| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Herpes Varicella-Zoster (Shingles) Infection
Related Subjects: |Herpes Varicella-Zoster (Shingles) Infection |Chickenpox Varicella Infection |Varicella Cerebral Vasculopathy |Analgesia and Pain management |Sedation and Analgesia on ITU |Neuropathic Pain Management
💉 The national vaccination campaign recommends immunisation in adults over 70 to prevent shingles and postherpetic neuralgia. 👁️ Also see related topics on Herpes Zoster Ophthalmicus and Varicella (chickenpox).
📖 About
- 🔬 Herpes viruses are double-stranded DNA viruses.
- 🌬️ Spread by droplet transmission → highly contagious.
- 🧒 Most people gain immunity in childhood, but virus may reactivate later in life → shingles.
- 🎯 Targets the skin, eyes, and nervous system.
🦠 Virology
- Varicella → chickenpox; Zoster → shingles.
- ⏳ Incubation: 10–21 days.
- 🧠 Virus remains latent in dorsal root ganglia or cranial nerve nuclei.
🩹 Shingles
Characteristic belt-like rash, unilateral, confined to a single dermatome.
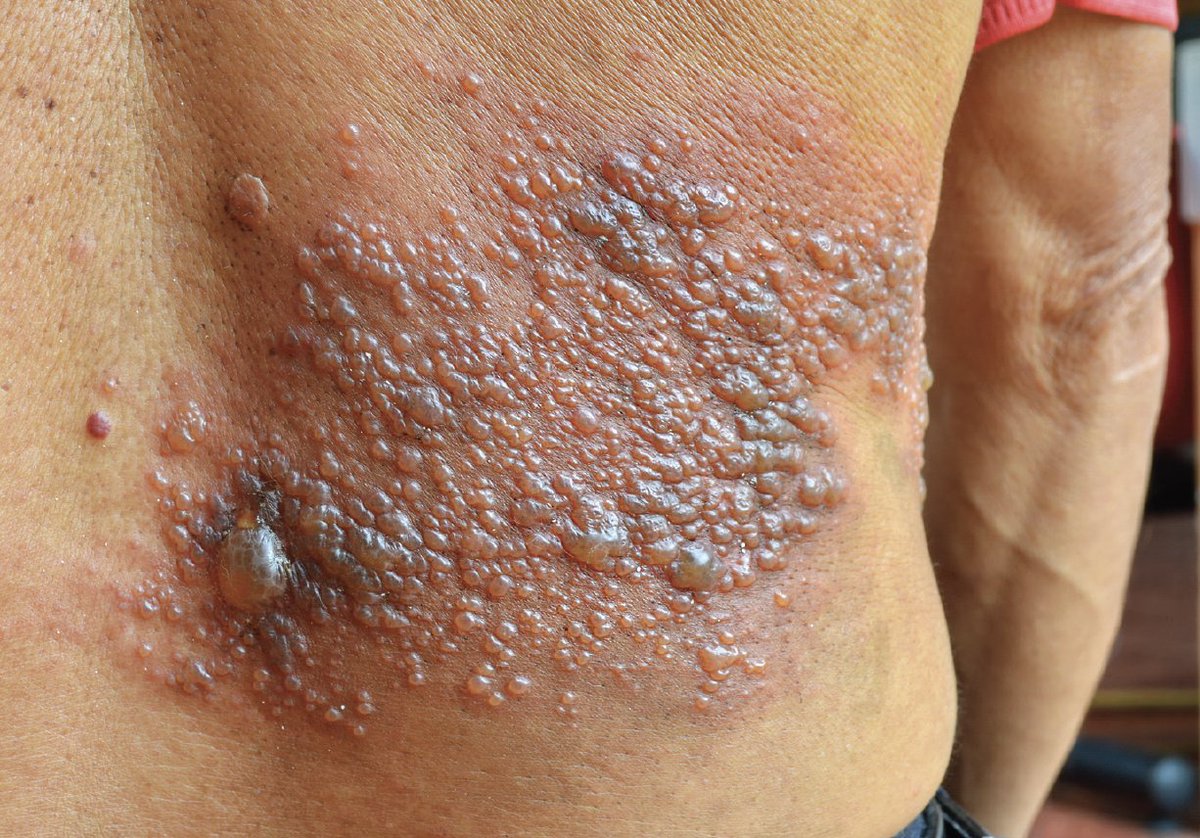
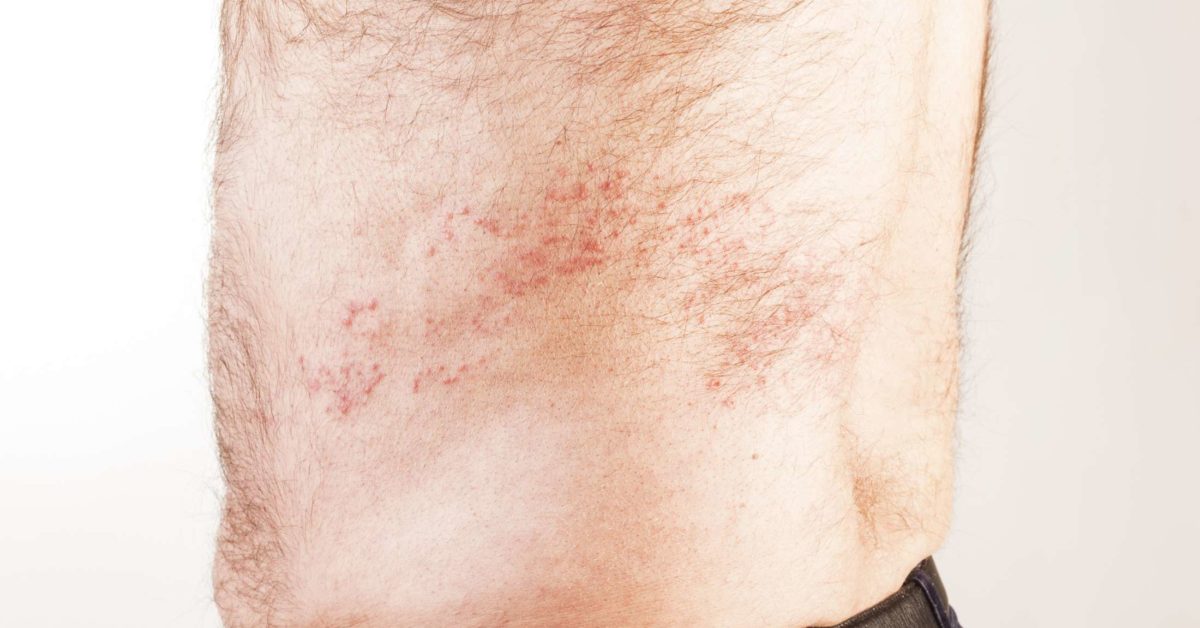
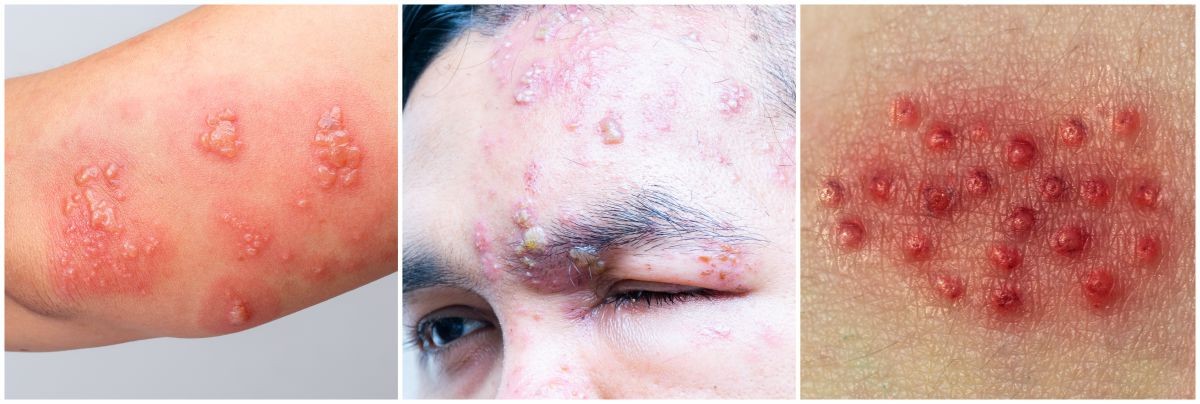
⚠️ Severe, extensive, or prolonged disease should raise suspicion for immunosuppression (e.g., HIV). 👉 Chickenpox can be caught from shingles, but not the other way around.
🩺 Clinical Presentation
- 🔥 Sharp, burning pain precedes rash (typically 2–3 days).
- 🌡️ Fever, malaise, itching, tingling.
- 🩹 Rash: grouped vesicles on erythematous base, confined to dermatome.
- 👶 Children: chickenpox → crops of vesicular lesions + fever.
- 👨 Adults: higher morbidity/mortality (15× that of children).
- 🤰 Pregnancy: risk of varicella pneumonitis.
- 🧠 Complications: pneumonitis, encephalitis (20% fatality), hepatitis, thrombocytopenia.
🔎 Other Manifestations
- ⚡ Postherpetic neuralgia: persistent neuropathic pain.
- 👁️ Herpes Zoster Ophthalmicus: corneal involvement (ophthalmic branch of CN V).
- 👂 Ramsay Hunt syndrome: facial palsy + vesicles in ear canal.
- 🧠 Neurological: transverse myelitis, Guillain-Barré syndrome, stroke syndromes (zoster vasculitis).
🚬 Risks for Varicella Pneumonia
- Smoking
- Pregnancy
- Immunosuppression
- Male sex
🧑⚕️ Immunocompromised Patients
- 💥 More severe, widespread, or prolonged disease.
- High-risk groups: HIV (low CD4), transplant recipients, patients on steroids/azathioprine/TNF antagonists, malignancy, pregnancy.
🧪 Investigations
- 🩸 Baseline bloods: FBC, U&E, LFT, CRP.
- 🧫 Vesicle fluid: PCR, EM, fluorescent antibody test.
- 🔍 Assess for immunodeficiency or cancer red flags.
🛠️ Primary Care Management
- 💊 Start oral antiviral within 72 h: e.g., Aciclovir 800 mg 5× daily × 7 days.
- 💡 Provide analgesia: paracetamol ± codeine; consider amitriptyline/gabapentin if neuropathic pain.
- 👕 Keep rash covered; avoid contact with non-immune, pregnant, or immunocompromised individuals until crusted over.
- 🗣️ Reassure: usually self-limiting but risk of postherpetic neuralgia.
- 📅 Follow-up if pain >4 weeks or rash becomes widespread (screen for immunosuppression).
- 💉 Discuss zoster vaccination for future prevention (if not already given).
🏥 Hospital Management
- 🚪 Isolate; only immune staff should provide care.
- 💊 Antivirals (start ≤72h of rash):
- Aciclovir 800 mg 5× daily × 7 days
- Famciclovir 500 mg tds × 7 days
- Valaciclovir 1 g tds × 7 days
- 🧑⚕️ Immunocompromised: same drugs but longer course (continue 2 days post-crusting).
- 💊 Pain relief: paracetamol, codeine ± neuropathic agents.
- 👩⚕️ Pregnant/breastfeeding: consult microbiology before antivirals.
⚡ Postherpetic Neuralgia
- Chronic neuropathic pain after shingles.
- ⬆️ Risk with age and severe acute pain.
- Options: amitriptyline, gabapentin, duloxetine, topical capsaicin, lidocaine patches.
- Tramadol: short-term rescue only (avoid long-term).
🛡️ Prevention
- 💉 National shingles vaccine ≥70 yrs to reduce incidence and neuralgia.
- 👩🍼 Exposed non-immune pregnant/immunocompromised → Zoster Immunoglobulin (ZIG) within 10 days.
- 💊 If infection develops → treat with aciclovir; seek microbiology advice.
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
