| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Body Mass Index
Related Subjects: |Malnutrition universal screening tool (MUST) |Body Mass Index |Peripherally inserted central catheters (PICC) |Refeeding syndrome
📖 Introduction
Body Mass Index (BMI) is a quick and widely used screening tool that relates an individual’s weight to their height, providing a numerical estimate of body fat. Although originally designed for population-level epidemiology by Adolphe Quetelet in the 19th century, it remains a key measure in modern clinical practice and public health. It is especially useful for flagging those at risk of undernutrition, overweight, or obesity, all of which carry significant health implications.
🧮 Calculation and Classification
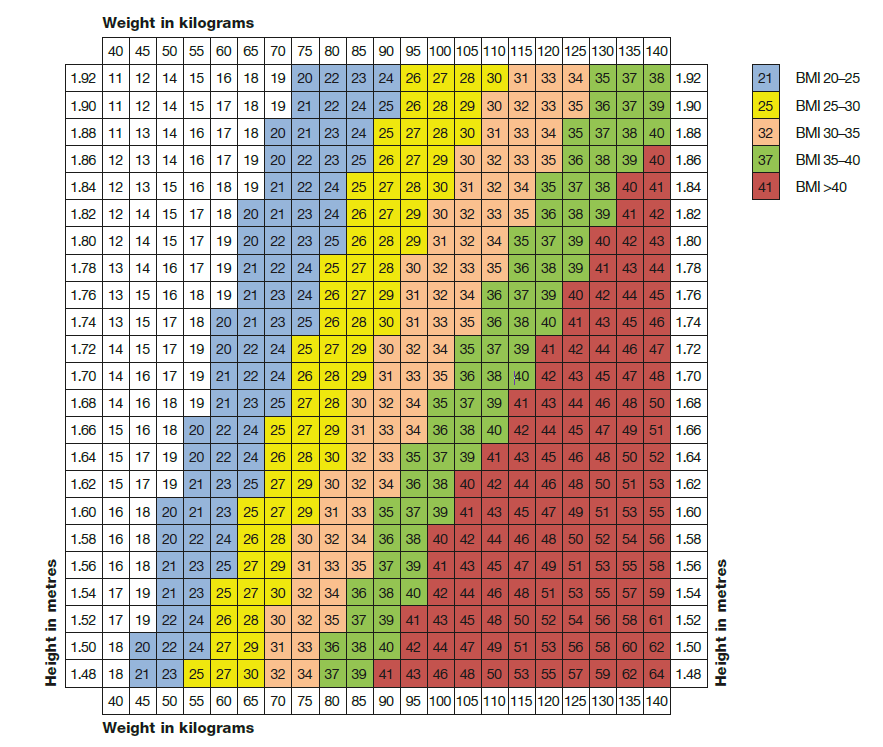
BMI is calculated using the standard formula:
BMI = Weight (kg) / [Height (m)]2
For adults, BMI is classified into categories (WHO/NICE):
- ⚠️ Underweight: <18.5
- ✅ Normal weight: 18.5 – 24.9
- ⚠️ Overweight: 25 – 29.9
- ⬆️ Obesity Class I: 30 – 34.9
- ⬆️ Obesity Class II: 35 – 39.9
- 🚨 Obesity Class III (Morbid obesity): ≥40
🏥 Clinical Significance
- 📊 Screening tool: Provides a rapid overview of nutritional status in both undernutrition and obesity.
- ❤️ Risk stratification: Higher BMI is associated with increased risk of type 2 diabetes, hypertension, cardiovascular disease, stroke, and some cancers.
- 🧩 Monitoring: Useful for following weight changes over time, particularly in patients on weight management programmes or nutritional support.
- 👶 Paediatrics: In children, BMI must be plotted against age- and sex-specific centile charts (UK-WHO growth charts) rather than adult cut-offs.
⚖️ Limitations of BMI
- 💪 Muscle vs fat: BMI does not distinguish lean mass from fat mass, so muscular individuals may appear “overweight.”
- 🧍 Fat distribution: Central obesity (visceral fat) carries more cardiometabolic risk than peripheral fat, but BMI alone cannot capture this.
- 🧓 Age & sex: Elderly patients may have sarcopenia (muscle loss) despite a “normal” BMI. Women generally have higher body fat at the same BMI than men.
- 🌍 Ethnic variation: In South Asian and Chinese populations, health risks occur at lower BMI thresholds → NICE advises using 23 kg/m² as the overweight threshold for these groups.
📌 Alternative / Complementary Measures
- Waist Circumference (WC): Better predictor of central obesity and metabolic syndrome risk. → Risk increased if WC >94 cm (men) or >80 cm (women).
- Waist-to-Height Ratio: >0.5 suggests increased cardiometabolic risk.
- Body Fat %: Measured by bioelectrical impedance or DEXA scanning, gives more accurate assessment of adiposity.
- Clinical context: Combine BMI with blood pressure, lipids, HbA1c, and lifestyle assessment.
🧭 Conclusion
BMI remains a simple, cost-effective, first-line screening tool for assessing nutritional status. However, it should never be used in isolation. Interpreting BMI alongside waist circumference, comorbidities, and demographic factors provides a more accurate picture of health risk. In UK practice, NICE and Public Health England recommend combining BMI with waist measures to guide interventions in obesity and metabolic risk.
📚 References
- NICE CG189: Obesity Identification, Assessment and Management
- WHO – Obesity and Overweight
- Public Health England. Adult Obesity: Applying All Our Health.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
