| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Internal; Decapitation
Related Subjects: |Transverse myelitis |Acute Disseminated Encephalomyelitis |Cervical spondylosis |Spinal Cord Anatomy |Acute Disc Prolapse |Spinal Cord Compression |Spinal Cord Haematoma |Foix-Alajouanine syndrome |Cauda Equina |Conus Medullaris syndrome |Anterior Spinal Cord syndrome |Central Spinal Cord syndrome |Brown-Sequard Spinal Cord syndrome |Internal Decapitation
🚨 Internal decapitation usually refers to traumatic atlanto-occipital dissociation (AOD) — severe instability between the occiput (skull base) and C1/C2. Although the skin remains intact, the ligamentous attachments between the head and upper cervical spine are critically disrupted. This is a neurosurgical / spinal emergency with high mortality and risk of immediate respiratory arrest, lower cranial nerve injury, and tetraparesis.
🧠 Definition
- Atlanto-occipital dissociation (AOD) = loss of normal stability between the skull and cervical spine at the craniovertebral junction.
- It is often called “internal decapitation” in lay language because the head is effectively detached from the spine internally, even though there is no external separation.
- The injury may involve ligamentous rupture, capsular disruption, bony injury, or a combination.
🦴 Relevant Anatomy
- The occipital condyles articulate with the superior facets of C1 (atlas).
- Stability depends heavily on the tectorial membrane, alar ligaments, apical ligament, joint capsules, and supporting soft tissues.
- The nearby structures at greatest risk are the medulla / lower brainstem, upper cervical spinal cord, and vertebral arteries.
⚡ Mechanism
- Usually follows high-energy blunt trauma such as road traffic collisions, major falls, or severe sports trauma.
- Mechanisms include combinations of hyperextension, distraction, rotation, and lateral bending.
- Children are relatively more vulnerable because of a larger head-to-body ratio, shallower joints, and greater ligamentous laxity.
👀 Clinical Features
- Presentation ranges from immediate death to survival with neck pain alone.
- Possible features: reduced GCS, apnea, quadriparesis, cranial nerve deficits, severe neck pain, torticollis, or cardiorespiratory instability.
- Some patients can initially appear neurologically intact, so a normal first examination does not exclude this injury.
🚩 Red Flags
- High-speed trauma with major head/face injury.
- Persistent severe upper neck pain after high-energy mechanism.
- Lower cranial nerve signs, respiratory compromise, or unexplained neurological findings.
- Marked prevertebral swelling or abnormal craniocervical alignment on imaging.
🩻 Diagnosis
- CT cervical spine is the key first-line imaging test in major trauma and is central to diagnosis.
- MRI is useful for showing ligamentous disruption, cord injury, and soft-tissue damage, especially when suspicion remains despite equivocal CT findings.
- Plain radiographs are less reliable than modern CT, and subtle injuries can be missed.
📏 Imaging Measurements Often Used
- Basion-dens interval (BDI): abnormal if enlarged; CT-based thresholds are commonly used to suggest AOD.
- Basion-axial interval (BAI): another alignment measure that may be abnormal in dissociation.
- Powers ratio: historically described, but relatively insensitive compared with modern CT-based measures.
- Condyle-C1 interval (CCI): particularly useful, especially in paediatric assessment, for detecting occipito-atlantal malalignment.
💥 Associated Injuries
- Traumatic brain injury.
- Upper cervical cord injury.
- Vertebral artery injury.
- Facial fractures, skull base trauma, and other cervical spine injuries.
🆘 Emergency Management
- Manage using ATLS principles: airway, breathing, circulation, disability, exposure.
- Maintain strict cervical spine precautions with minimal neck movement.
- Early involvement of major trauma, spinal surgery, and neurosurgery teams is essential.
- Avoid cervical traction in suspected traumatic AOD because distraction can worsen the injury.
🔧 Definitive Treatment
- Most survivors with true traumatic AOD require operative stabilisation, usually occipitocervical fusion.
- External immobilisation alone is generally not considered reliable definitive treatment for classic unstable AOD in adults.
- Selected unusual cases may be managed differently in specialist centres, but this is not routine practice.
📉 Prognosis
- Historically, AOD carried an extremely high mortality because of brainstem and high cervical cord injury.
- Outcomes are improving with better prehospital care, rapid CT diagnosis, and earlier operative stabilisation.
- Neurological outcome depends heavily on the severity of the initial neural injury and whether cardiorespiratory arrest occurred at the scene.
🧪 Pathophysiology
- The occiput–C1–C2 complex acts as the mechanical bridge between the skull and the rest of the spine.
- When the major stabilising ligaments fail, the skull can translate abnormally relative to the atlas and axis.
- Because the medulla and upper cervical cord sit immediately behind this junction, even small displacements can cause catastrophic neuro-respiratory collapse.
- This is why some patients die at the scene, while survivors may still deteriorate rapidly if the injury is missed or the neck is moved excessively.
🎓 Exam Pearls
- Internal decapitation = traumatic atlanto-occipital dissociation in most trauma contexts.
- Think of it after high-energy trauma with severe upper neck injury.
- CT first, MRI for ligaments/cord.
- Do not use traction in suspected AOD.
- Definitive treatment in survivors is usually occipitocervical fusion.
⚠️ Common Pitfalls
- Being falsely reassured by an initially normal neurological examination.
- Relying on a single old radiographic measurement rather than overall CT assessment of the craniovertebral junction.
- Missing the injury in a patient with severe head trauma where the neck is not assessed carefully.
- Using traction in an unstable dissociation injury.
📝 One-Line Summary
- Internal decapitation is a catastrophic craniocervical instability injury — suspect it after high-energy trauma, diagnose it urgently with CT ± MRI, avoid traction, and treat survivors with specialist stabilisation.
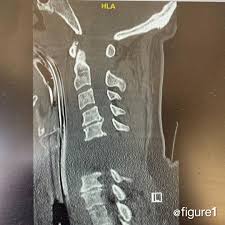
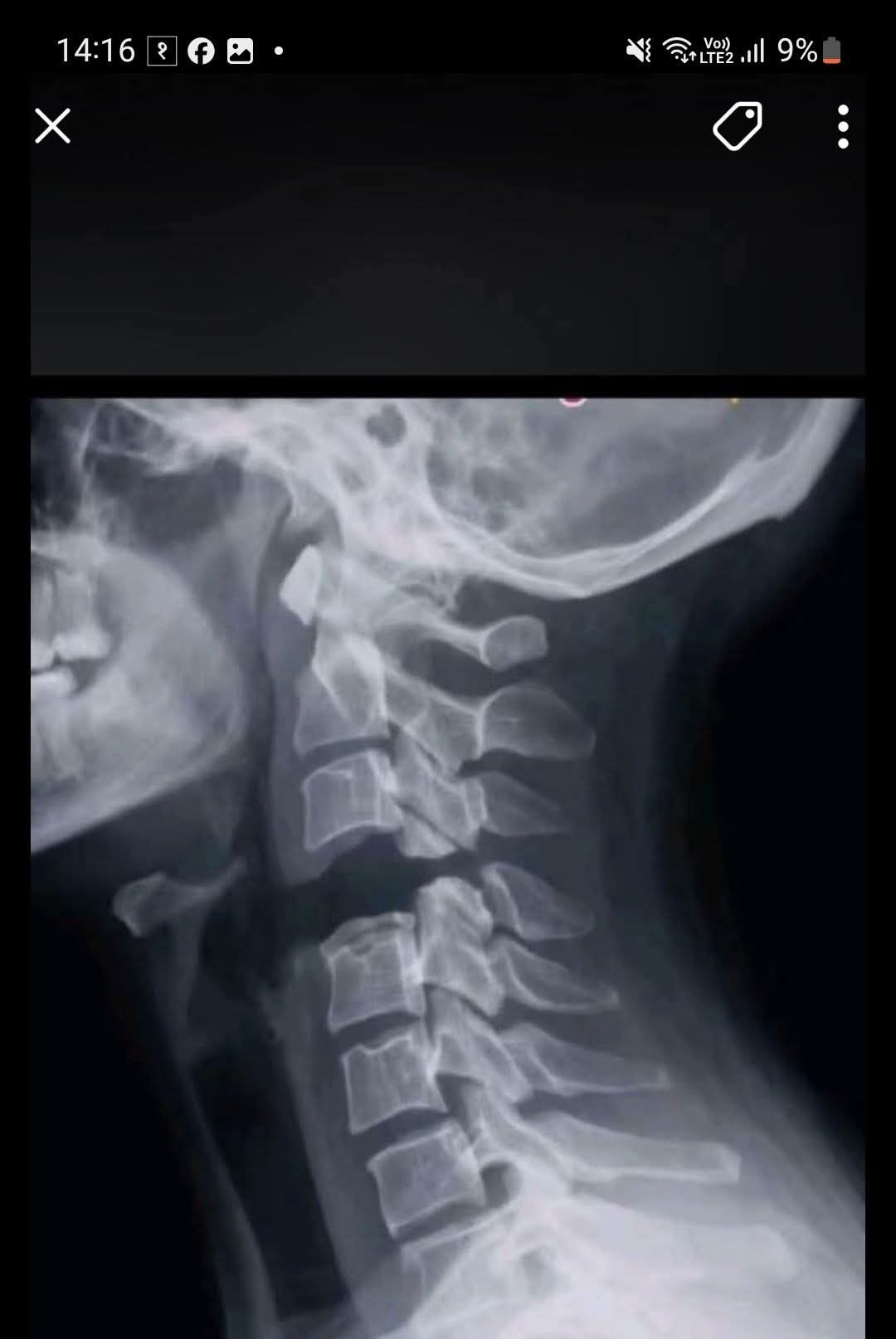
A few practical teaching points: this injury is dangerous because it is primarily a ligament failure problem, so the CT may show subtle malalignment rather than an obvious dramatic fracture, which is why clinicians must actively inspect the craniovertebral junction rather than just looking for broken bones. The terminology can be confusing: atlanto-occipital dissociation/dislocation is the standard medical term, while “internal decapitation” is mostly a lay or media phrase. In adults, enlarged BDI/BAI and abnormal occiput–C1 alignment on CT are important clues, while MRI adds value when ligament injury is suspected or neurological findings do not match the CT appearance.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
