| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Seborrheic Dermatitis
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
📖 About
- Seborrhoeic Dermatitis is a chronic, relapsing skin condition caused by an abnormal inflammatory response to skin yeasts (especially Malassezia species).
- It is common, affecting up to 5% of adults, and is usually mild but can be distressing due to itching and cosmetic impact.
- Antifungal creams and medicated shampoos are the mainstay of long-term management and are safe for repeated use.
🧬 Aetiology
- Strongly associated with the yeast Pityrosporum ovale (Malassezia), which thrives in sebaceous (oily) areas.
- More severe in patients with Parkinson’s disease and HIV, due to altered immune responses.
- May also be worsened by genetic susceptibility, environmental stress, or cold weather.
👀 Clinical Features
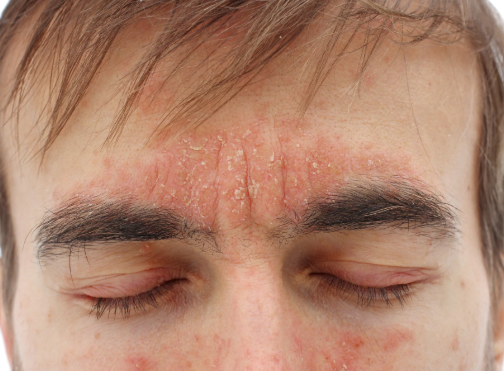
- Dry, scaly, flaky rash with erythema, often itchy.
- Commonly affects:
- Eyebrows & nasolabial folds
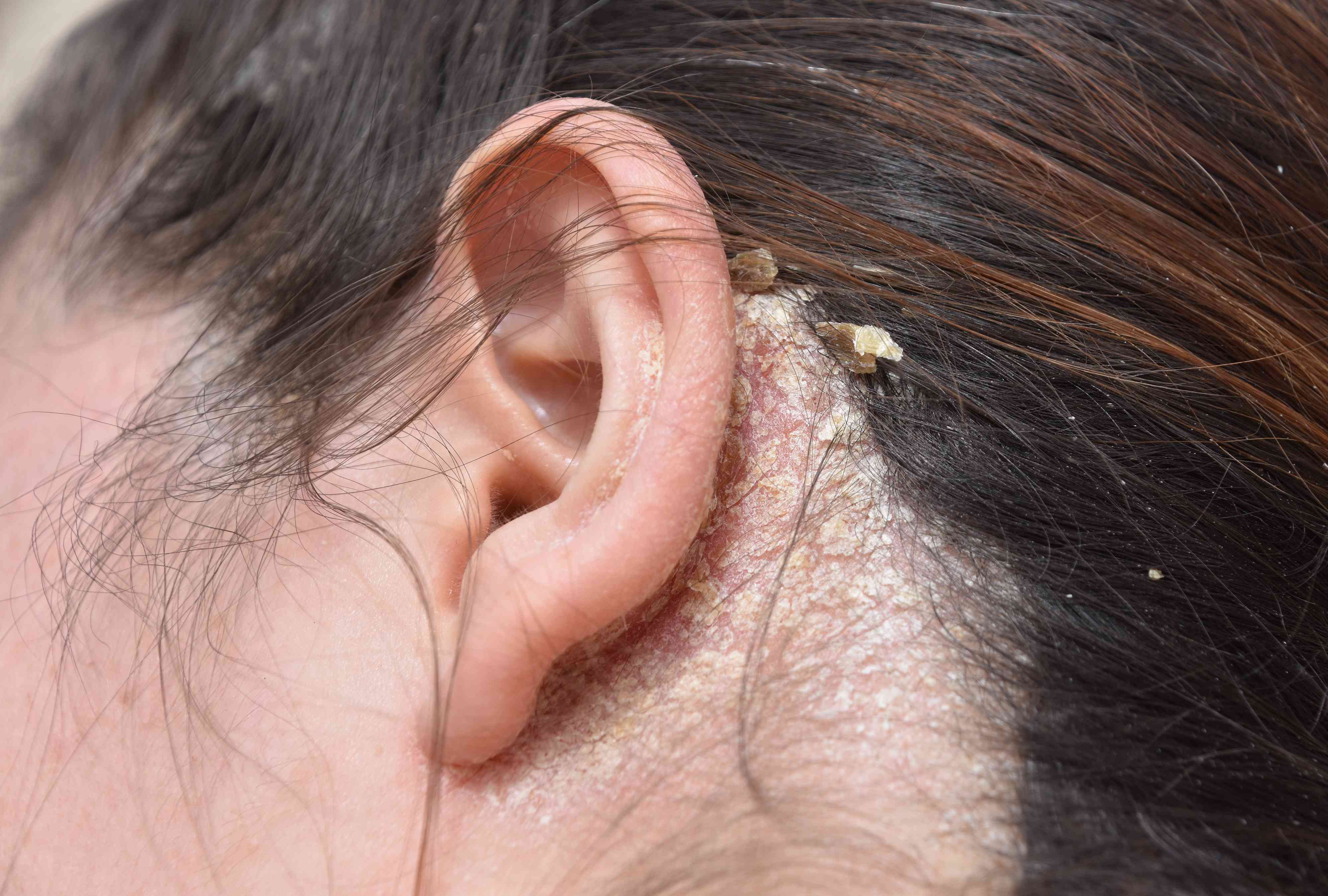
- External ears & ear canals
- Scalp (dandruff or thick crusting)
- Chest and sternum
- Worsens in stress or winter.
- Unilateral distribution may occur in stroke patients due to altered skin innervation.
🔗 Associations
- Parkinson’s disease – thought to relate to autonomic dysfunction and excess sebum production.
- HIV infection – often more severe, refractory, and widespread.
- Stroke – can affect the scalp unilaterally on the side of neurological deficit.
🧪 Investigations
- Diagnosis is clinical, based on rash distribution and appearance.
- Skin scrapings/mycology if tinea capitis suspected.
- HIV testing if seborrhoeic dermatitis is severe or atypical.
🩺 Differential Diagnosis
- Psoriasis – thicker, silvery-white scales; usually spares the face.
- Tinea capitis – patchy hair loss, positive fungal microscopy.
- Atopic dermatitis – flexural distribution, more pruritic.
- Contact dermatitis – clear exposure trigger.
💊 Management
- General: Chronic relapsing course, requires maintenance therapy.
- Scalp:
- Anti-dandruff shampoos: ketoconazole, selenium sulphide, or zinc pyrithione.
- Leave shampoo on for 5–10 minutes before rinsing.
- Descaling: coconut oil or salicylic acid overnight for thick crusts.
- Short-term mild steroid scalp lotion/gel for inflamed cases.
- Face/Body:
- Topical antifungals: clotrimazole, miconazole, ketoconazole.
- Short course of mild topical steroids if significant erythema.
- Moisturisers to reduce scaling and redness.
- Ear canals: Medicated antifungal/steroid eardrops; avoid cotton buds.
- Eyelids: Gentle cleansing with diluted baby shampoo or eyelid wipes.
- Refractory/widespread cases: Short oral antifungal course (e.g., itraconazole) may be considered.
- Maintenance: Weekly antifungal shampoo once clear.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
