| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Anomalous Coronary Arteries
Related Subjects: |Brugada Syndrome |Long QT syndrome (LQTS) Acquired |Long QT syndrome (LQTS) Congenital |Torsades de Pointes |Ventricular Fibrillation |Ventricular Tachycardia |Resuscitation - Adult Tachycardia Algorithm |Automatic Implantable Cardioverter Defibrillator (AICD)
ℹ️ About Anomalous Coronary Arteries
- Rare congenital variants affecting coronary origin or course.
- Most are harmless incidental findings, but certain subtypes carry risk of myocardial ischemia or sudden death.
- High-risk features include interarterial course (between aorta and pulmonary artery), intramural segment, slit-like ostium, acute take-off angle, or proximal narrowing - these can cause compression during exercise.
📊 Incidence & Epidemiology
These anomalies are uncommon but increasingly detected thanks to advanced imaging. Prevalence varies by detection method and anomaly type.
- Overall Prevalence: ~0.3–1.3% in angiography/CT studies; up to 1–5.6% in some reports; higher in autopsy/specialized imaging (many asymptomatic cases undetected).
- Age & Gender: ALCAPA often presents in infancy with severe symptoms; anomalous origin from opposite sinus (e.g., right from left) may appear in adolescence/adulthood. Slight male predominance in some high-risk types linked to sudden events.
- Sudden Death Risk: Major cause of sudden cardiac death in young athletes (<35 years); highest with interarterial course (especially left from right sinus); right from left sinus also risky but lower than left anomalies.
- Detection Trends: Rising due to CT coronary angiography (CCTA), MRI, and awareness; key in screening athletes or symptomatic young people.
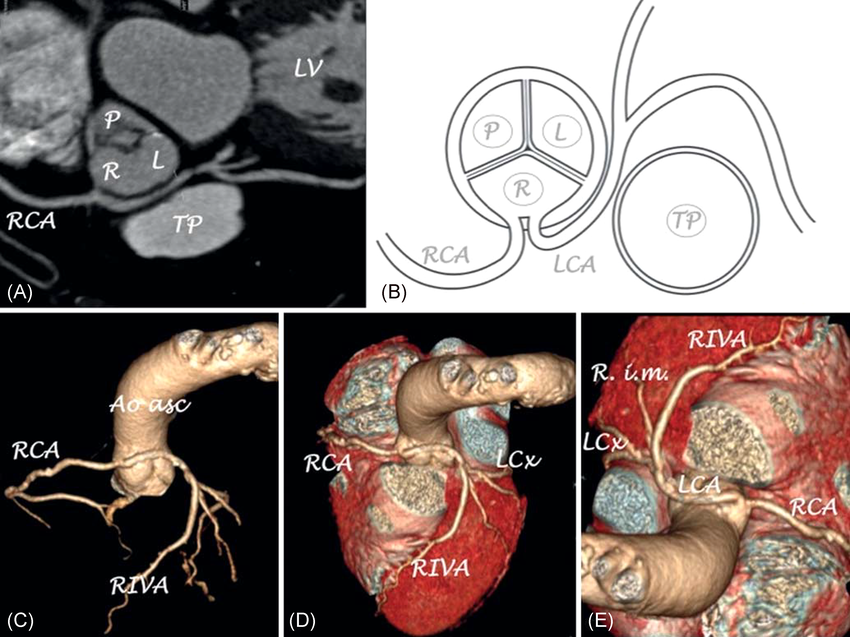
🔍 Main Types of Anomalous Coronary Arteries
| Type | Description | Risk Level | Key Notes |
|---|---|---|---|
| ALCAPA
(Anomalous Left Coronary Artery from Pulmonary Artery) |
Left coronary arises from pulmonary artery instead of aorta. | High (malignant in infancy) | Infants: heart failure, ischemia; surgery essential early. Rare in adults if survived untreated. |
| Anomalous Right Coronary Artery from Left Sinus
(R-AAOCA/ARCA) |
RCA originates from left sinus; often interarterial course. | Moderate–High | Common high-risk type; compression risk during exercise; sudden death link. |
| Anomalous Left Coronary Artery from Right Sinus
(L-AAOCA) |
Left (or left main) from right sinus; interarterial common. | Very High | Strongest SCD association in young; often surgical indication. |
| Single Coronary Artery | One artery supplies entire heart via branches. | Variable | May be benign or cause ischemia depending on course/distribution. |
| Other Variants | e.g., High/low interarterial, retroaortic, prepulmonic, subpulmonic. | Mostly Benign (except interarterial) | Interarterial = high-risk; others usually low-risk. |
High-risk = interarterial + features like intramural/slits/acute angle.
🩺 Symptoms & Presentation
Symptoms vary widely - many people have none 😴.
- Asymptomatic (most common).
- Exertional chest pain/angina, shortness of breath, fatigue.
- Palpitations, syncope, or arrhythmias.
- In severe cases: myocardial infarction or sudden cardiac arrest ⚡.
- Infants (ALCAPA): poor feeding, sweating, irritability, heart failure signs.
Symptoms often exertion-related; high-risk anomalies worse during intense activity.
🛠️ Diagnostic Investigations
Accurate imaging is key to confirm anomaly, assess course/risk features, and guide management. Echocardiography first-line; advanced imaging essential.
- ECG: Initial screen; may show ischemia/arrhythmias (often nonspecific).
- Echocardiography ❤️: First-line, especially kids; views origin/course; stress echo for ischemia.
- CT Coronary Angiography (CCTA) 📸: Gold standard noninvasive; detailed anatomy, high-risk features (interarterial, intramural); low radiation with modern protocols.
- Cardiac MRI/CMR: No radiation; excellent for anatomy, function, perfusion, scarring; great for follow-up.
- Invasive Coronary Angiography: Reserved for complex cases or pre-intervention; real-time but invasive.
- Exercise Stress Testing: Assess inducible ischemia in active/suspected patients; helps risk-stratify.
(Recent guidelines [2025 ACC/AHA] emphasize CCTA/MRI for detailed evaluation in suspected anomalies.)
💉 Treatment Options
Depends on type, symptoms, ischemia evidence, high-risk anatomy, age, and activity level. Conservative for low-risk; surgery for high-risk/symptomatic.
- Conservative/Medical: Asymptomatic low-risk → observation, risk factor control (BP, lipids), beta-blockers for symptoms; restrict intense sports if uncertain.
- Surgical Correction (preferred for high-risk):
- Reimplantation: Move anomalous artery to correct sinus (common for AAOCA).
- Unroofing: Open intramural segment + neo-ostium creation.
- Other: PA translocation, patch augmentation; CABG rarely (competitive flow issues).
- Lifestyle & Monitoring: Activity restriction (avoid competitive sports if high-risk); regular follow-up imaging/tests; shared decision-making.
Surgery safe/effective in expert centers; relieves symptoms in most.
📈 Outcomes & Prognosis
- Benign anomalies: excellent long-term with monitoring; normal life.
- High-risk (esp. untreated interarterial): risk of SCD, but early detection/surgery dramatically improves outlook.
- Post-surgery: low mortality, symptom relief in >95%; return to activity possible after clearance.
- Individualized: based on anomaly, age, symptoms - specialist (adult congenital/pediatric cardiology) input essential.
🔚 Summary
Anomalous coronary arteries range from harmless variants to life-threatening causes of ischemia/SCD. Early detection via advanced imaging (CCTA/MRI key), risk stratification (high-risk features), and tailored management (surgery for symptomatic/high-risk) save lives - especially in young/active people. Always refer to cardiologist for personalized assessment! 🚀
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
