| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Psoriasis
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Psoriatic Arthritis |Psoriasis |Eczema/Dermatitis |Anatomy of Skin | Topical Steroids
🩺 Psoriasis = chronic, relapsing-remitting inflammatory skin disease. Characterised by well-demarcated erythematous plaques with silvery scales. Onset often 10–30 yrs. Significant morbidity due to disfigurement, itching, psychological impact, and risk of psoriatic arthritis.
📖 About
- Definition: Autoimmune condition with accelerated epidermal turnover → thick scaly plaques.
- Pathophysiology: Keratinocyte maturation shortened from 21–28 days to ~7 days.
- Associated: Psoriatic arthropathy (dactylitis, sacroiliitis, arthritis).
🧪 Aetiology
- 👫 Affects males & females equally.
- 🧬 Genetic predisposition + family history.
- 🛡️ Immunological: T-cell mediated, chronic inflammation.
- 🧱 Pathological: keratinocyte proliferation, angiogenesis.
- ⚡ Triggers: stress, infections, trauma (Koebner phenomenon), smoking, alcohol, certain drugs (β-blockers, lithium, NSAIDs, antimalarials).
📌 Types of Psoriasis
- 🟥 Chronic plaque psoriasis: Most common. Extensor plaques with silvery scale.
- 💧 Guttate psoriasis: “Raindrop” lesions post-streptococcal infection in young patients.
- 🟡 Seborrhoeic psoriasis: Affects nasolabial folds, scalp, retroauricular areas.
- 🔄 Flexural (inverse): Shiny red lesions in body folds (axillae, inframammary).
- 🔥 Erythrodermic psoriasis: Rare, life-threatening, widespread erythema/scaling → admit.
- 👣 Palmar-plantar pustulosis: Sterile pustules on palms/soles.
⚡ Clinical Features
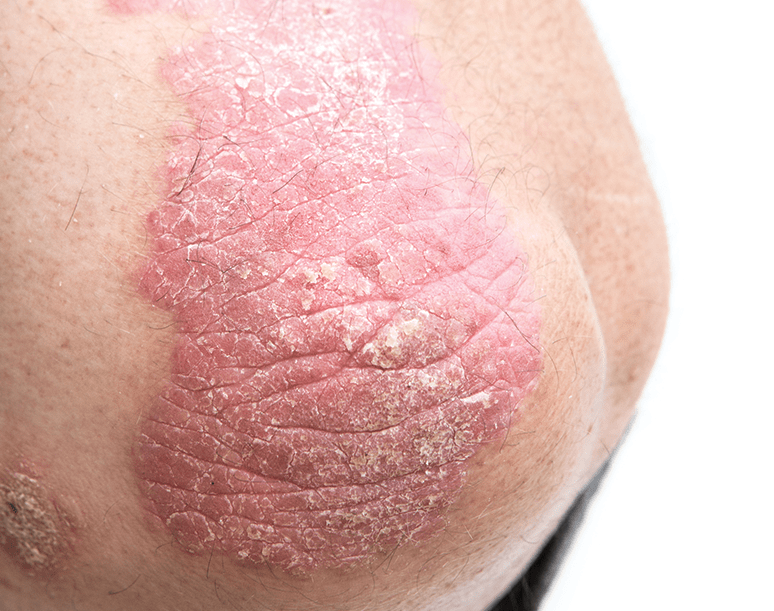
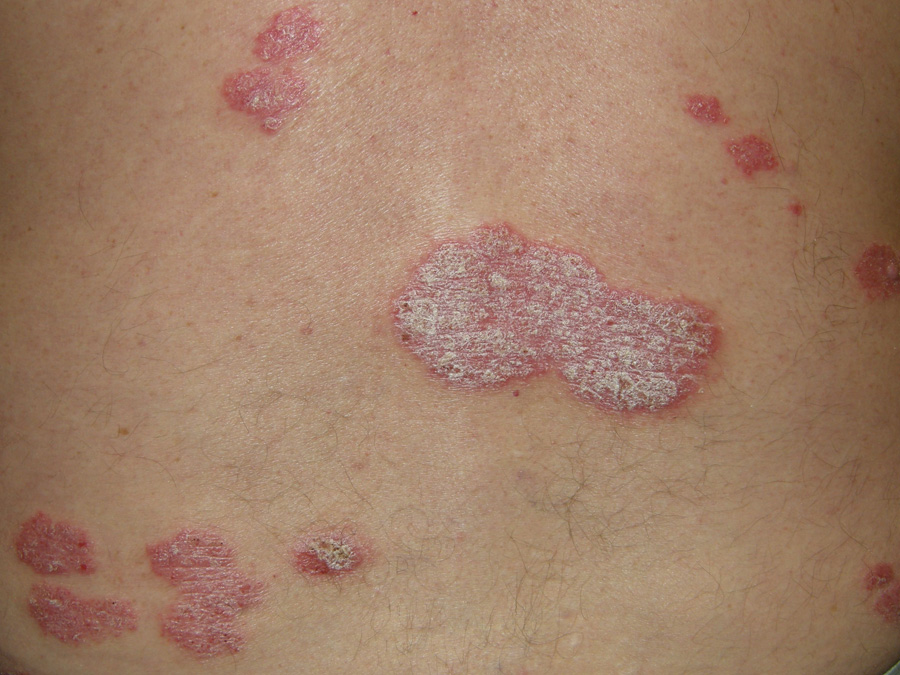
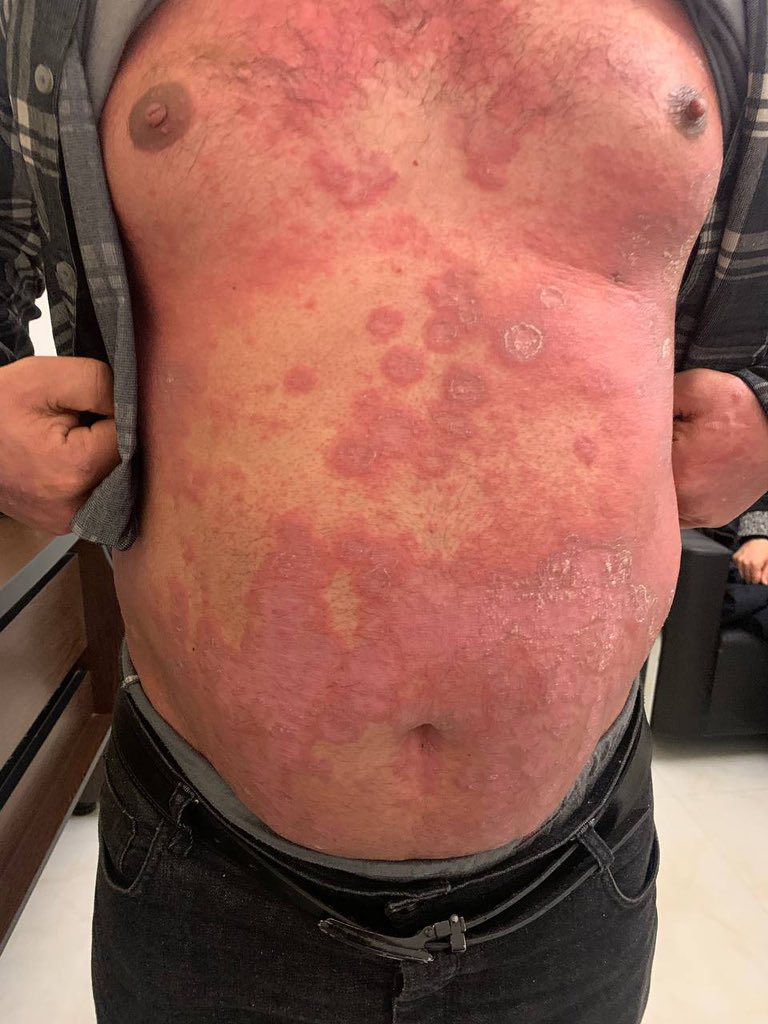
- Red plaques, silvery scales (classically elbows, knees, scalp, lumbosacral area).
- Koebner phenomenon: new lesions at trauma sites.
- Scalp: thick adherent plaques.
- Nails: pitting, onycholysis, “oil drop” sign.
- Pustules (localized/generalized).
- Erythrodermic psoriasis → urgent review.
🔀 Differential Diagnosis
- Pityriasis rosea vs guttate psoriasis.
- Scalp psoriasis vs seborrhoeic dermatitis (dandruff).
- Chronic eczema vs flexural psoriasis.
🔎 Investigations
- Usually clinical diagnosis.
- Skin biopsy if atypical.
- Screen for comorbidities: metabolic syndrome, diabetes, cardiovascular disease.
💊 Management
- 👩⚕️ Referral: To dermatology if diagnosis uncertain, extensive disease, occupational impact, face/palm/genital involvement, poor response to 2–3 months of topicals, severe/recalcitrant cases, or suspected psoriatic arthritis → rheumatology.
🧴 Topical Therapies
- 💧 Emollients: 3–4× daily. Reduce scaling, itching.
- 🧪 Vitamin D analogues: Calcipotriol, tacalcitol, calcitriol. Often first-line with/without steroids.
- 💊 Topical corticosteroids: Useful for plaques, scalp, flexures (short-term).
- 🟤 Coal tar: Anti-inflammatory, odorous but effective. Can combine with salicylic acid for scaling.
- 🟣 Dithranol: For large plaques. Effective but irritant, stains skin.
- 🧴 Topical retinoids (tazarotene): Mild–moderate plaque psoriasis.
- 🧠 Psychological support: Important given stigma and mental health impact.
- 📅 Follow-up at 6 weeks to assess efficacy/adherence (SIGN 122).
🔆 Special Topical Guidance
- 🧴 Scalp psoriasis: Potent corticosteroid short-term ± vitamin D analogue (SIGN 121).
- 🔄 Flexural psoriasis: Moderate steroids short-term. Alternatives: tacrolimus, vitamin D analogues.
🌞 Phototherapy & Systemic Therapies
- 🌞 Phototherapy: Narrow-band UVB for widespread guttate or resistant psoriasis.
- 💊 Oral retinoids: Acitretin for severe disease.
- 🛡️ Immunosuppressants: Ciclosporin, methotrexate, mycophenolate.
- 🧬 Biologics: Infliximab, etanercept, adalimumab, ustekinumab for severe refractory psoriasis.
- ⚠️ Systemic corticosteroids: Reserved for emergency pustular/erythrodermic cases → risk of rebound flare.
📈 Prognosis
- Chronic, relapsing condition with variable severity.
- Good control possible with modern therapies.
- Important to monitor for psoriatic arthritis + metabolic/cardiovascular comorbidities.
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
