| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
EEG (Electroencephalogram)
🧠 An Electroencephalogram (EEG) is a non-invasive test that records electrical activity in the brain via scalp electrodes. It provides a real-time picture of brain function and is particularly useful for detecting abnormalities such as seizures, sleep disorders, and encephalopathies. EEG is safe, painless, and remains a cornerstone of neurological diagnosis.
✨ Uses of EEG
- ⚡ Seizure Disorders: The most common use ➝ helps diagnose epilepsy and classify seizure types by identifying abnormal discharges (spikes, sharp waves).
- 😴 Sleep Disorders: Assists in diagnosing narcolepsy, sleep apnea, and parasomnias. Can also map normal sleep stages.
- 🧀 Brain Tumors & Structural Lesions: Detects focal slowing near lesions or mass effect.
- 🤕 Head Injuries: Evaluates functional impairment post-trauma, especially in diffuse brain injury.
- 🧪 Encephalopathy: Metabolic or toxic encephalopathies produce global slowing of EEG activity.
- 🔪 Intraoperative Monitoring: Used during neurosurgery or vascular surgery to monitor cortical activity and prevent ischemia.
- 💤 Coma & Brain Death Evaluation: EEG can show low-amplitude slow waves in coma or a flatline pattern in brain death (with clinical correlation).
⚙️ How EEG is Done
- 🧼 Preparation: Avoid caffeine/medications that alter brain activity. The scalp is cleaned; electrodes applied with conductive gel.
- 🎯 Electrode Placement: Usually 16–25 electrodes placed using the 10–20 system. They record regional brain activity.
- 📊 Recording: Patient relaxes, often asked to close eyes. Provocative maneuvers like hyperventilation or photic stimulation (flashing lights) may be added to trigger abnormalities.
- ⏱️ Duration: Routine EEG lasts 20–40 minutes. Prolonged/ambulatory EEGs (24–72 hrs) increase diagnostic yield, especially for intermittent seizures.
- ✅ Post-Test: Electrodes are removed; no recovery period needed. A neurologist interprets the traces.
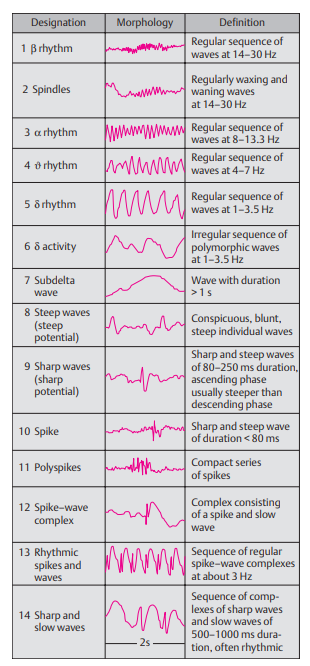
📈 Interpretation of EEG Results
- ✅ Normal Brain Waves:
- Alpha waves (8–12 Hz): Relaxed, awake state (posterior head regions).
- Beta waves (13–30 Hz): Alert, active thinking.
- Theta (4–7 Hz) & Delta (<4 Hz): Normal in sleep, abnormal in awake adults.
- ⚠️ Abnormal Brain Waves:
- Epileptic Seizures: Sharp spikes, spike-and-wave complexes (classic 3 Hz in absence seizures).
- Brain Tumors/Lesions: Focal slowing near lesion sites.
- Sleep Disorders: Altered sleep spindles or disrupted architecture.
- Coma/Brain Death: Low-voltage slow activity in coma; flatline in brain death (must be confirmed with repeat studies + clinical assessment).
- 💡 Clinical Relevance: EEG patterns alone are rarely diagnostic ➝ they must be interpreted alongside history, clinical exam, and imaging (MRI/CT).
📌 Teaching Pearl: A normal EEG does not exclude epilepsy ❗ Abnormalities may only appear during seizures, so prolonged monitoring or video-EEG telemetry is often required.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
