| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Moyamoya disease
Related Subjects: |Subarachnoid Haemorrhage |Haemorrhagic stroke
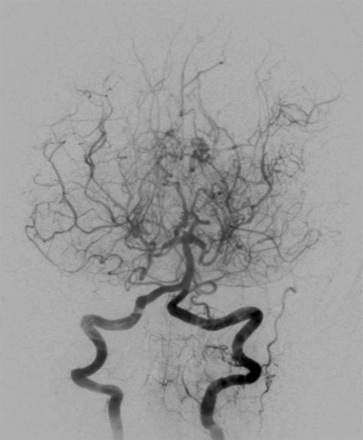
🌫️ Moyamoya disease is a progressive, non-inflammatory vasculopathy affecting the intracranial internal carotid arteries (ICA), middle cerebral arteries (MCA), and anterior cerebral arteries (ACA). It causes both ischaemic and haemorrhagic stroke. On angiography, a hazy network of collateral vessels forms, resembling "moyamoya" - the Japanese word for smoke drifting in the air. First described in 1957, the name was popularised by Jiro Suzuki in 1965 and later codified [Suzuki J, 1983].
📖 About
- Described in Japan in 1957 as “hypoplasia of the bilateral ICAs”; renamed “Moyamoya” in 1965.
- 🧮 Incidence: ~10/100,000 in Japan; ~1/1,000,000 in the USA.
- Involves progressive ICA occlusion and development of fragile collateral vessels.
- Increased basic fibroblast growth factor has been implicated in pathogenesis.
- Can be sporadic or familial, leading to both ischaemic and haemorrhagic stroke.
🧬 Genetics
- Most common in Japanese, Chinese, and Korean populations (10x more frequent than in Europeans).
- Familial clustering: linked to variants on chromosome 17 (e.g., RNF213 gene).
- Seen worldwide, including non-Asian cohorts.
⚙️ Aetiology & Pathophysiology
- Affects the distal ICA, MCA, and ACA stems.
- Results in extensive collateralisation via lenticulostriate, thalamic, and transdural anastomoses.
- Non-inflammatory; pathology shows intimal hyperplasia with lumen narrowing.
- Fragile collaterals predispose to haemorrhage.
- Similar angiographic patterns (“Moyamoya syndrome”) may occur with atherosclerosis, diabetes, or sickle cell disease.
🤝 Associations
- Haematological: Sickle cell disease, β-thalassaemia, hereditary spherocytosis, Fanconi anaemia.
- Neurological/genetic: Neurofibromatosis type 1.
- Metabolic/immune: Homocystinuria, antiphospholipid syndrome, Grave’s disease, SLE.
🩺 Clinical Presentation
- Common in children/young adults, but may present at any age.
- ⛔ Ischaemic events: recurrent hemiplegia, TIAs, cognitive impairment, silent infarcts.
- ⚡ Seizures and movement disorders (chorea, dystonia) may occur.
- 💥 Haemorrhage: intraparenchymal or intraventricular bleed from fragile collaterals.
🔍 Investigations
- 🧪 Bloods: Usually normal; confirms non-inflammatory nature.
- 🖼️ CT: Cortical/subcortical infarcts, volume loss, haemorrhage.
- 🧲 MRI/MRA: Gold standard → ICA narrowing + “puff of smoke” collaterals. FLAIR: “Ivy sign” from slow cortical flow. GRE: Detects microhaemorrhages in basal ganglia/thalamus.
- 📡 Transcranial Doppler: Non-invasive assessment of stenosis/hemodynamics.
- ⚡ EEG: In children → “re-build-up phenomenon” after hyperventilation.
- 🩻 Perfusion imaging: Identifies hypoperfused territories at risk of infarct.
📊 Suzuki Angiographic Stages
- 1️⃣ Early ICA stenosis.
- 2️⃣ Development of Moyamoya collaterals at brain base.
- 3️⃣ Progressive ICA occlusion; ↑ collateral vessels, ↓ MCA/ACA flow.
- 4️⃣ Circle of Willis + PCA occlusion; extracranial–intracranial collateralisation.
- 5️⃣ Fewer Moyamoya vessels; major arteries absent.
- 6️⃣ Disappearance of Moyamoya collaterals; brain perfused only by ECA branches.
⚖️ Management
- Best managed in specialist neurosurgical centres.
- 📉 Medical therapy: Limited role. BP optimisation crucial. Antiplatelets are sometimes used in children but avoided in adults due to haemorrhage risk.
- 🧑⚕️ Surgical revascularisation: - Direct bypass: STA–MCA anastomosis. - Indirect: Encephaloduroarteriosynangiosis (EDAS), burr holes, encephalomyosynangiosis (EMS). Recent studies show direct bypass reduces haemorrhagic risk most effectively.
- 💊 Aspirin often used in children; usually stopped in adults due to bleed risk.
- 📉 Most common cause of death: haemorrhage from fragile collaterals.
📖 Further Reading
- Moyamoya Disease and Syndrome - NEJM, 2009
- Treatment and Outcomes in Moyamoya - J Stroke, 2016
- EEG findings in childhood Moyamoya - Neurosurg Rev, 1992
- MRI vs CT perfusion in Moyamoya - Sichuan Univ J Med, 2018
- Multiple burr hole surgery - Acta Neurochir, 2018
💡 Exam Pearl: Moyamoya = young patient + recurrent TIAs/strokes + angiogram “puff of smoke.” Think early referral for surgical revascularisation to prevent ischaemia and haemorrhage.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
