| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Prostate cancer✅
Related Subjects: | Urothelial Tumours | Haematuria | Acute Urinary Retention | Anuria and Oliguria | Bladder Cancer |Penile Cancer | Renal Cell Carcinoma | Benign Prostatic Hyperplasia | IgA Nephropathy | Prostate Cancer | Henoch-Schonlein Purpura | Glomerulonephritis
🧪 PSA (Prostate-Specific Antigen) is a protein produced by epithelial cells of the prostate gland. ⚗️ It is a 34 kDa serine protease glycoprotein that helps liquefy semen.
- 📈 PSA can rise in prostate cancer, benign prostatic hyperplasia (BPH), prostatitis, urinary retention, and increasing age.
- ⏱️ PSA velocity refers to the rate of PSA change over time and may suggest malignancy if rapidly rising.
- 🦴 Very high PSA levels (often >100 ng/mL) strongly suggest metastatic disease, particularly bone metastases.
- ✋ Digital rectal examination (DRE) does not significantly elevate PSA.
- ⚠️ PSA is not cancer-specific; interpretation requires clinical context.
📌 About Prostate Cancer
- 🧓 Most common cancer in men in the UK.
- 📈 Incidence increases sharply with age.
- 🔍 Many tumours are slow growing and may never cause symptoms.
- ⚖️ The clinical challenge is balancing early detection with avoiding overtreatment.
- 💉 Tumour growth is typically androgen-dependent (driven by testosterone).
📊 Epidemiology
- 🇬🇧 Around 52,000 new cases per year in the UK.
- 👨 Rare before age 50.
- 🏿 Risk is significantly higher in Black African and Caribbean men.
- 👨👦 Family history increases risk (≈2–3×).
- ⚖️ Obesity and smoking are associated with more aggressive disease.
🧫 Pathology
- 🧬 ~95% are acinar adenocarcinomas arising from glandular epithelium.
- 📍 Most tumours arise in the peripheral zone of the prostate.
- 🧪 Prostatic intraepithelial neoplasia (PIN) is a recognised precursor lesion.
- 🧬 Tumour aggressiveness is graded using the Gleason scoring system.
🩺 Clinical Presentation
- 💧 Lower urinary tract symptoms (LUTS) frequency, nocturia, weak stream, hesitancy
- 🩸 Haematuria or haematospermia
- 🦴 Bone pain → may indicate metastatic disease
- ⚠️ Many patients are asymptomatic at diagnosis
🧩 Common Clinical Findings
- 📈 Raised PSA on blood testing
- ✋ DRE findings: hard, irregular or nodular prostate
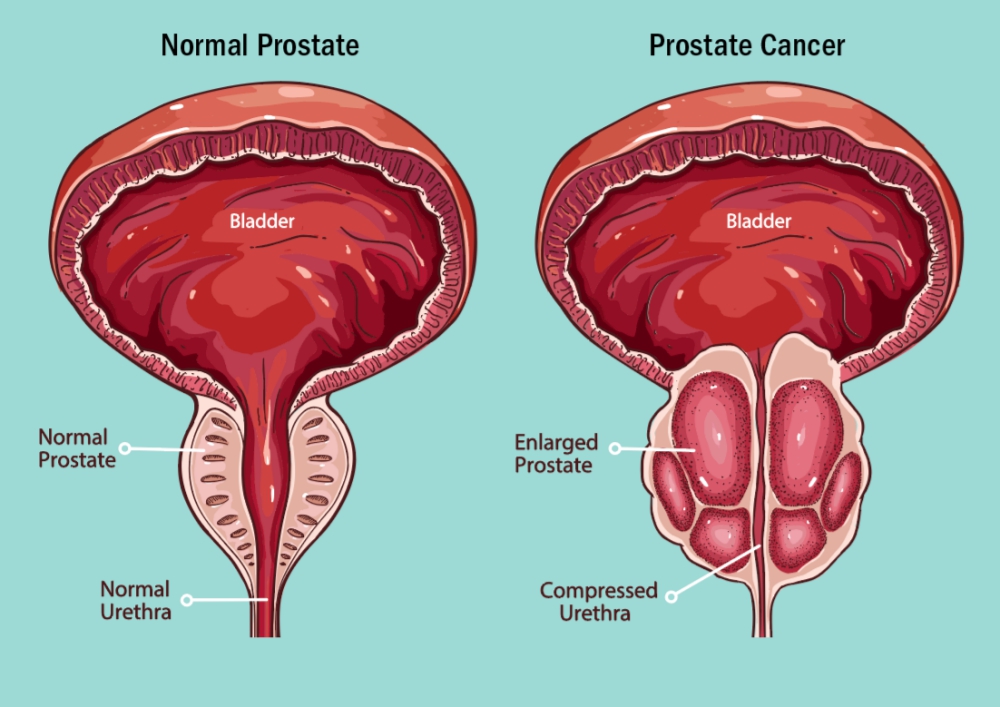
- 🚽 Bladder outflow obstruction → possible renal impairment
- 🦴 Osteosclerotic bone metastases causing pain or pathological fracture
📐 PSA Reference Ranges (Age-Adjusted)
- 👨 40–49 yrs: <2.5 ng/mL
- 👨 50–59 yrs: <3.5 ng/mL
- 👨 60–69 yrs: <4.5 ng/mL
- 👨 ≥70 yrs: <6.5 ng/mL
- 📊 PSA 4–10 ng/mL → cancer risk ≈25%
- 📊 PSA >10 ng/mL → higher risk of malignancy
🔍 Investigations
- 🩸 Blood tests: U&E, FBC, ALP (may rise with bone metastases)
- 📡 Multiparametric MRI (mpMRI) is now performed before biopsy in suspected prostate cancer.
- 🧪 Targeted prostate biopsy (usually transperineal) guided by MRI findings.
- 📊 Gleason score / Grade Group used to determine tumour aggressiveness.
- 🦴 Bone scan or PSMA-PET if high PSA, high Gleason score, or symptoms suggesting metastases.
📊 Risk Stratification (Localised Disease)
| Risk Level | PSA | Gleason Score | Clinical Stage |
|---|---|---|---|
| Low | <10 | ≤6 | T1–T2a |
| Intermediate | 10–20 | 7 | T2b |
| High | >20 | 8–10 | ≥T2c |
🛠️ Management (UK Practice – NICE NG131)
📌 Initial Assessment
- Risk stratification using PSA, MRI findings, Gleason score, and stage.
- All cases discussed at specialist multidisciplinary team (MDT).
🏥 Localised Disease (T1–T2)
Low-risk disease- 👀 Active surveillance is often preferred.
- Definitive treatment if progression occurs.
- 🔪 Radical prostatectomy
- 🎯 External beam radiotherapy ± short-course androgen deprivation therapy
- ⚡ Brachytherapy in selected patients
- 🎯 Radiotherapy + long-term androgen deprivation therapy (ADT)
- 🔪 Surgery considered in selected patients in specialist centres
📍 Locally Advanced Disease (T3–T4)
- 🎯 External beam radiotherapy + long-term ADT
- Multimodal treatment often required
🌍 Metastatic Disease
Hormone-sensitive metastatic disease- 💉 Androgen deprivation therapy (ADT) (LHRH agonist or antagonist)
- ➕ Treatment intensification with docetaxel, abiraterone, enzalutamide, or apalutamide
- Continue ADT
- ➕ novel hormonal therapies or chemotherapy
- 🦴 Radium-223 for symptomatic bone metastases
- 🧬 PARP inhibitors (e.g. olaparib) for BRCA-mutated cancers
🤝 Supportive Care
- 🦴 Bone protection: bisphosphonates or denosumab
- 💪 Manage ADT complications (osteoporosis, metabolic syndrome, fatigue)
- 🎯 Palliative radiotherapy for painful bone metastases
🇬🇧 UK Practice Points
- Follow NICE NG131 guidance.
- mpMRI is recommended before biopsy.
- All treatment decisions made via MDT discussion.
- 📊 Long-term PSA monitoring after treatment is essential.
🩺 Case 1 – Low-risk Prostate Cancer
A 62-year-old man has PSA 6.1 ng/mL detected in primary care. MRI shows a small PIRADS-3 lesion and biopsy confirms Gleason 3+3 disease. Management: Active surveillance with regular PSA monitoring, MRI follow-up, and repeat biopsy if disease progression is suspected.
🩺 Case 2 – Intermediate-risk Disease
A 68-year-old man presents with PSA 12.8 ng/mL and MRI showing a PIRADS-5 lesion. Biopsy confirms Gleason 4+3 cancer. Management: Radical prostatectomy or external beam radiotherapy with short-term androgen deprivation therapy.
🩺 Case 3 – Metastatic Prostate Cancer
A 74-year-old man presents with back pain and PSA 186 ng/mL. Imaging confirms multiple bone metastases. Management: Androgen deprivation therapy combined with systemic therapy (e.g. abiraterone or docetaxel), with palliative radiotherapy for symptomatic bone metastases.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
