| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Psoriatic arthritis ✅
Related Subjects: |Monoarticular arthritis |Polyarticular arthritis |Seronegative Spondyloarthropathies |Ankylosing spondylitis |Enteropathic Spondyloarthritis |Reactive Arthritis
🦴 Psoriatic Arthritis (PsA) is a chronic inflammatory arthritis associated with psoriasis. It is part of the seronegative spondyloarthropathies (negative for RF/anti-CCP). Presentation ranges from mild oligoarthritis to severe, deforming arthritis (arthritis mutilans). ⚠️ Severe PsA is more common in HIV-positive patients. Early recognition and prompt treatment prevent irreversible joint damage and disability.
📊 Overview
- Seronegative arthritis (RF/anti-CCP negative).
- Psoriasis usually precedes arthritis but PsA can rarely precede skin lesions.
- Affects both peripheral joints and axial skeleton (sacroiliac joints, spine).
- Equal sex distribution; peak age 30–55 yrs.
🧬 Aetiology & Pathophysiology
- Genetic: HLA-B27 (axial disease), HLA-Cw6 (skin involvement).
- Immune-mediated: T-cell and cytokine-driven (TNF-α, IL-17, IL-23).
- Triggers: Trauma (Koebner phenomenon), infection, environmental factors.
- Pathophysiology: Enthesitis → synovitis → bone erosion and proliferation → characteristic deformities.
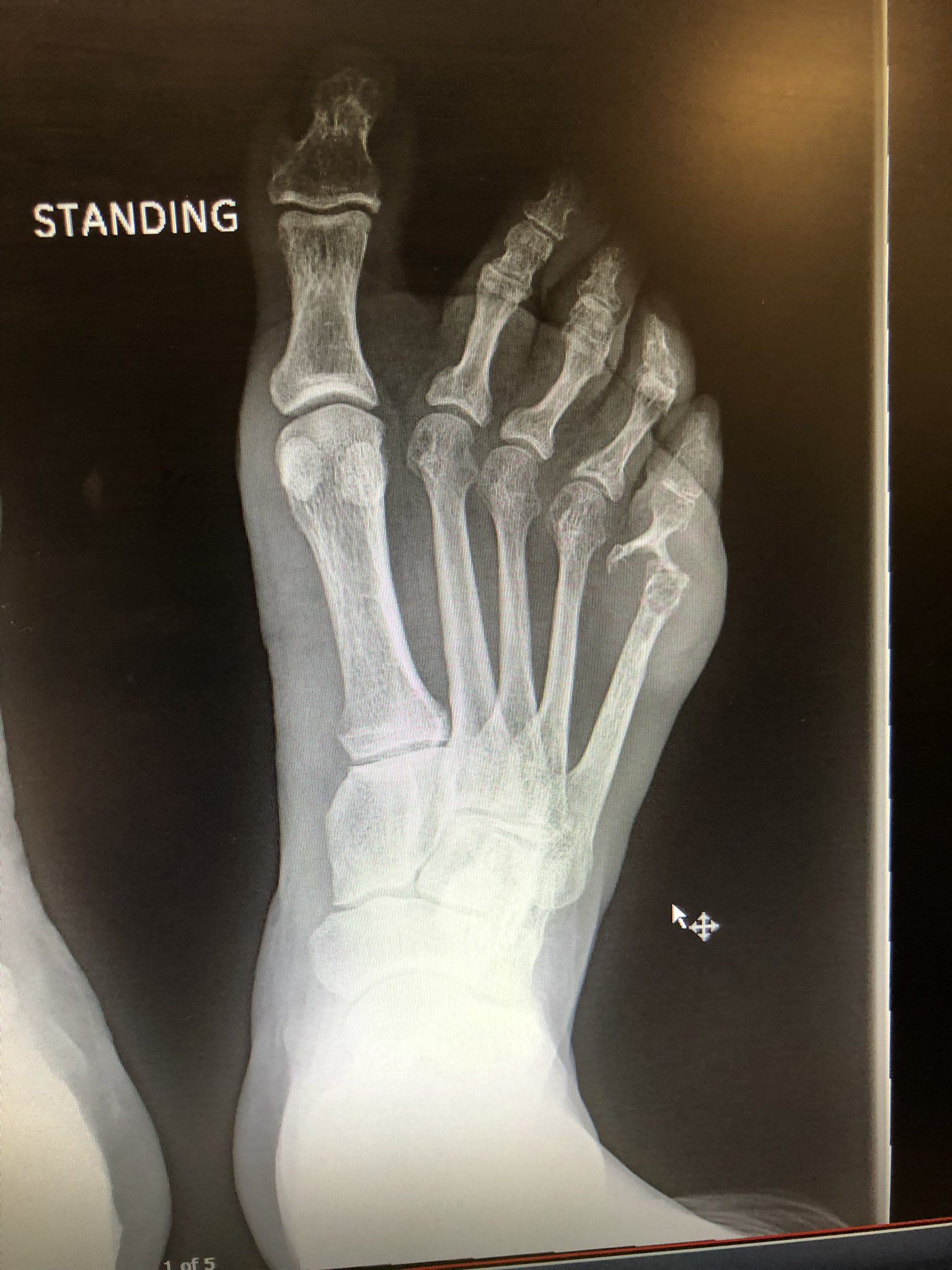
🔎 Key Radiological Feature
🖊️ Pencil-in-Cup Deformity: distal bone tapering into adjacent bone cup, classic of advanced PsA.
🩺 Clinical Features
- Skin 🖐️: Psoriasis on scalp, elbows, knees, umbilicus, natal cleft, palms/soles.
- Nails 💅: Pitting, onycholysis, “oil drop” sign.
- Joints:
- Asymmetrical oligoarthritis (most common).
- Symmetrical polyarthritis (RA-like).
- DIP arthritis often with nail involvement.
- Dactylitis = “sausage digit”.
- Arthritis mutilans → destructive, deforming joints.
- Axial disease → sacroiliitis, spinal stiffness, enthesitis.
- Extra-articular 🌍: Anterior uveitis, conjunctivitis, pulmonary fibrosis, aortic regurgitation.
📌 Patterns of Joint Involvement
- DIP predominant (linked to nail disease) 👆
- Asymmetrical oligoarthritis (knees, large joints) ✋
- Symmetrical polyarthritis (mimics RA) 🤲
- Arthritis mutilans (rare, severe) 🦴
- Axial arthritis (sacroiliitis, spine) 🧍
🧾 CASPAR Classification Criteria (≥3 points)
- Psoriasis: current = +2, past/family = +1
- Nail dystrophy (pitting/onycholysis) = +1
- Dactylitis (past or present) = +1
- RF negative = +1
- Juxta-articular new bone formation on X-ray = +1
🧪 Investigations
- Bloods: FBC (may show anaemia of chronic disease), ESR/CRP ↑, RF/anti-CCP negative.
- Imaging:
- X-ray: erosions, joint narrowing, periostitis, bony proliferation, pencil-in-cup deformity.
- MRI: early axial disease, sacroiliitis, enthesitis.
- Ultrasound: synovitis, tenosynovitis, and enthesitis detection.
💊 Management (NICE-aligned, Treat-to-Target)
- Principle: Early intervention prevents joint destruction. Tailor therapy to dominant phenotype (peripheral, axial, enthesitis, dactylitis, skin).
- 🟢 Lifestyle & Supportive:
- Patient education, shared decision-making.
- Weight management (obesity reduces biologic efficacy).
- Smoking cessation.
- Physiotherapy and occupational therapy for joint function.
- 🟡 Symptomatic Relief:
- NSAIDs for pain/stiffness (monitor CV/GI risk).
- Intra-articular steroid injections for isolated joints.
- Systemic steroids cautiously (risk of psoriasis rebound).
- 🟠 Conventional DMARDs (peripheral arthritis):
- Methotrexate – first-line for peripheral arthritis and skin disease.
- Sulfasalazine or Leflunomide – alternatives.
- Limited efficacy for axial disease.
- 🔵 Biologic / Targeted Therapy (moderate–severe or DMARD-refractory):
- Anti-TNF agents (etanercept, adalimumab, infliximab)
- IL-17 inhibitors (secukinumab, ixekizumab)
- IL-23 inhibitors (guselkumab)
- JAK inhibitors (upadacitinib) in selected patients
- 🔴 Axial PsA:
- NSAIDs first-line.
- Persistent disease → biologics (anti-TNF or IL-17 inhibitors).
- Conventional DMARDs usually ineffective.
- Monitoring & Screening:
- Regular assessment of joint and skin disease activity.
- Screen for uveitis, inflammatory bowel disease, cardiovascular risk, metabolic syndrome.
- Adjust therapy per treat-to-target principles (low disease activity or remission).
- Surgical: Synovectomy or joint replacement in advanced destructive disease.
💡 Student Tips
- Remember: PsA = seronegative, often with nail changes and dactylitis.
- Pencil-in-cup deformity is classic for exam radiology questions.
- Assess for axial involvement separately – different management pathway.
- Always consider comorbidities: CV risk, metabolic syndrome, IBD, HIV.
📚 References
- NICE CKS – Psoriatic Arthritis
- Psoriatic Arthritis: A Review
- EULAR 2023 Recommendations: EULAR Management of PsA
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
