| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Coronary: Percutaneous Coronary Intervention
Related Subjects: |Atherosclerosis |Ischaemic heart disease |Assessing Chest Pain |ACS - General |ACS - STEMI |ACS - NSTEMI |ACS - GRACE Score |ACS - ECG Changes |ACS -Cardiac Troponins |ACS - Post MI arrhythmias |ACS: Right Ventricular Infarction
⚠️ Always consult cardiology before discontinuing antiplatelet therapy after stent insertion. 🚫 Stopping clopidogrel or other antiplatelets too early (especially with drug-eluting stents) risks catastrophic in-stent thrombosis. 🕐 Standard practice: Dual Antiplatelet Therapy (DAPT) - aspirin + clopidogrel/ticagrelor/prasugrel - for 6–12 months, with aspirin often lifelong. 👉 Local / guideline variations exist, so confirm with the cardiology team.
ℹ️ About
- PCI (Percutaneous Coronary Intervention): Opens blocked coronary arteries using balloons and stents to restore perfusion. Improves angina symptoms and quality of life, though elective PCI does not significantly reduce overall mortality.
- Originally developed to select candidates for CABG, PCI is now a primary treatment for many acute coronary syndromes (ACS).
- Widespread catheterization labs, even in district hospitals, allow rapid reperfusion without immediate need for cardiac surgery backup.
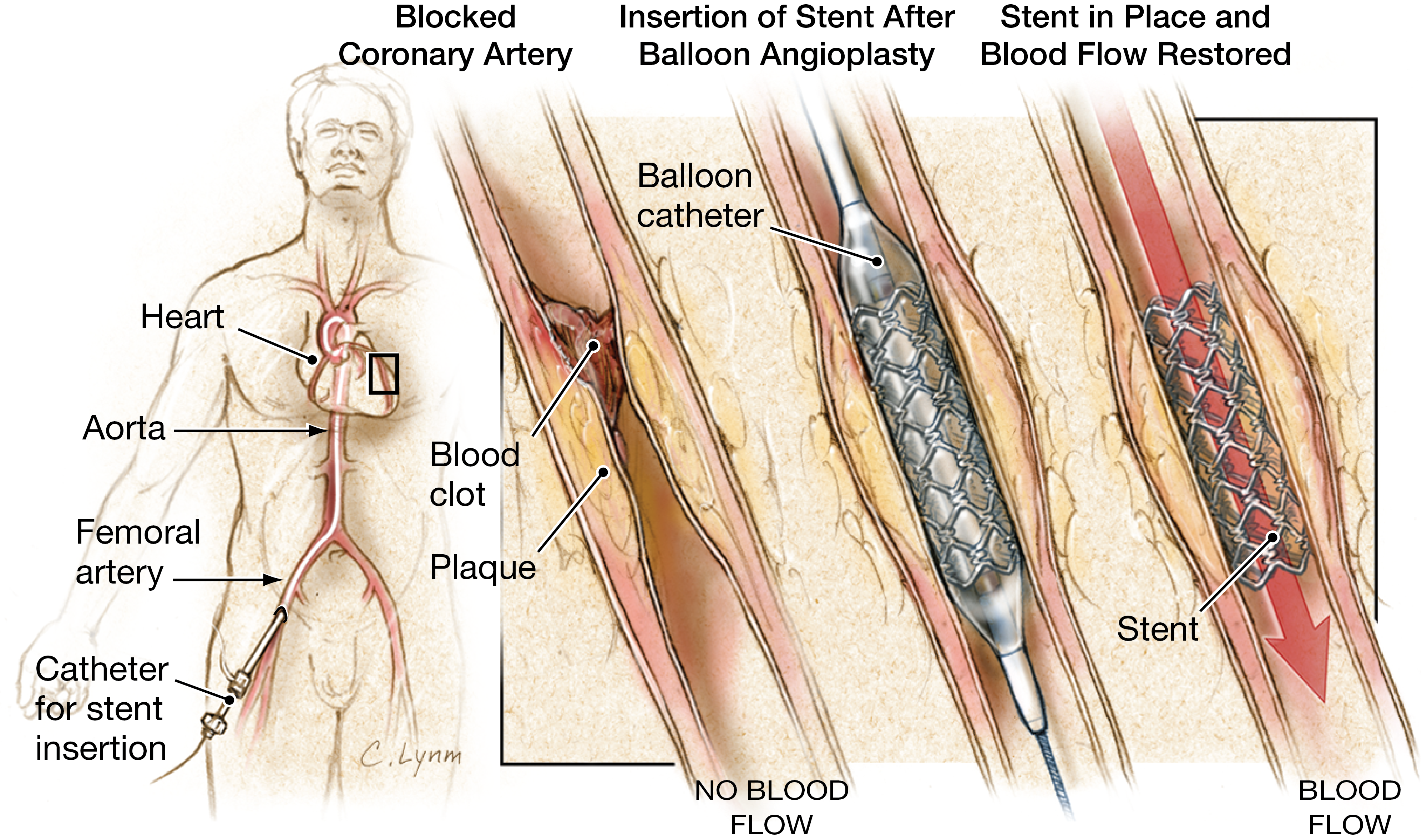
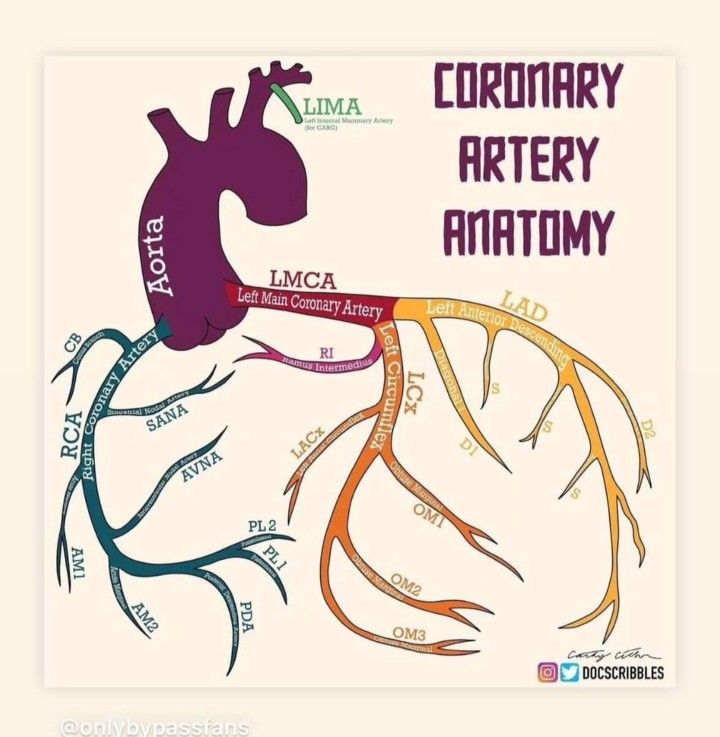
🧩 Stents
- 🛠️ Stents = metallic scaffolds to keep an artery open after balloon angioplasty.
- 🚑 Deployed via femoral or radial approach using guidewires and balloons under fluoroscopy.
- 💊 Drug-Eluting Stents (DES): Coated with antiproliferative drugs (e.g., sirolimus, paclitaxel) to reduce restenosis risk. Preferred in diabetics and complex lesions.
- ⚡ Difficult lesions: Long, calcified, eccentric, bifurcation, thrombotic, or tortuous arteries.
- 🩸 DAPT: Almost all patients receive aspirin + clopidogrel (or ticagrelor/prasugrel) for 6–12 months after PCI.
🏥 Indications (Mortality Benefit)
- 🚨 STEMI: Primary PCI within 90 minutes of first medical contact.
- 🚑 STEMI with hemodynamic compromise or failed thrombolysis.
- ⚡ STEMI in thrombolysis-contraindicated patients (e.g., recent intracranial hemorrhage).
📋 Other Indications
- High-risk NSTEMI.
- Unstable angina with high-risk features.
- Unexplained ischemic cardiomyopathy.
- Survivors of cardiac arrest where ischemia is suspected.
- Significant ventricular arrhythmias (VT) due to ischemic substrate.
🔍 Vascular Access
- Common sites: Radial artery (preferred for lower bleeding risk), femoral artery, or brachial artery.
📝 Protocol
- 🖊️ Consent: Mortality risk ~0.1% for diagnostic angiography, higher with PCI complexity.
- 🩸 Pre-procedure checks: FBC, platelets, U&Es, renal function, glucose, and peripheral pulses.
- 💊 Consider acetylcysteine in renal impairment (contrast nephropathy prevention - though evidence is mixed).
- 🚫 Fast for 6 hours, continue aspirin, load clopidogrel/ticagrelor as advised.
⚙️ Interventions
- 🎈 Balloon Angioplasty: Rarely used alone; risk of restenosis high.
- 🧱 Bare Metal Stents (BMS): Reduce restenosis vs balloon, but higher thrombosis risk. Shorter DAPT course than DES.
- 💊 Drug-Eluting Stents (DES): Reduce neointimal hyperplasia and restenosis; require longer DAPT.
- 🔀 Referral for CABG: Triple-vessel disease or significant left main stem involvement.
⚠️ Post-Procedure Complications
- 💉 Bleeding: At access site or retroperitoneal (suspect if hypotension + tachycardia).
- 🦵 Limb Ischemia: Cold, pale leg from thrombosis or dissection → urgent vascular review.
- 📈 Acute Stent Thrombosis: Presents like STEMI → urgent repeat PCI.
- 💧 Contrast Nephropathy: Monitor U&Es, hydrate well.
- 🧠 Stroke: Rare but serious embolic complication.
- 🦠 Infection / pseudoaneurysm / AV fistula: At puncture site, confirmed by ultrasound.
📚 Exam Tip: 👉 Always mention DAPT duration when discussing PCI. 👉 Drug-eluting stents reduce restenosis but require longer antiplatelet therapy. 👉 Radial access = fewer bleeding complications vs femoral.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
