| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Graves Disease (Thyrotoxicosis) ✅
Related Subjects: |Thyrotoxicosis and Hyperthyroidism |Thyroid Storm - Thyrotoxic crisis |Graves' Disease (Thyrotoxicosis) |Amiodarone and Thyroid disease |Thyroid Surgery (Thyroidectomy) |Hypothyroidism |Hashimoto's thyroiditis |DeQuervain's thyroiditis |Subacute Thyroiditis |Thyroid nodule |Congenital Hypothyroidism |Thyroid Function Tests and antibodies |Post partum thyroiditis |Sick Euthyroid Syndrome |Thyroid Exam (OSCE) |Thyroid Gland anatomy and Physiology |Thyroid Cancer
⚠️ Smokers with Graves' Disease have a significantly higher risk of developing thyroid eye disease (TED). Smoking cessation is essential to reduce complications and improve outcomes. 💨
📖 About
- Autoimmune disease: Graves’ disease is the most common cause of hyperthyroidism (60–80% of cases).
- Leading cause of thyrotoxicosis in the UK and worldwide.
- Immune-mediated stimulation of TSH receptors drives thyroid hormone overproduction.
🔎 Risk Factors
- Gender: Women >> Men (~10:1).
- Age: Typically 30–50 years.
- Postpartum: Increased risk in first 6–12 months.
- Smoking: Major modifiable risk factor for TED; worsens severity and prognosis.
- Family history: Genetic predisposition via HLA-B8, DR3.
🧬 Pathophysiology & Aetiology
- TSH receptor antibodies (TRAb): Stimulate follicular hyperplasia, ↑ T3/T4 production; cross placenta → neonatal thyrotoxicosis.
- Thyroid peroxidase antibodies (TPOAb): Present in ~80%.
- Orbital fibroblast activation: Glycosaminoglycan deposition → proptosis, diplopia, orbital oedema.
- Autoimmunity can be triggered by infections, stress, or iodine exposure.
🩺 Clinical Presentation
- Symptoms: Weight loss, heat intolerance, palpitations, anxiety, tremor, diarrhoea.
- Elderly: May present with apathetic thyrotoxicosis – fatigue, anorexia, atrial fibrillation.
- Examination: Diffuse, smooth goitre with bruit/thrill, tremor, warm moist skin, tachycardia, hyperreflexia.
🌟 Specific Signs
- Thyroid Eye Disease (TED): Lid lag, lid retraction, proptosis, diplopia, corneal ulceration (~40% of patients).
- Pretibial myxoedema: Non-pitting, pink-orange plaques (~5%).
- Thyroid acropachy: Rare clubbing with onycholysis.
🔬 Investigations (NICE & ATA Guidelines)
- Thyroid function tests: ↑Free T4/T3, suppressed TSH (<0.05 mIU/L).
- TRAb: Confirms autoimmune aetiology; predicts risk of TED.
- Radionuclide uptake scan: Diffuse uptake in Graves’, distinguishes from toxic adenoma/multinodular goitre.
- Thyroid ultrasound: Optional; evaluates nodularity.
- Ophthalmology assessment: Baseline visual acuity, colour vision, intraocular pressure, exophthalmometry for TED severity.
🧾 Differentials
- Toxic multinodular goitre
- Toxic adenoma
- Exogenous thyroxine excess
- Subacute thyroiditis (painful, self-limiting)
⚕️ Management (NICE & ATA/ETA Guidance)
- Symptom control: Beta-blockers (propranolol 20–40 mg QDS) for palpitations, tremor, anxiety.
- Antithyroid drugs (ATDs): Carbimazole first-line (20–40 mg daily titrated), propylthiouracil reserved for pregnancy or intolerance.
- Radioiodine therapy: Avoid in active TED, particularly smokers; may worsen ophthalmopathy.
- Surgery: Subtotal or total thyroidectomy for severe, compressive, or refractory disease.
- Atrial fibrillation: Consider anticoagulation per CHA₂DS₂-VASc; monitor for hyperthyroid-related cardiomyopathy.
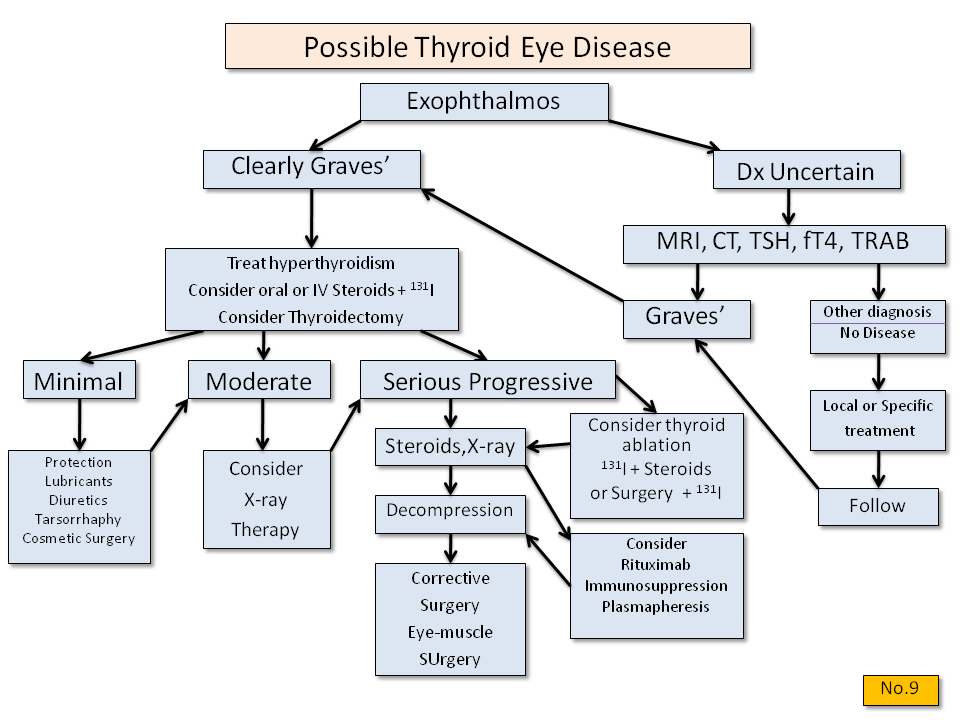
👁️ Thyroid Eye Disease (TED) Management
- Initial muscle involved: Inferior rectus → restricted upgaze.
- Smoking cessation: Most important modifiable factor.
- Ophthalmology referral: Monitor acuity, optic nerve function, intraocular pressure.
- Conservative: Lubricants, eyelid taping, head elevation, selenium supplementation if mild.
- Medical therapy: IV/oral glucocorticoids (prednisolone 60 mg), immunomodulators (ciclosporin, rituximab, teprotumumab where available).
- Advanced: Orbital radiotherapy or surgical decompression in sight-threatening disease.
💡 Exam Tips
• Hyperthyroid patient who smokes → always ask about eye symptoms; early TED referral improves prognosis.
• TRAb positive → confirms Graves’ and risk stratification for TED.
• Active TED = contraindication to radioiodine therapy.
• Diffuse goitre with bruit → hallmark on palpation.
• Pretibial myxoedema or acropachy → pathognomonic but rare.
📚 References
- NICE NG145: Thyroid disease – assessment and management
- ATA Guidelines: 2016 Hyperthyroidism Management
- ETA/Endocrine Society: Thyroid Eye Disease Guidelines
- Ross DS, et al. 2016. American Thyroid Association Guidelines for Diagnosis and Management of Hyperthyroidism and Other Causes of Thyrotoxicosis. Thyroid. 26(10):1343–1421.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
