haematuria/protein; consider renal-origin haematuria implications.
- Bloods: U&E/eGFR, potassium, bicarbonate, FBC, HbA1c (if diabetes), lipids; calcium/phosphate/PTH if advanced CKD or symptoms.
- Renal ultrasound if accelerated progression, persistent haematuria, obstruction symptoms, FHx ADPKD >20y, or eGFR <30 (G4–G5).
📉 Monitoring frequency (minimum eGFR checks per year – NICE Table 2)
- G1–G2: A1 = 0–1; A2 = 1; A3 = 1+
- G3a: A1 = 1; A2 = 1; A3 = 2
- G3b: A1 = 1–2; A2 = 2; A3 = 2+
- G4: A1 = 2; A2 = 2; A3 = 3
- G5: A1 = 4; A2 = 4+; A3 = 4+
- ACR monitoring: individualise based on risk and whether a change would alter management.
🎯 Blood pressure targets (NICE NG203)
- ACR <70 mg/mmol: aim clinic BP <140/90 (systolic target range 120–139).
- ACR ≥70 mg/mmol: aim clinic BP <130/80 (systolic target range 120–129).
- Frailty/multimorbidity: individualise (see NICE hypertension guidance).
💊 Proteinuria-lowering / kidney-protective therapy (NICE)
- Diabetes + ACR ≥3: offer ACEi or ARB titrated to the highest licensed tolerated dose.
- Hypertension + ACR >30 (A3): offer ACEi or ARB titrated to highest tolerated dose.
- No diabetes + ACR ≥70: refer and offer ACEi or ARB.
- RAAS safety: check eGFR and potassium before starting; repeat 1–2 weeks after starting and after each dose increase; avoid routine start if baseline K+ >5.0 mmol/L.
💔 CV risk reduction
- Statin: offer atorvastatin 20 mg as preferred initial high-intensity statin for people with CKD (unless contraindicated/not appropriate).
- Smoking cessation, exercise, weight and dietary salt reduction are core interventions.
- Antiplatelet therapy is for secondary prevention when indicated, balancing bleeding risk.
🩸 Anaemia of CKD (NICE)
- Investigate/manage if Hb ≤110 g/L (or symptomatic).
- Diagnostic clue: if eGFR >60, anaemia is unlikely due to CKD; if eGFR <30, CKD is often contributory but still consider other causes.
- ESA targets: do not correct to normal; typically maintain Hb 100–120 g/L in adults; avoid Hb >120 g/L (CV risk).
🦴 CKD-MBD / phosphate
- Monitor calcium/phosphate/PTH as CKD advances; manage persistent hyperphosphataemia (often in CKD 4–5) with diet and binders per local renal pathways.
🧯 Metabolic acidosis (NICE)
- Consider oral sodium bicarbonate if eGFR <30 (G4–G5) and serum bicarbonate <20 mmol/L.
🚑 When to refer (NICE NG203)
- KFRE: 5-year risk of needing RRT >5% (4-variable KFRE).
- ACR ≥70 mg/mmol (unless due to diabetes and already appropriately treated).
- ACR >30 with haematuria.
- Progression: sustained eGFR drop ≥25% with category change in 12 months, or ≥15 mL/min/1.73m2 per year.
- Resistant hypertension despite ≥4 agents, suspected genetic/rare CKD, suspected renal artery stenosis.
📚 References
- NICE NG203: Chronic kidney disease: assessment and management (Published 25 Aug 2021; last updated 24 Nov 2021)
- NICE NG203 Recommendations (BP targets, ACR confirmation, referral criteria, RAAS monitoring, anaemia, bicarbonate)
- NICE CKS: Chronic kidney disease
- NICE QS5: Statins for people with CKD (atorvastatin 20 mg)
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
