| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Renal cell carcinoma ✅
Related Subjects: |Urothelial tumour s |Haematuria |Acute Urinary Retention |Anuria and Oliguria |Bladder cancer |Renal cell carcinoma |Benign Prostatic Hyperplasia |IgA nephropathy |Prostate Cancer |Henoch-Schonlein purpura |Glomerulonephritis
🔎 About Renal Cell Carcinoma (RCC)
- 🧬 Renal cell carcinoma (RCC) is the most common primary kidney cancer in adults, accounting for ~90% of renal malignancies.
- 👨🦳 Typically occurs in people aged 50–70 years and is around 2–3× more common in males.
- 🩺 Many cases are now detected incidentally on imaging performed for unrelated reasons.
- 📈 Incidence has increased with widespread use of abdominal CT and ultrasound.
🧬 Aetiology
- Genetic Syndromes
- 🧩 Von Hippel–Lindau (VHL) syndrome – mutation of the VHL tumour suppressor gene → predisposition to clear cell RCC.
- 🧬 Hereditary papillary RCC – autosomal dominant mutation affecting MET proto-oncogene.
- 🧬 Birt-Hogg-Dubé syndrome – folliculin gene mutation.
- 🧬 Hereditary leiomyomatosis and RCC – fumarate hydratase mutation.
- Lifestyle Factors
- 🚬 Smoking – strongest modifiable risk factor.
- ⚖️ Obesity – increased risk due to metabolic and hormonal effects.
- Medical Conditions
- 📈 Hypertension
- 🩺 Chronic kidney disease
- 🩸 Long-term dialysis and acquired cystic kidney disease
- Occupational Exposures
- 🏭 Heavy metals (e.g. cadmium)
- 🏭 Industrial solvents and dyes
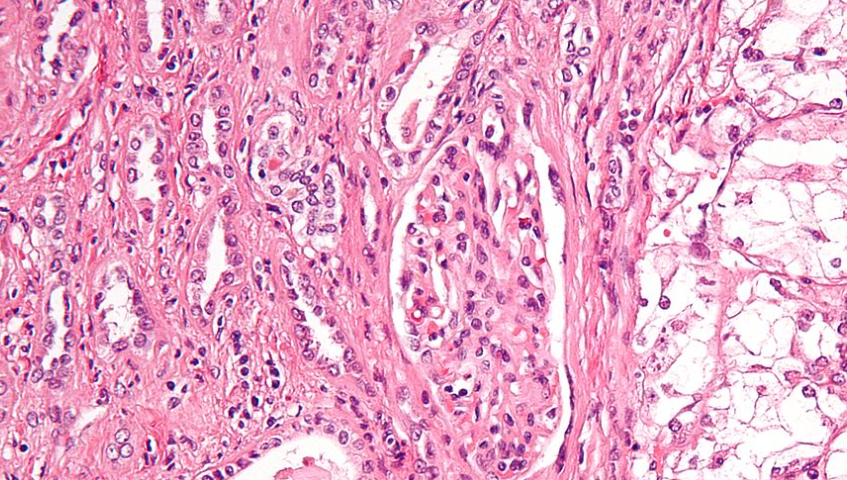
🧫 Histology
- RCC arises from the renal tubular epithelium.
- 📊 Major subtypes:
- Clear cell RCC (~75–80%) – most common and often associated with VHL mutation.
- Papillary RCC (~10–15%).
- Chromophobe RCC (~5%).
- 🧬 Tumours may invade renal veins and the inferior vena cava.
⚠️ Risk Factors
- 👨 Male sex
- 🚬 Smoking
- ⚖️ Obesity
- 📈 Hypertension
- 🩺 CKD and long-term dialysis
- 🧬 Genetic syndromes
- 🩸 Acquired cystic kidney disease
🩺 Clinical Features
- Classic triad (rare): 🩸 haematuria, flank pain, palpable abdominal mass.
- 📉 Constitutional symptoms: weight loss, fatigue, fever.
- 🍇 Left-sided varicocele (compression of left testicular vein).
- 🩸 Paraneoplastic syndromes:
- Polycythaemia (↑ erythropoietin)
- Hypercalcaemia (PTH-related peptide)
- Hypertension (renin secretion)
- Non-metastatic hepatic dysfunction (Stauffer syndrome)
- 🌍 Metastatic spread commonly to lungs, bones, liver, brain.
- 🫀 Tumour may extend into renal vein → inferior vena cava → right atrium.
🔍 Investigations
- 💉 Urinalysis: haematuria
- 📊 Blood tests: FBC, U&E, calcium, LFTs
- Imaging
- 🖥️ Ultrasound – may detect a renal mass.
- 🖼️ Contrast CT (renal protocol) – main diagnostic and staging investigation.
- 🧲 MRI – useful if venous invasion suspected or CT contraindicated.
- 🫁 CT chest for metastatic staging.
- 🧪 Renal tumour biopsy may be performed if systemic therapy is planned or diagnosis uncertain.
💡 Key concept: Many RCCs are now discovered incidentally on CT scans. Early-stage tumours are often asymptomatic and potentially curable with surgery.
🛠️ Management (UK Practice)
- General Measures
- 🚭 Smoking cessation
- ⚖️ Weight management
- 🩺 Optimisation of cardiovascular risk factors
- Surgical Treatment (Preferred for Localised Disease)
- 🔪 Partial nephrectomy – nephron-sparing surgery for small tumours (T1).
- ⚡ Radical nephrectomy – removal of kidney ± adrenal ± lymph nodes if larger or invasive tumour.
- Ablative Therapies
- 🔥 Radiofrequency ablation
- ❄️ Cryoablation
- Used for small tumours in patients unsuitable for surgery.
- Systemic Therapy (Metastatic Disease)
- 🛡️ Immune checkpoint inhibitors (e.g. nivolumab, pembrolizumab, ipilimumab)
- 🎯 Tyrosine kinase inhibitors (VEGF inhibitors) (e.g. sunitinib, pazopanib, cabozantinib)
- ⚡ Combination therapy often used first-line (e.g. immunotherapy + TKI).
- Radiotherapy
- 🎯 Primarily palliative for bone or brain metastases.
📊 Prognosis
- 📍 Localised disease → ~60–75% 5-year survival.
- 🌍 Metastatic disease → significantly lower survival.
- Outcome depends strongly on stage at diagnosis.
🩺 Case 1 – Localised RCC
A 58-year-old smoker presents with intermittent painless haematuria. CT scan shows a 5.2 cm enhancing upper-pole renal mass without metastases. Management: nephron-sparing partial nephrectomy. Post-operative follow-up includes surveillance CT imaging and renal function monitoring.
🩺 Case 2 – Metastatic RCC
A 72-year-old patient presents with weight loss, bone pain and hypercalcaemia. CT demonstrates an 8 cm renal mass with lung metastases. Management: systemic therapy with immune checkpoint inhibitor + VEGF-targeted therapy. Palliative radiotherapy may be used for symptomatic bone metastases.
📚 References
- NICE Kidney Cancer Guidance
- European Association of Urology (EAU) Guidelines
- American Cancer Society Kidney Cancer Resources
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
